The Future of Malaria Eradication: A Race Against Resistance
Table of Contents
- The Future of Malaria Eradication: A Race Against Resistance
- The Staggering Toll of Malaria: Why We Can’t Afford to Lose
- The Enemy Within: Understanding Resistance
- Hope on the Horizon: New Weapons in the Arsenal
- The American Angle: How the U.S. is Involved
- The Road Ahead: Collaboration and Innovation
- The Final Push: A Malaria-Free World
- FAQ: Your Questions Answered
- Pros and Cons: The Path to Eradication
- The Race Against Resistance: Can We Achieve a Malaria-Free World? A Q&A with Dr.Aris Thorne
Imagine a world without malaria. A world where children in sub-Saharan Africa can grow up without the constant threat of fever, chills, and potentially death. while this vision seems distant, groundbreaking advancements in science and collaborative efforts are bringing us closer to making it a reality. But the path is fraught with challenges, particularly the relentless evolution of drug and insecticide resistance.
The Staggering Toll of Malaria: Why We Can’t Afford to Lose
Malaria’s impact is devastating. sub-Saharan Africa bears the brunt, with eleven countries accounting for two-thirds of the global burden.While significant progress was made between 2000 and 2015, with new cases dropping by 18%, the fight has stalled, and in some regions, reversed. The World Health Association (WHO) estimates that 2.2 billion cases and 12.7 million deaths were averted between 2000 and 2023. Yet, in 2023 alone, Africa reported a staggering 246 million cases, far exceeding the WHO’s target of 47,000.
Quick Fact:
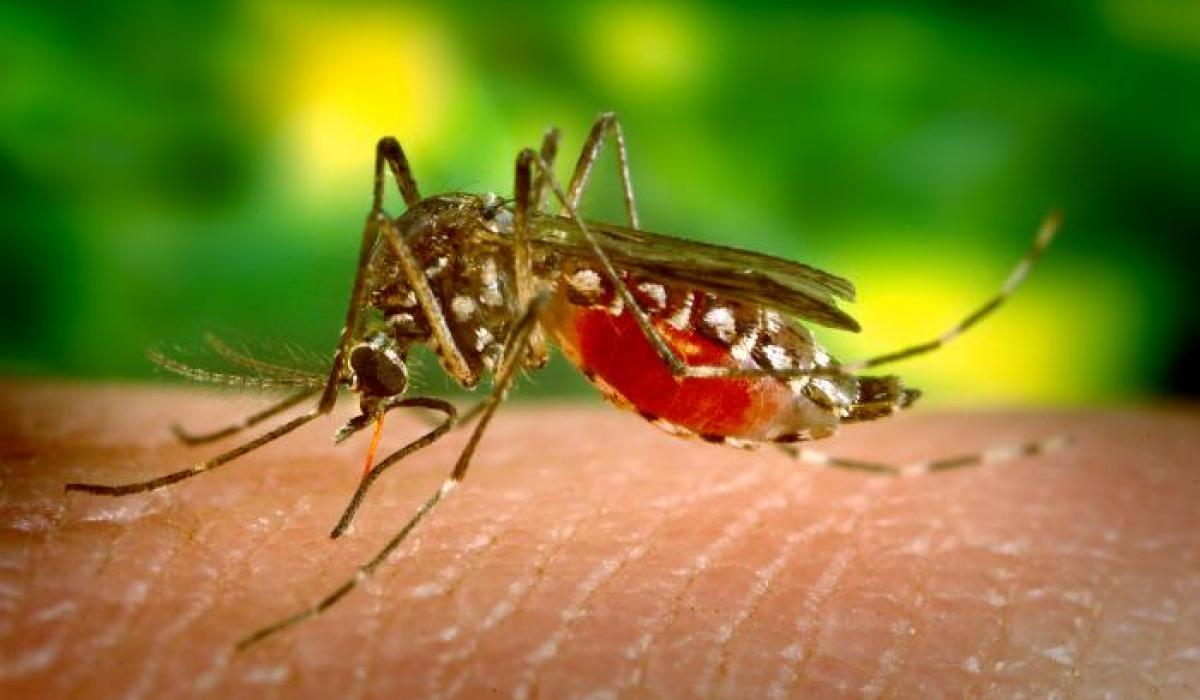
Did you know? Malaria is caused by parasites transmitted to humans through the bites of infected female Anopheles mosquitoes. It’s not contagious from person to person like a cold or the flu.
Why the stagnation? The answer lies in the adaptability of both the malaria parasites and the mosquitoes that carry them. thay are evolving faster than our current tools can keep up.
The Enemy Within: Understanding Resistance
The fight against malaria is a constant arms race. Mosquitoes are developing resistance to insecticides, and parasites are becoming resistant to antimalarial drugs. This resistance threatens to undo decades of progress.
Mosquitoes: Masters of Adaptation
african mosquitoes, particularly those that prefer human blood, are becoming increasingly adept at avoiding insecticide-treated surfaces. Studies in South Africa have shown that mosquitoes can enter homes and bite people without resting on sprayed walls. This behavioral adaptation, coupled with physiological resistance to insecticides like pyrethroids (the most common class used in mosquito nets), is a major concern.
Parasites: The Evolving Threat
the emergence of artemisinin resistance is particularly alarming. Artemisinin-based combination therapies (ACTs) are the cornerstone of malaria treatment. Resistance to artemisinin was first detected in Southeast Asia in 2007 and has as spread to parts of Africa, including Eritrea, Rwanda, Tanzania, and Uganda. Molecular markers of resistance have also been found in Namibia and Zambia.
Even more concerning, malaria parasites are developing mutations that allow them to evade detection by rapid diagnostic tests (RDTs), the primary tool for malaria diagnosis in Africa. This means that infected individuals may not be properly diagnosed and treated, leading to further transmission.
Hope on the Horizon: New Weapons in the Arsenal
Despite the challenges, there is reason for optimism. scientists are developing innovative tools and strategies to combat malaria, offering a renewed hope for eradication.
The Vaccine Revolution: A Game Changer
After decades of research, two malaria vaccines, RTS,S and R21, have been approved by the WHO and are being deployed in 19 African countries. These vaccines have shown promising results in reducing cases and deaths, particularly in children under five, the most vulnerable population. Clinical trials have demonstrated a reduction of serious malaria cases by around 30% and deaths by 17%.
The growth and deployment of these vaccines represent a monumental achievement. they offer a crucial layer of protection, especially in areas where insecticide and drug resistance are high.
next-Generation Mosquito Nets: Outsmarting Resistance
Researchers are developing new and improved insecticide-treated mosquito nets to overcome insecticide resistance.these nets incorporate new insecticides and chemical components that help manage resistance. Dual-insecticide nets, wich combine pyrethroids with other insecticides like pyriproxyfen or chlorfenapyr, are showing promise in killing mosquitoes that are resistant to pyrethroids alone.
Innovative Vector Control: Thinking Outside the Box
Beyond conventional methods, scientists are exploring novel approaches to control mosquito populations. These include:
Attractive Toxic Sugar baits (ATSBs):
Mosquitoes feed on sugar for energy. ATSBs exploit this behavior by using sweet, toxic baits to attract and kill mosquitoes. This method is environmentally friendly and can be deployed in areas where mosquitoes are resistant to insecticides.
Biological Control:
Researchers are investigating the use of modified gut bacteria to disrupt mosquito development or reduce their ability to transmit malaria parasites. this approach offers a enduring and targeted way to control mosquito populations.
Genetic Modification:
Releasing sterile or genetically modified mosquitoes into wild populations can reduce mosquito numbers. Trials are underway in Burkina Faso, where the release of genetically sterilized males has shown encouraging results in reducing mosquito populations.
New Antimalarial Drugs: A Fresh Approach
Two new antimalarial drugs are expected to become available in the next year or two. Artemisinin-based tritherapies, which combine artemisinin with two other antimalarial drugs, have shown high efficacy in clinical trials in Africa and Asia. Ganaplacide-Lumenfantrine, the first new antimalarial drug developed without artemisinin in over 20 years, has demonstrated effectiveness in young children and could be used against artemisinin-resistant parasites.
The American Angle: How the U.S. is Involved
The united States plays a critical role in the global fight against malaria. Through organizations like the U.S. Agency for International Development (USAID) and the Centers for Disease Control and Prevention (CDC), the U.S. provides significant funding, technical expertise, and research support to malaria-endemic countries.
The President’s Malaria Initiative (PMI):
Launched in 2005, the PMI is a U.S. government initiative that works to reduce malaria-related mortality by 50% across 24 high-burden countries in sub-saharan Africa and 3 programs in the Greater Mekong Subregion. The PMI provides insecticide-treated nets, antimalarial drugs, and diagnostic tools, as well as training and technical assistance to local health workers.
American research and Innovation:
American universities and research institutions are at the forefront of malaria research, developing new vaccines, drugs, and vector control strategies. For example, the National Institutes of Health (NIH) funds numerous research projects aimed at understanding the biology of malaria parasites and mosquitoes, as well as developing new tools to combat the disease.
Expert Tip:
Expert Tip: Support organizations like the Against Malaria Foundation (AMF) or Malaria No More. These organizations are highly effective at distributing insecticide-treated nets and advocating for increased funding for malaria control programs.
The Road Ahead: Collaboration and Innovation
Eradicating malaria will require a concerted effort from governments, researchers, healthcare workers, and communities. Collaboration is essential to ensure that limited resources are used effectively and that new tools are deployed rapidly.
Strengthening Health Systems:
Effective malaria control requires strong health systems that can deliver diagnostic testing, treatment, and prevention services to all populations, especially those in remote and underserved areas. Investing in training and equipping healthcare workers is crucial to ensure that they can accurately diagnose and treat malaria cases.
Community Engagement:
Engaging communities in malaria control efforts is essential to ensure that interventions are culturally appropriate and sustainable. Community health workers can play a vital role in educating people about malaria prevention, distributing mosquito nets, and providing early diagnosis and treatment.
Data-Driven Decision Making:
Collecting and analyzing data on malaria cases, mosquito populations, and drug and insecticide resistance is essential to inform decision-making and track progress. This data can be used to identify areas where interventions are most needed and to monitor the effectiveness of different control strategies.
The Final Push: A Malaria-Free World
The WHO has identified 25 countries with the potential to eliminate malaria by 2025. While none of these countries have yet achieved elimination, some have made significant progress. Costa Rica and Nepal have reported fewer than 100 cases, and Timor-Leste has reported only one case in recent years.
Three southern African countries – Botswana, eswatini, and South Africa – are also part of this group. Unfortunately, all of these countries recorded an increase in the number of cases in 2023. Though, with the new tools and strategies available, these countries and many others have the potential to eliminate malaria and bring us closer to the dream of a malaria-free world.
Reader Poll:
Reader Poll: How optimistic are you that we will see a malaria-free world in your lifetime?
FAQ: Your Questions Answered
Here are some frequently asked questions about malaria and the efforts to eradicate it:
What is malaria?
Malaria is a life-threatening disease caused by parasites that are transmitted to humans through the bites of infected female Anopheles mosquitoes.
What are the symptoms of malaria?
Symptoms of malaria include fever, chills, headache, muscle aches, and fatigue. In severe cases, malaria can lead to organ failure and death.
How is malaria diagnosed?
Malaria is typically diagnosed using rapid diagnostic tests (RDTs) or microscopy, which involves examining a blood sample under a microscope to look for malaria parasites.
How is malaria treated?
Malaria is treated with antimalarial drugs, such as artemisinin-based combination therapies (ACTs).
How can malaria be prevented?
Malaria can be prevented by using insecticide-treated mosquito nets, spraying indoor residual insecticides, and taking prophylactic antimalarial drugs.
What is artemisinin resistance?
Artemisinin resistance is a phenomenon in which malaria parasites become less susceptible to artemisinin, the key ingredient in ACTs. This resistance threatens the effectiveness of malaria treatment.
What are the new malaria vaccines?
The new malaria vaccines, RTS,S and R21, have been approved by the WHO and are being deployed in African countries.These vaccines have shown promising results in reducing malaria cases and deaths, particularly in children under five.
What is the role of the U.S. in the fight against malaria?
The U.S. plays a critical role in the global fight against malaria through organizations like USAID and the CDC, which provide funding, technical expertise, and research support to malaria-endemic countries.
Pros and Cons: The Path to Eradication
Eradicating malaria presents both significant opportunities and challenges.
Pros:
- Reduced mortality and morbidity,particularly in children under five.
- Improved economic productivity in malaria-endemic countries.
- Strengthened health systems and infrastructure.
- Increased global health security.
Cons:
- The emergence of drug and insecticide resistance.
- The high cost of developing and deploying new tools.
- The need for strong health systems and infrastructure.
- The challenges of reaching remote and underserved populations.
Despite the challenges, the potential benefits of eradicating malaria are enormous. By investing in research, strengthening health systems, and working together, we can make a malaria-free world a reality.
The Race Against Resistance: Can We Achieve a Malaria-Free World? A Q&A with Dr.Aris Thorne
Time.news: Dr. Thorne, thank you for joining us.Malaria continues to be a global health crisis. Our recent report, “The Future of Malaria Eradication: A Race Against Resistance,” highlights both the progress made and the daunting challenges ahead. Can you summarize the current state of the fight against malaria?
Dr.Aris thorne: thank you for having me. You’re right, it’s a complex picture. We’ve seen incredible progress as 2000, averting millions of cases and deaths.However, the momentum has stalled. Africa, in particular, continues to bear the brunt of the disease. In 2023 alone,the continent reported a staggering 246 million cases.This underscores that controlling malaria and working toward malaria eradication require persistent and innovative approaches.
Time.news: The article stresses the issue of resistance – mosquitoes to insecticides and parasites to antimalarial drugs. How significantly is this hampering efforts?
Dr. Aris Thorne: Resistance is arguably the biggest threat. It’s an arms race. Mosquitoes are becoming resistant to pyrethroids, the most common insecticide used in bed nets. They’re even changing their behavior to avoid treated surfaces.Simultaneously, we’re seeing the emergence and spread of artemisinin resistance in parasites. Artemisinin-based combination therapies (ACTs) are the cornerstone of malaria treatment,and their effectiveness is being undermined. This requires the continuous development and deployment of new antimalarial drugs. Critically, parasites are also evolving to evade detection by rapid diagnostic tests (RDTs), hindering timely diagnosis and treatment.
Time.news: Let’s talk about hope. The article highlights new tools like malaria vaccines and next-generation mosquito nets. How game-changing are these advancements?
Dr. Aris Thorne: These advancements are crucial. The RTS,S and R21 malaria vaccines mark a monumental achievement. Clinical trials have shown they can significantly reduce cases and deaths, especially among children. Their deployment across African countries addresses a critical need. Next-generation mosquito nets, such as dual-insecticide nets, are designed to overcome insecticide resistance, offering a renewed layer of protection. But these aren’t silver bullets; they need to be used strategically and in conjunction with other vector control methods.
Time.news: The article also mentions innovative vector control strategies like attractive toxic sugar baits (ATSBs) and genetic modification of mosquitoes. Are these feasible on a large scale?
Dr. Aris Thorne: They hold immense potential, especially as we grapple with resistance. ATSBs are environmentally pleasant and can target resistant mosquitoes. Biological control using modified gut bacteria is another promising avenue.Genetic modification, while still under development, offers a targeted approach to reducing mosquito populations. However, these methods are relatively new and require further research and careful implementation to ensure safety and effectiveness. Public acceptance is also critical for prosperous deployment.
Time.news: The U.S. plays a vital role in the global fight against malaria. Can you elaborate on American involvement and its impact?
Dr. Aris Thorne: The U.S., through USAID and the CDC, is a major funder of malaria control programs globally. The President’s Malaria Initiative (PMI) has had a notable impact, providing insecticide-treated nets, antimalarial drugs, and diagnostic tools. American universities and research institutions are also at the forefront of malaria research, developing new vaccines, drugs, and vector control strategies. Continued U.S. support is essential for sustaining progress and accelerating malaria eradication efforts.
time.news: what’s yoru perspective on artemisinin-based tritherapies and Ganaplacide-Lumenfantrine as new options for antimalarial drugs?
Dr. Aris Thorne: I see these new medicines as really encouraging developments in the fight against malaria. Artemisinin-based tritherapies are a very welcome addition, and they’ve proven to be highly effective in recent trials throughout Africa and Asia. Ganaplacide-Lumenfantrine has also demonstrated strong effectiveness against malaria parasites,notably amongst young children. Even more importantly,its artemisinin-free formula makes it an ideal candidate for fighting the rising tide of artemisinin-resistance in malaria. Both of these options should serve as potent tools in doctors’ kits for years to come.
Time.news: What can our readers do to contribute to the fight against malaria?
Dr. Aris Thorne: There are several ways to get involved. Supporting organizations like the Against Malaria Foundation (AMF) or Malaria No More is a great start. These organizations are highly effective at distributing insecticide-treated nets and advocating for increased funding. Raising awareness about malaria in your community and supporting policies that prioritize global health are also critical. Every contribution, no matter how small, can make a difference.
Time.news: The article concludes with a reader poll asking about optimism for achieving a malaria-free world in their lifetime. What’s your take?
Dr.Aris Thorne: I remain cautiously optimistic. The challenges are undeniable, but the scientific advancements and increased global commitment give me hope. Eradicating malaria is an enterprising goal,but one worth pursuing. It requires sustained investment, innovation, and collaboration.As long as we continue to prioritize research, strengthen health systems, and engage communities, we can make significant progress towards a malaria-free world.