For millions of people managing diabetes or prediabetes, the daily struggle to stabilize glucose levels often feels like a game of whack-a-mole. While diet and medication are the primary pillars of care, the timing of physical activity may be the missing variable in achieving tighter glycemic control. Emerging research suggests that the best time of day for exercise to lower blood sugar is not a one-size-fits-all answer, but rather a strategic window that aligns with the body’s natural metabolic rhythms.
The core of the issue lies in postprandial glucose spikes—the surge in blood sugar that occurs after eating. When muscles contract during exercise, they can take up glucose from the bloodstream even without the assist of insulin. By timing a workout to coincide with the peak of these spikes, individuals can effectively “blunt” the rise in blood sugar, leading to lower average glucose levels throughout the day.
As a board-certified physician, I have seen how the frustration of “doing everything right” yet seeing high readings can discourage patients. The science of chronobiology—the study of internal clocks—indicates that our sensitivity to insulin and our body’s ability to process sugar fluctuate based on the hour. Understanding these peaks and valleys allows for a more surgical approach to fitness, transforming a general health habit into a targeted clinical tool.
The Post-Meal Window: Targeting Glucose Spikes
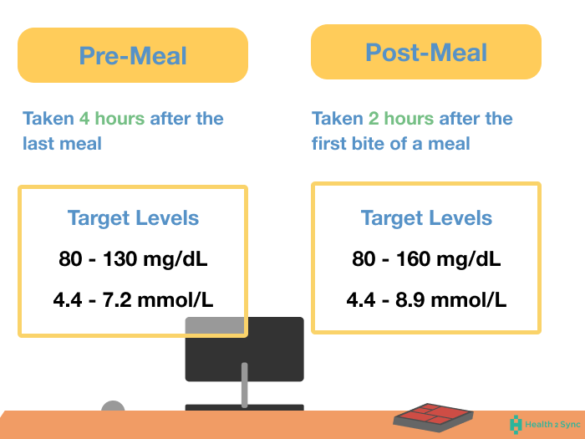
The most immediate impact on blood sugar occurs when exercise is performed shortly after a meal. For many, the glucose peak occurs roughly 30 to 90 minutes after eating. Engaging in moderate activity—such as a brisk walk or light strength training—during this window encourages the skeletal muscles to utilize the newly absorbed glucose for energy.
This timing is particularly effective for those with insulin resistance. Because exercise increases the expression of GLUT4 transporters—proteins that move glucose into cells—it provides a non-pharmacological way to reduce the burden on the pancreas. The goal is not necessarily high-intensity training, but consistent movement that keeps the metabolic engine running during the body’s most volatile glucose periods.
However, the “best” time is also influenced by the type of meal consumed. High-carbohydrate meals typically produce sharper spikes, making the post-meal walk even more critical. For those managing Type 2 diabetes, this strategy can help reduce HbA1c levels, a three-month average of blood sugar, by minimizing the volatility of daily readings.
Chronotypes and the Internal Clock
While post-meal activity addresses immediate spikes, the broader concept of “chronotypes”—whether you are an early bird or a night owl—plays a significant role in overall exercise efficacy. Our circadian rhythms regulate everything from core body temperature to hormone secretion, including cortisol and insulin.
Research indicates that matching workouts to your specific body clock can enhance performance and potentially lower the risk of cardiovascular complications. For “larks” (early risers), morning workouts often align better with their natural peak in alertness and metabolic readiness. Conversely, “owls” may find that late afternoon or evening sessions result in better strength gains and more stable energy levels.
When exercise is forced at a time that clashes with a person’s chronotype, the body may respond with higher levels of stress hormones. Since cortisol can trigger the liver to release more glucose into the bloodstream, exercising at the “wrong” time for your specific biology could, in some cases, lead to temporary blood sugar elevations—a phenomenon sometimes seen in early morning workouts for those with certain types of diabetes.
Comparing Exercise Timing Strategies
| Timing Strategy | Primary Goal | Key Biological Mechanism |
|---|---|---|
| Post-Meal (30-90 min) | Blunt Glucose Spikes | Increased GLUT4 glucose uptake |
| Morning (Chronotype-aligned) | Metabolic Reset | Alignment with cortisol peaks |
| Evening (Chronotype-aligned) | Performance/Recovery | Optimized core temperature |
The Cardiovascular Connection and Long-Term Risks
The benefits of timing extend beyond glucose management. Aligning physical activity with the body’s internal clock may also reduce the risk of heart disease. The heart, like the pancreas, follows a circadian rhythm. blood pressure and heart rate naturally fluctuate throughout a 24-hour cycle.
Studies suggest that exercising when the body is most primed for it—often in the late afternoon for a large portion of the population—can lead to better improvements in blood pressure and vascular function. For those with metabolic syndrome, which often combines high blood sugar with hypertension, this dual benefit is critical for long-term survival and quality of life.
The challenge for many is the “friction” of scheduling. The BBC has highlighted that a lack of motivation often stems from trying to exercise at a time that contradicts one’s natural biological preference. When the timing is wrong, the effort feels greater and the perceived benefit is lower, which often leads to abandonment of the routine.
Practical Implementation and Safety
For those looking to optimize their schedule, the transition should be gradual. It is significant to monitor how the body responds to different timings, especially for those using insulin or glucose-lowering medications, as the risk of hypoglycemia (dangerously low blood sugar) can increase when exercise is combined with medication.

- The “10-Minute Rule”: Start with a 10-minute walk after the largest meal of the day to observe the impact on post-meal readings.
- Track Your Energy: Note the times of day when you sense most energetic versus most sluggish to identify your chronotype.
- Consistency Over Intensity: Regular, moderately timed movement is generally more effective for glucose stability than sporadic, high-intensity workouts.
Patients should consult with their healthcare provider to determine if their medication dosage needs adjustment when shifting their exercise window, particularly if they are moving toward more intense activities in the early morning or late evening.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Looking ahead, the medical community is moving toward “precision medicine,” where exercise prescriptions will likely be tailored to an individual’s genetic chronotype and real-time glucose monitoring data. Further research into the interplay between the American Diabetes Association guidelines and circadian biology is expected to refine these recommendations in the coming years.
We aim for to hear from you. Have you noticed a difference in your energy or blood sugar levels by changing when you work out? Share your experience in the comments below.