For decades, the global benchmark for success in public health was simple: extend the human lifespan. In South Korea, this goal has been achieved with remarkable efficiency, placing the nation among the world leaders in longevity. However, a growing disparity between how long people live and how long they stay healthy is revealing a sobering reality about the nature of modern aging.
Recent data indicates that while overall life expectancy continues to climb, the healthy life expectancy in South Korea—the period of life spent free from chronic disease or disability—is not keeping pace. This widening gap suggests that many citizens are spending a significant portion of their final years battling debilitating illnesses or relying on intensive long-term care, transforming the triumph of longevity into a challenge of quality of life.
As a physician, I have seen this trend manifest in clinics daily. We have grow exceptionally good at preventing premature death through advanced acute care and pharmaceutical interventions, but we are struggling to prevent the slow accumulation of chronic morbidity. The result is a “longevity paradox”: we are adding years to life, but not necessarily life to those years.
The Growing Gap Between Survival and Wellness
The distinction between life expectancy and healthy life expectancy is critical for understanding the true burden of aging. Life expectancy measures the average age at death, whereas healthy life expectancy focuses on the years lived without significant health limitations. When these two numbers diverge, the resulting interval represents the “period of morbidity”—the years a person lives with a diminished capacity for independence.
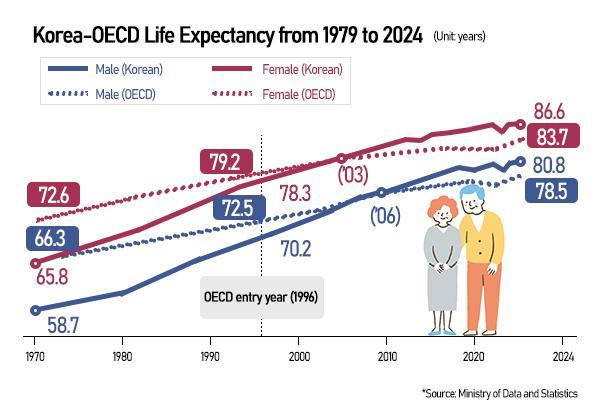
According to data from Statistics Korea, the national life expectancy has seen a steady increase, yet the growth of healthy years has stagnated or, in some demographics, slightly regressed. This means the average person may spend more than a decade of their senior years managing chronic conditions such as hypertension, diabetes, or neurodegenerative diseases.
This trend is particularly concerning given South Korea’s status as one of the fastest-aging societies globally. The rapid increase in the elderly population, coupled with a decline in healthy years, creates a compounding pressure on the national healthcare infrastructure and the social fabric of the family unit.
| Metric | Trend Direction | Primary Driver |
|---|---|---|
| Overall Life Expectancy | Increasing | Advanced medical technology, better nutrition |
| Healthy Life Expectancy | Stagnating/Decreasing | Rise in chronic metabolic diseases, sedentary lifestyles |
| Morbidity Period | Expanding | Prolonged survival with chronic illness |
The Drivers of Chronic Morbidity
The decline in healthy life expectancy is rarely the result of a single factor. Instead, We see a confluence of lifestyle shifts and the inherent nature of chronic disease management. The prevalence of “lifestyle diseases”—conditions driven by diet, physical inactivity, and stress—has risen sharply. While these conditions are often manageable with medication, they rarely disappear, and their cumulative effect often leads to frailty in later stages of life.
the mental health component of aging is often overlooked. Social isolation and depression among the elderly can accelerate physical decline, creating a feedback loop where poor mental health leads to poorer physical outcomes, further reducing the number of healthy years lived.
From a clinical perspective, the focus has historically been on “treatment” rather than “prevention.” The medical system is designed to respond to crises—a heart attack, a stroke, a fracture—rather than to optimize the biological resilience of a 60-year-old to ensure they remain mobile and cognitive at 80. This reactive approach maintains life but does not necessarily preserve vitality.
The Societal and Economic Toll
The implications of a shrinking healthy life expectancy extend far beyond the individual. The economic burden of long-term care is shifting from a familial responsibility to a state-level crisis. When the period of morbidity expands, the demand for nursing homes, home-care services, and long-term hospitalization increases exponentially.
This “care gap” places an immense emotional and financial strain on the “sandwich generation”—adults who are simultaneously caring for their children and their ailing parents. As the number of healthy years decreases, the duration of this caregiving burden increases, often forcing family members out of the workforce and further impacting national productivity.
Public health experts argue that the current model of healthcare is unsustainable. If the goal remains solely on extending life expectancy, the cost of maintaining a frail population will eventually overwhelm the national health insurance system. The shift must move toward “active aging,” where the priority is maintaining functional independence for as long as possible.
Bridging the Gap: A Path Toward Functional Longevity
To reverse the decline in healthy life expectancy, the approach to geriatric care must evolve from a pharmaceutical-first model to a holistic, preventive one. This involves several key shifts in public health strategy:
- Early Intervention: Shifting the window of preventive care from the 65+ demographic to the 40-60 age bracket to mitigate chronic risks before they become disabilities.
- Integrated Community Care: Moving away from institutionalized care toward community-based support systems that allow the elderly to age in place while receiving medical and social support.
- Nutritional and Physical Literacy: Implementing national programs that prioritize muscle mass retention (preventing sarcopenia) and cognitive stimulation to delay the onset of frailty.
- Mental Health Integration: Treating loneliness and social isolation as clinical risk factors that require systemic intervention.
The goal is not merely to avoid death, but to avoid the long, slow decline that often precedes it. By focusing on the “compression of morbidity”—pushing the onset of chronic illness as close to the end of life as possible—society can improve the quality of life for millions of seniors.
Disclaimer: This article is for informational purposes only and does not constitute professional medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next critical milestone in addressing this issue will be the upcoming updates to the national health promotion plans, which are expected to integrate more specific targets for healthy life expectancy rather than just overall longevity. These policy shifts will determine whether the future of aging in South Korea is defined by endurance or by wellness.
Do you believe our healthcare system focuses too much on longevity and not enough on quality of life? Share your thoughts in the comments below or share this article to start a conversation about healthy aging.

