It often begins as a subtle tightening in the chest or a sudden, unexplained surge of heat. Within seconds, the world can feel as though it is closing in, accompanied by a racing heart, shallow breath, and an overwhelming sense of impending doom. For those experiencing a panic attack, the sensation is not merely psychological; it is a violent, full-body physiological takeover that can leave a person feeling powerless and terrified.
Understanding the mechanics of this response is the first step toward regaining control. While a panic attack feels like a medical emergency, it is essentially a “false alarm” of the body’s survival mechanism. When the brain perceives a threat—even if that threat is an internal thought or a subconscious trigger—it activates the sympathetic nervous system, flooding the body with adrenaline and cortisol to prepare for a “fight or flight” scenario.
Clinical psychologist Dr. Julie Smith has become a leading voice in translating these complex biological processes into actionable tools for the general public. By focusing on the intersection of psychology and physiology, Dr. Smith outlines a framework for not only surviving a panic attack but actively interrupting the feedback loop that sustains it. For those navigating the disorientation of acute anxiety, the goal is not to “fight” the panic, but to signal to the brain that the danger is not real.
As a physician, I have seen how the physical symptoms of panic—tachycardia, dizziness, and hyperventilation—often lead patients to believe they are having a heart attack or a stroke. This fear creates a secondary layer of panic, which in turn releases more adrenaline, intensifying the symptoms. This is known as the “panic loop,” and breaking it requires a deliberate shift from the emotional centers of the brain back to the rational, sensory-driven prefrontal cortex.
The Biology of the Panic Loop
To stop a panic attack, one must first understand why it persists. A panic attack is an overreaction of the amygdala, the brain’s almond-shaped alarm system. When the amygdala triggers the fight-or-flight response, your heart rate increases to pump blood to your muscles, and your breathing becomes shallow to take in more oxygen. However, when there is no physical predator to fight or forest to flee, these sensations are interpreted by the conscious mind as signs of disaster.
This interpretation is where the “loop” begins. A person notices their heart racing and thinks, “Something is wrong with my heart.” This thought is perceived by the amygdala as a new threat, which triggers more adrenaline, making the heart beat even faster. The result is a spiraling escalation of physical distress and mental terror.
Breaking this cycle requires an “interruption”—a physical or mental stimulus strong enough to override the amygdala’s alarm and force the body back into the parasympathetic nervous system, often referred to as the “rest and digest” state.
Immediate Tools for Physiological De-escalation
When the body is in a state of high arousal, talking oneself “out of it” is rarely effective because the rational part of the brain is effectively offline. Instead, the most effective interventions are those that target the body’s hardware directly.
The Mammalian Dive Reflex
One of the most potent ways to abruptly lower the heart rate is by triggering the mammalian dive reflex. This is a biological response found in all mammals that optimizes oxygen conservation when submerged in cold water. By splashing ice-cold water on the face or holding a cold pack to the eyes and cheekbones for 30 seconds, you send a signal to the vagus nerve. This nerve tells the heart to slow down and the brain to shift out of the “panic” mode, providing an almost immediate physiological “reset.”
Controlled Exhalation
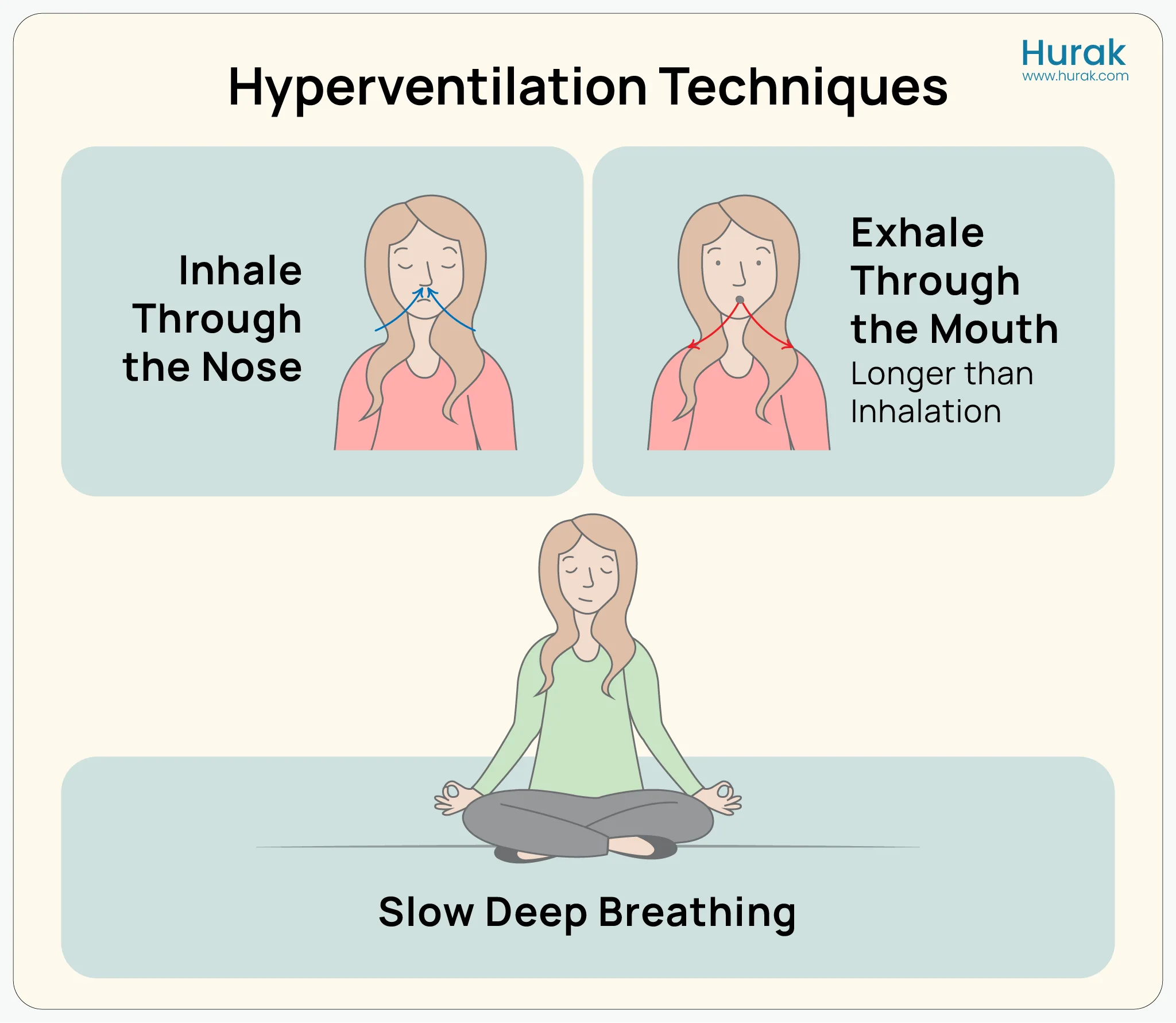
Hyperventilation—taking in too much oxygen and blowing off too much carbon dioxide—is a hallmark of panic. This imbalance causes the dizziness and tingling in the fingers that often terrify people. To counter this, the focus must be on the exhale. By making the exhale longer than the inhale (for example, breathing in for four seconds and breathing out for six), you stimulate the parasympathetic nervous system, signaling to the brain that the “emergency” has passed.
Sensory Grounding
Grounding techniques pull the mind away from internal catastrophic thoughts and back into the physical environment. The “5-4-3-2-1” method is a gold standard in clinical practice:
- 5: Acknowledge five things you see around you.
- 4: Acknowledge four things you can touch.
- 3: Acknowledge three things you hear.
- 2: Acknowledge two things you can smell.
- 1: Acknowledge one thing you can taste.
This process forces the brain to switch from the amygdala’s emotional processing to the prefrontal cortex’s sensory processing, effectively “grounding” the person in the present moment.
The Paradox of Acceptance
Perhaps the most challenging but effective strategy is the practice of non-resistance. Many people attempt to “fight” a panic attack, which involves tensing the muscles and mentally pleading for the feeling to stop. In the eyes of the brain, “fighting” is a confirmation that there is a threat, which only fuels the production of adrenaline.

The paradox of panic is that the more you accept the sensations, the faster they dissipate. By observing the symptoms with a sense of curiosity—“My heart is beating swift right now, and that is an uncomfortable but harmless sensation”—you stop feeding the panic loop. This shift from “victim” to “observer” reduces the fear, which eventually allows the adrenaline to metabolize and the body to return to baseline.
| Tool | Primary Action | Physiological Effect |
|---|---|---|
| Cold Water/Ice | Vagus nerve stimulation | Immediate heart rate reduction |
| Extended Exhale | CO2 balance restoration | Activates parasympathetic system |
| 5-4-3-2-1 Method | Sensory redirection | Shifts activity to prefrontal cortex |
| Radical Acceptance | Cognitive reframing | Stops the adrenaline feedback loop |
Disclaimer: This content is for informational purposes only and does not constitute medical advice. Panic attack symptoms can mimic other serious medical conditions, such as cardiac events. Always consult a healthcare provider for a formal diagnosis and personalized treatment plan.
While these immediate tools provide essential relief, long-term management often involves Cognitive Behavioral Therapy (CBT) or medication to address the underlying triggers of anxiety. The transition from acute crisis management to long-term stability is a journey that typically involves working with a licensed mental health professional to rewire the brain’s response to stress.
Looking forward, the field of mental health is moving toward more integrated, “bottom-up” approaches—treating the body’s physical state as a gateway to treating the mind. As more people adopt these evidence-based physiological tools, the stigma surrounding panic disorders continues to diminish, replaced by a practical understanding of human biology.
Do you have a grounding technique that works for you? Share your experience in the comments below or share this guide with someone who may need it.

