Walk into any office building in Berlin or a classroom in Munich this month, and the soundtrack is familiar: a rhythmic cadence of coughing, the rustle of tissues, and the hushed conversations of colleagues discussing who is “out sick” this week. For many Germans, the current wave of respiratory infections feels like a return to a more chaotic era of public health, where the lines between a common cold, the seasonal flu, and COVID-19 have blurred into a single, exhausting experience of malaise.
As a physician, I have seen this pattern evolve over the last few seasons. We are no longer dealing with a single dominant pathogen, but rather a “syndemic”—a situation where multiple viruses circulate simultaneously, compounding the strain on both the individual patient and the healthcare infrastructure. The current data suggests that Germany is navigating a complex intersection of Influenza, SARS-CoV-2, and Respiratory Syncytial Virus (RSV), creating a diagnostic challenge for primary care providers and a source of anxiety for the public.
The Robert Koch Institute (RKI), Germany’s federal agency for disease control, continues to monitor these trends through its sentinel surveillance system. While the acute crisis phase of the pandemic has passed, the “winter wave” has regained its seasonal predictability, albeit with a more complicated viral cocktail. The result is a significant increase in absenteeism across the workforce and a recurring bottleneck in general practitioner (GP) waiting rooms, where the primary question remains: “Which one do I have?”
The Diagnostic Dilemma: Flu, Cold, or Corona?
From a clinical perspective, the difficulty in distinguishing between these illnesses is not just a nuisance—We see a public health hurdle. The symptomatic overlap is profound. Fever, fatigue, a sore throat, and a dry cough are the hallmarks of all three major respiratory threats. However, the underlying pathology and the required interventions differ significantly.
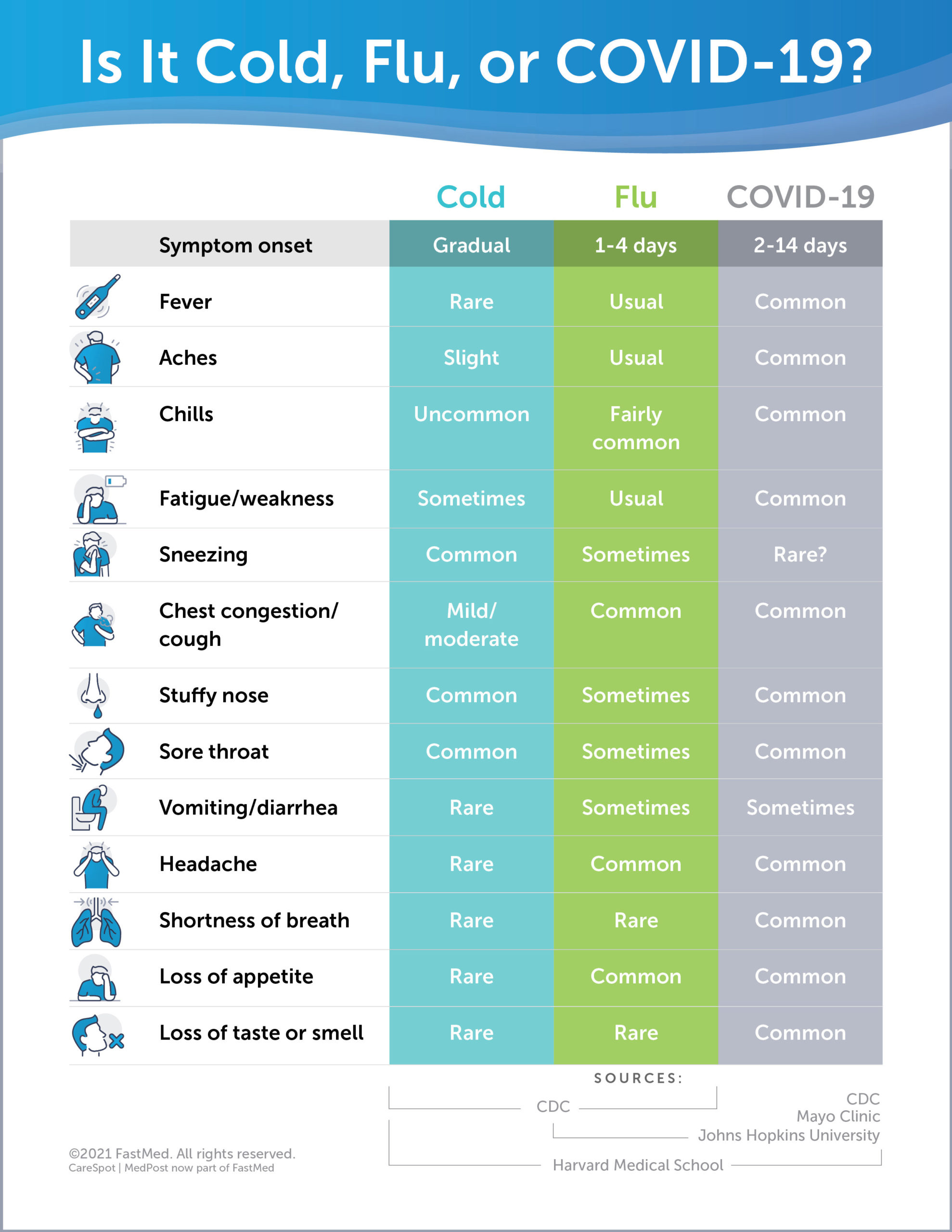
The “common cold” (grippaler Infekt) is typically caused by rhinoviruses or coronaviruses other than SARS-CoV-2. These are generally mild and self-limiting. Influenza, however, is a systemic assault. It often hits with a sudden onset of high fever and severe muscle aches (myalgia), which are less common in a standard cold. COVID-19 remains the wildcard; while vaccination and prior infection have attenuated the severity for many, it still presents with a wider range of symptoms, including the lingering “brain fog” or extreme fatigue that neither the flu nor a cold typically produces.
The danger of the “it’s just a cold” mentality is that it can lead to delayed treatment for high-risk groups. For the elderly or immunocompromised, a “simple” RSV infection can lead to severe bronchiolitis or pneumonia, requiring hospitalization. This is why the current push from health authorities emphasizes testing over guessing.
| Feature | Common Cold | Influenza (Flu) | COVID-19 |
|---|---|---|---|
| Onset | Gradual | Sudden/Abrupt | Variable |
| Fever | Rare/Low | High (Common) | Common |
| Muscle Aches | Slight | Severe | Common |
| Incubation | 1–3 Days | 1–4 Days | 2–14 Days |
| Primary Risk | Mild discomfort | Pneumonia | Long COVID/Severe ARDS |
The Strain on the ‘Hausarzt’ System
The current wave is testing the resilience of Germany’s primary care network. The Hausarzt (general practitioner) is the first point of contact for millions, and during these peaks, the system often reaches a breaking point. The surge in patient volume is not merely a result of the number of sick people, but the time required to differentiate these viruses.
Physicians are now spending a disproportionate amount of time conducting rapid antigen tests to determine if a patient needs isolation (for COVID-19) or if they can return to work after a few days of rest. This “diagnostic triage” slows down the flow of the clinic, leading to the infamous overcrowded waiting rooms that paradoxically increase the risk of cross-infection among patients.
there is a documented “immunity gap.” During the strict lockdown periods of 2020 and 2021, the population’s exposure to common rhinoviruses and the flu plummeted. Now, we are seeing a “catch-up” effect where the population is more susceptible to viruses that would have been routine in 2019, leading to more frequent and sometimes more severe infections in children and young adults.
Navigating the Recovery: When to Seek Help
For the majority of healthy adults, the strategy remains supportive care: hydration, rest, and the judicious use of antipyretics like ibuprofen or paracetamol. However, the threshold for seeking medical intervention should be clear. I advise patients to monitor for “red flag” symptoms that indicate a progression from a viral upper respiratory infection to a lower respiratory complication.
- Shortness of Breath: Any difficulty breathing or a feeling of chest tightness requires immediate medical evaluation.
- Persistent High Fever: A fever that does not respond to medication or returns after a period of improvement (a “double-peak”) can signal a secondary bacterial pneumonia.
- Oxygen Saturation: For those with home pulse oximeters, a drop below 94% is a signal to contact a provider.
- Dehydration: Particularly in the elderly, an inability to keep fluids down can lead to rapid kidney dysfunction.
Vaccination remains the most effective tool for reducing the severity of these illnesses. The Standing Committee on Vaccination (STIKO) in Germany recommends annual flu shots and updated COVID-19 boosters for those over 60, people with underlying health conditions, and medical staff. While these vaccines may not always prevent a mild infection, they are highly effective at preventing the hospitalizations that crash the healthcare system.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As Germany moves toward the end of the winter season, the RKI is expected to release its comprehensive seasonal summary in the coming weeks, which will provide a definitive look at the total burden of disease and the efficacy of this year’s vaccine formulations. This data will be critical in shaping the public health strategy for the next cycle.
Do you have thoughts on how your workplace or community is handling the current wave of illness? Share your experience in the comments below.