The transmission began at a birthday party. A man sat beside an infected individual, contracted the virus, and later passed it to his wife. He died shortly after. His wife, in turn, infected 10 more people during his wake. Perhaps most alarming was another guest at that initial party who had no significant interaction with the index patient beyond a brief “hello” while crossing paths; that person also fell ill.
This sequence—one index patient leading to 33 subsequent infections and 11 deaths across four waves of transmission—is not a hypothetical exercise in epidemiology. It’s a meticulously documented outbreak of the Andes strain of hantavirus in Argentina, published in the New England Journal of Medicine (NEJM). The data suggested a chilling reality: the virus was moving through the air, independent of physical touch or prolonged proximity.
Despite this evidence, a recurring pattern has emerged in public health messaging. When hantavirus outbreaks occur, officials frequently lean on the phrase “prolonged close contact” to describe how the virus spreads. While this phrasing is intended to reassure the public and prevent panic, it creates a foundational myth that can jeopardize the safety of healthcare workers and the efficacy of contact tracing.
In any outbreak, the most critical question is: How does it spread? The answer dictates every subsequent safety measure, from the type of masks worn by doctors to the ventilation requirements for quarantined spaces. When officials insist on a “close contact” narrative despite evidence of airborne transmission, they risk repeating one of the most costly mistakes of the early 21st century.
The Aerosol Blind Spot
For decades, the medical community categorized respiratory transmission into two rigid buckets: “droplets” and “airborne.” Droplets were thought to be large, heavy particles that fell to the ground within six feet. Airborne transmission was reserved for a tiny handful of pathogens, like measles or tuberculosis, which could linger in the air for hours.
This binary thinking led to a systemic failure at the start of the COVID-19 pandemic. Because health officials believed SARS-CoV-2 spread primarily via large droplets and contaminated surfaces—known as fomite transmission—the global response focused on scrubbing elevator buttons and marking floors with social-distancing stickers. These interventions did little to stop a virus that traveled via small aerosols—microscopic particles that linger in poorly ventilated enclosed spaces.

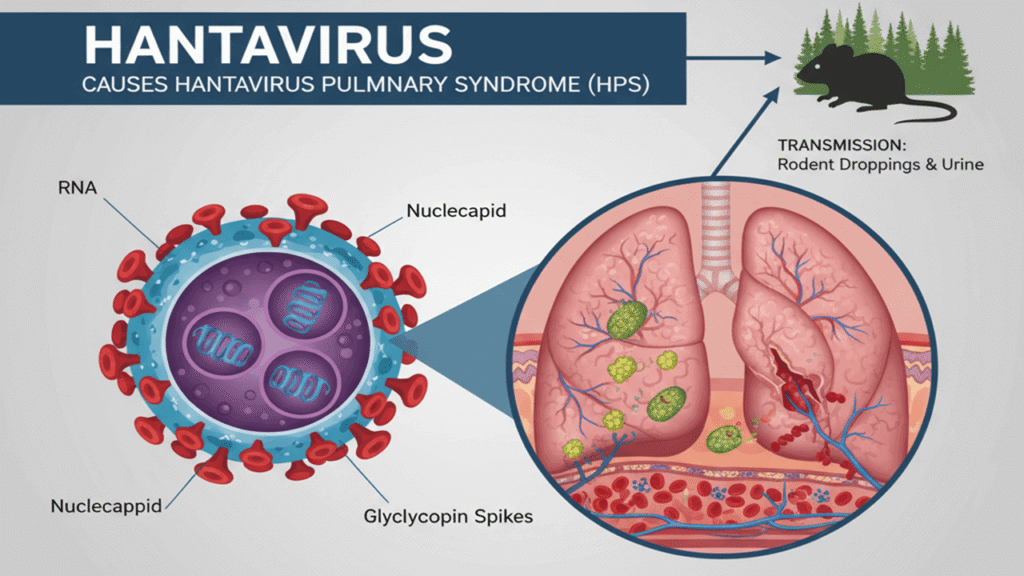
The Andes strain of hantavirus presents a similar challenge. Most hantaviruses are zoonotic; they originate in rodent feces and urine. A person typically becomes ill by inhaling dust contaminated with these droppings. However, the Andes strain is unique because it is the only one known to transmit from human to human.
The Argentina data published in the NEJM indicates that this human-to-human spread does not always require the “prolonged close contact” often cited by authorities. The fact that a person could be infected simply by crossing paths with a patient suggests that the virus can remain suspended in the air, bypassing the need for direct physical proximity.
Comparing Transmission Narratives
| Feature | “Close Contact” Narrative | “Airborne/Aerosol” Evidence |
|---|---|---|
| Primary Vector | Direct touch or large droplets | Small particles suspended in air |
| Distance Risk | Generally within 6 feet | Can travel across a room |
| Duration | Requires extended time together | Can occur during brief encounters |
| Key Protection | Hand washing, surgical masks | N95 respirators, HEPA filtration |
The Danger of False Certainty
The insistence on “close contact” as a requirement for transmission is more than a semantic disagreement; it is a matter of clinical safety. When medical teams treat patients based on the “close contact” myth, they may rely on gowns and goggles while neglecting the respiratory protection necessary for an airborne pathogen.
If a virus is airborne, a standard surgical mask—which is designed to stop droplets from leaving the wearer’s mouth—is insufficient. Protection requires an N95 or higher-rated respirator, which filters out the microscopic aerosols the wearer inhales. The environment becomes a variable: without high-grade ventilation and air filtration, a hospital room or a cruise ship cabin can become a reservoir for the virus.
This gap in communication also hampers contact tracing. If tracers only notify people who had “prolonged” contact with a patient, they will miss the individuals who simply shared a dining room or a lecture hall for a short period. This allows the virus to move silently through a population, creating new clusters that appear to have no origin.
A Call for Public Health Humility
It is unlikely that the Andes hantavirus will spark a global pandemic. It is significantly less contagious than influenza or SARS-CoV-2. However, the lack of extensive experience with this specific strain means that any claim of absolute certainty is a risk. The current system of quarantine and treatment is generally functioning, and the risk to the general public remains low, but the messaging remains flawed.
The lesson from recent years is that public health officials must be candid about what they do not know. Making bold pronouncements to prevent panic often backfires when the evidence eventually shifts, leading to a collapse in public trust. Humility in the face of an emerging pathogen is not a sign of weakness; it is a requirement for scientific accuracy.
When officials insist on the wrong answer to the question of transmission, they provide a false sense of security that can lead people to take risks they will later regret. The goal should not be to provide a comforting answer, but the correct one.
Health authorities continue to monitor the genomic sequencing of the Andes strain to determine if the virus is mutating to become more transmissible. The next critical checkpoint will be the publication of updated epidemiological reports from South American health ministries, which will clarify the total number of human-to-human cases in the most recent clusters.
Do you believe public health communication has improved since the pandemic, or are we repeating the same mistakes? Share your thoughts in the comments below.

