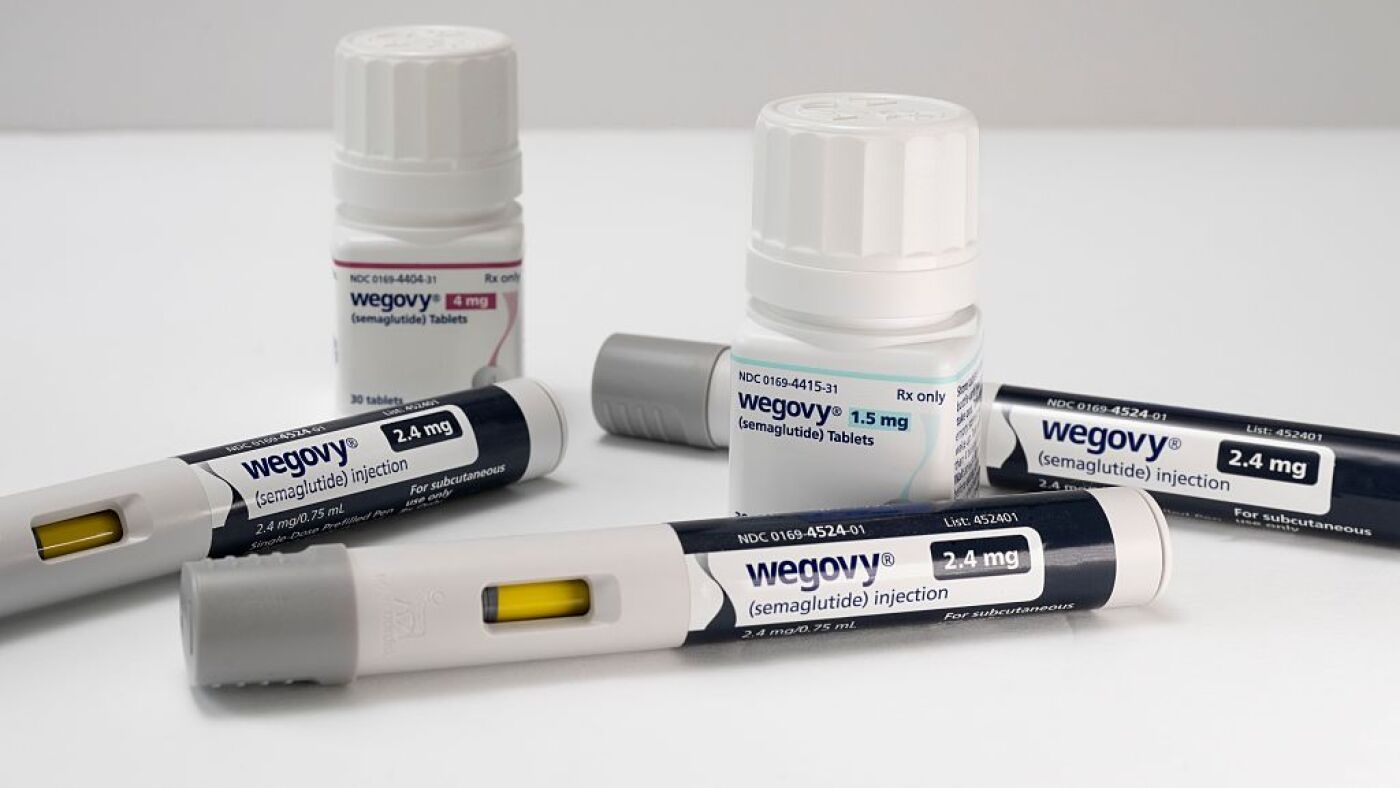
For millions of Medicare beneficiaries, the promise of GLP-1 weight loss medications has long been tempered by a staggering price tag. While drugs like Wegovy and Zepbound have demonstrated significant efficacy in reducing weight and improving metabolic health, they have remained largely out of reach for seniors due to a long-standing Medicare restriction against covering weight loss treatments.
That is about to change, albeit temporarily. The Centers for Medicare & Medicaid Services (CMS) has announced a new initiative known as the Medicare GLP-1 Bridge, a pilot program that will allow eligible beneficiaries to access select weight management medications for a flat $50 monthly copayment. The program is designed to provide a critical lifeline to patients who meet clinical guidelines but cannot afford the current cash prices, which can range from $149 to nearly $700 per month.
As a physician, I view this as a significant shift in how the federal government approaches obesity—treating it not merely as a lifestyle issue, but as a chronic medical condition requiring pharmacological intervention. However, the “Bridge” program is not a permanent benefit. It is a short-term experiment running from July 1, 2026, through December 31, 2027, intended to gather data before the government decides on a long-term coverage strategy for 2028.
Who Qualifies for the $50 Copay?
Access to the Bridge program is not universal; it is strictly tied to clinical necessity and existing insurance status. To participate, a patient must first be enrolled in a Medicare Part D prescription drug plan. Once that baseline is met, eligibility is determined by Body Mass Index (BMI) and the presence of weight-related comorbidities.
Under the program guidelines, beneficiaries will qualify if they fall into one of two categories:
- Automatic Qualification: Individuals with a BMI of 35 or higher.
- Conditional Qualification: Individuals with a BMI of 27 or higher who also have a qualifying health condition, such as heart disease or prediabetes.
This focus on BMI and comorbidities aligns with standard clinical practice, ensuring that the most high-risk patients—those for whom weight loss would most drastically reduce the risk of stroke or heart failure—get priority access. According to the CDC, approximately 40% of American adults are clinically obese (BMI of 30 or higher), suggesting a massive potential patient pool for this pilot.
Navigating the Logistics: A Different Kind of Benefit
The Medicare GLP-1 Bridge does not operate like a standard Part D benefit. Patients will not simply take their prescription to their pharmacist and apply their usual insurance. Instead, the program utilizes a centralized prior authorization system managed by Humana, a CMS contractor.
The workflow is streamlined to lower the barrier for providers: doctors do not need to be formally enrolled as Medicare providers to submit a prior authorization request or write a prescription under this specific program. Once the request is approved through the central system, the patient pays the flat $50 copay at the pharmacy. Crucially, this $50 fee remains constant regardless of the dosage, providing a level of financial predictability that is rare with these medications, which typically increase in price as the dose is titrated upward.
| Medication | Covered Formulations | Copay Cost |
|---|---|---|
| Wegovy | Pill and Injectable | $50 / month |
| Zepbound | KwikPen formulation | $50 / month |
| Foundayo | Pill formulation | $50 / month |
The Fine Print: Financial Gaps and Clinical Risks
While a $50 copay is a drastic reduction from the market price, the program contains several “catches” that may leave the most vulnerable patients struggling. First, the $50 payment is a standalone cost. It does not count toward the patient’s annual Part D deductible, nor does it contribute to the $2,100 annual out-of-pocket cap on prescription drugs.
More concerning is the exclusion of low-income subsidies. Beneficiaries who rely on the Medicare Extra Help program cannot apply that assistance toward the Bridge program’s copay. For a senior living on a fixed Social Security check of $750 a month, a $50 monthly expense is still a significant financial burden, especially when compared to the $5 or $10 copays they may pay for other essential medications.
There is also the clinical “cliff” at the end of 2027. GLP-1 medications are generally intended for long-term use. Clinical data consistently shows that patients who discontinue these drugs often regain a substantial portion of the weight they lost. Because the Bridge program ends on December 31, 2027, patients face the very real possibility of losing access to their medication unless a permanent program is established by 2028.
The Policy Struggle: Why a ‘Bridge’ Instead of a Permanent Plan?
The existence of a “Bridge” program is a symptom of a larger conflict between the federal government and private insurers. The Trump administration originally envisioned a two-step process: a short pilot followed by a long-term program where the cost would shift from the government to insurance companies.
However, that transition hit a wall. Recent projections indicated that shifting these costs to insurers would cost the industry billions of dollars in the first year alone. When not enough insurers volunteered for the plan by the April deadline, CMS extended the Bridge program to 18 months. This extension serves two purposes: it gives insurers more time to negotiate and provides the government with real-world data on exactly how many millions of seniors will utilize these drugs.
Despite the benefit to patients, the cost to the taxpayer will be immense. While CMS has not released public projections, analysis from KFF suggests that with roughly 14 million Medicare beneficiaries overweight or obese, the subsidies required to keep the copay at $50 could run into the billions of dollars annually.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult with your healthcare provider to determine if GLP-1 medications are appropriate for your specific health needs.
The next critical checkpoint for this program will be the official rollout on July 1, 2026. Between now and then, the healthcare industry will be watching closely to see if the data gathered during the Bridge phase can convince insurers to accept a long-term coverage model for obesity treatment.
Do you think a $50 copay is accessible for most seniors, or does it still leave too many behind? Share your thoughts in the comments or share this story with someone who may be eligible.