The moment a patient hears the words “breast cancer,” the world often seems to stop. Even when the diagnosis is qualified with medical terminology like “ductal carcinoma in situ” (DCIS), the word “carcinoma” triggers an immediate, visceral fear. This specific anxiety has become a focal point of digital health conversations, exemplified by a viral TikTok from Dr. Mario Gianella, where a patient asks the quintessential question: “Doctor, I was diagnosed with DCIS; how serious is it?”
For many, DCIS is a confusing diagnosis because it sits in a medical gray area. This proves technically classified as Stage 0 breast cancer, yet it is frequently described by clinicians as “non-invasive” or even “pre-cancer.” As a physician and medical writer, I have seen how this linguistic gap creates profound distress for patients who are told their condition is “not invasive” while simultaneously being told they have cancer.
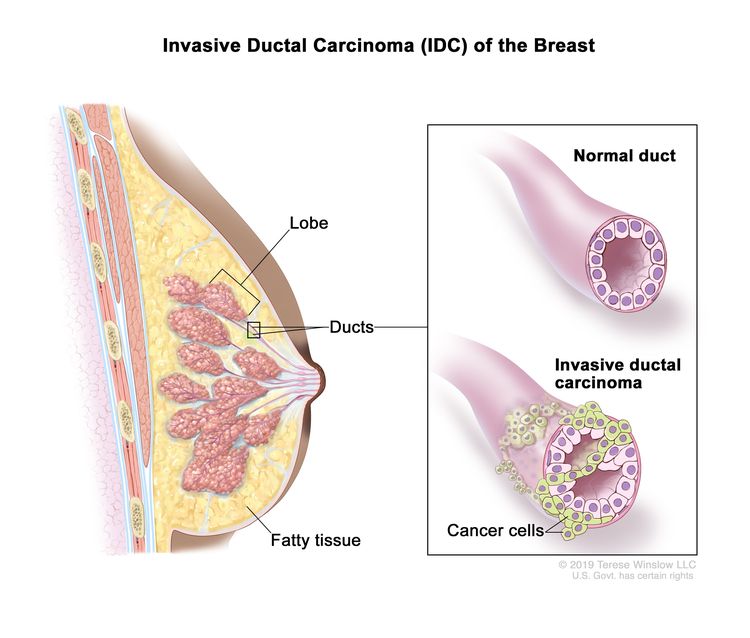
Understanding DCIS requires a shift in how we view the progression of the disease. Unlike invasive ductal carcinoma, which has the ability to spread to lymph nodes and other organs, DCIS is confined to the milk ducts of the breast. While it does not have the capacity to metastasize in its current state, it serves as a critical warning sign. If left untreated, DCIS can evolve into invasive cancer, making early detection and a nuanced treatment plan essential for long-term health.
Defining the ‘In Situ’ Distinction
To understand why DCIS is treated differently than invasive cancer, one must look at the anatomy of the breast. The “ducts” are the tubes that carry milk from the glands to the nipple. “In situ” is a Latin phrase meaning “in its original place.” In the case of DCIS, abnormal cells are growing inside the lining of these ducts but have not broken through the basement membrane—the structural barrier that separates the duct from the surrounding breast tissue.
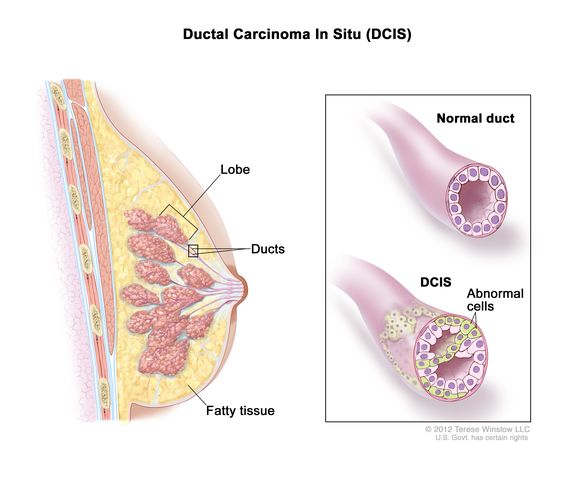
Because these cells are contained, the risk of the cancer spreading to other parts of the body is virtually zero while it remains in the DCIS stage. Here’s why the prognosis for DCIS is exceptionally high; the five-year survival rate is nearly 100%. However, the “seriousness” of the diagnosis stems from the fact that it is often impossible to tell which areas of DCIS will remain dormant and which will eventually breach that membrane to become invasive.
How DCIS is Typically Detected
DCIS is frequently an incidental finding. Many patients have no palpable lump and no visible changes to the breast. Instead, it is often discovered during routine screening mammograms as “microcalcifications”—tiny calcium deposits that appear as bright white spots on an X-ray. While calcifications are common and often benign, certain patterns alert radiologists to the possibility of DCIS, leading to a diagnostic biopsy.

Navigating Treatment Pathways
Because DCIS is non-invasive, the goal of treatment is to prevent it from ever becoming invasive. However, the approach to treatment has evolved. In the past, the standard was aggressive surgical removal. Today, the medical community emphasizes a more personalized approach based on the patient’s age, the size of the lesion, and the grade of the cells.
The primary options generally fall into two categories: breast-conserving surgery (lumpectomy) or a mastectomy. For many, a lumpectomy combined with radiation therapy provides the same survival benefit as a mastectomy, though the choice often depends on the extent of the DCIS within the breast.
| Approach | Procedure Goal | Typical Follow-up | Key Consideration |
|---|---|---|---|
| Lumpectomy | Remove the DCIS and a small margin of healthy tissue. | Often followed by radiation therapy. | Preserves breast appearance; risk of local recurrence. |
| Mastectomy | Remove the entire breast tissue to eliminate DCIS. | Radiation usually not required. | Higher surgical impact; eliminates most local risk. |
| Hormone Therapy | Block estrogen receptors in breast cells. | Daily medication (e.g., Tamoxifen). | Used if the DCIS is estrogen-receptor positive (ER+). |
The Debate Over Overdiagnosis
One of the most complex aspects of DCIS—and a topic rarely covered in short-form social media videos—is the phenomenon of overdiagnosis. Because we have become so proficient at detecting Stage 0 cancer through high-resolution imaging, we are finding many cases of DCIS that might never have progressed to cause harm during a patient’s lifetime.
This has led to a significant debate within the oncology community. Some experts argue that treating every case of DCIS leads to “over-treatment,” exposing women to the side effects of surgery and radiation for a condition that may have remained indolent. This is why “active surveillance”—closely monitoring the area with frequent imaging rather than immediate surgery—is being studied as a viable option for remarkably low-grade DCIS.
Questions to Ask Your Oncology Team
If you or a loved one has received a DCIS diagnosis, the “seriousness” is best determined through a detailed conversation with a multidisciplinary team. Consider asking the following:
- What is the grade of the DCIS? (Low-grade cells grow more slowly than high-grade cells).
- Is the DCIS focal or multifocal? (Is it in one spot or spread across multiple areas of the breast?).
- Is the lesion ER+ or ER-? (This determines if hormone therapy is an option).
- What is the risk of recurrence if I choose a lumpectomy over a mastectomy?
- Am I a candidate for active surveillance?
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The future of DCIS management is moving toward genomic profiling. Researchers are currently working to identify specific biomarkers that can distinguish between “aggressive” DCIS and “indolent” DCIS. The next major checkpoint in this evolution is the integration of these molecular tests into standard clinical practice, which would allow doctors to move away from a “one size fits all” surgical approach and toward truly precision medicine.
We want to hear from you. Have you or a family member navigated a Stage 0 diagnosis? Share your experience or ask a question in the comments below to help others in the community.
