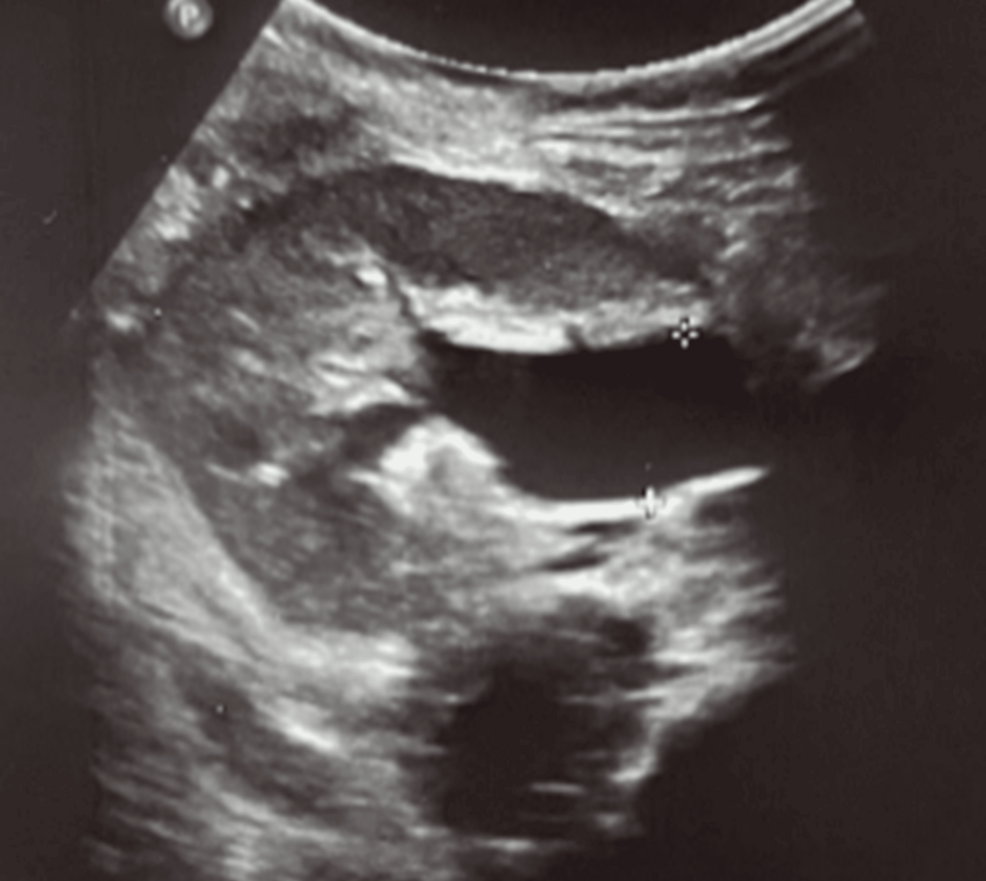
For a child awaiting a kidney transplant, the surgery is more than a medical procedure; it is a return to a semblance of normal childhood. But in the delicate months and years following the operation, a subtle, often invisible complication can threaten the longevity of the new organ. Clinicians call it partial distal ureteral obstruction—a narrowing or blockage at the lower end of the ureter where it connects to the bladder.
Unlike a complete blockage, which triggers immediate and obvious alarms, partial distal ureteral obstruction after pediatric kidney transplantation is a diagnostic challenge that often masquerades as other, more common post-surgical issues. Since the symptoms can be vague and the imaging inconclusive, the window between detection and permanent graft damage is perilously small.
The ureter is the vital conduit that carries urine from the transplanted kidney to the bladder. In pediatric cases, the surgical connection—the ureteroneocystostomy—is particularly complex due to the small scale of the patient’s anatomy. When this connection narrows, urine backs up into the kidney, increasing pressure within the renal pelvis and potentially triggering a decline in graft function.
The Stealth Nature of Partial Obstruction
The primary difficulty in diagnosing partial obstruction lies in its subtlety. In a total obstruction, the kidney swells rapidly, a condition known as hydronephrosis, which is easily spotted on a standard ultrasound. Still, in partial cases, the urine may still trickle through, meaning the kidney may not appear significantly dilated on initial scans.
Medical teams often uncover themselves navigating a “diagnostic maze” when a pediatric patient presents with a gradual rise in serum creatinine—the primary marker of kidney function. In the high-stakes environment of transplant care, this rise is frequently attributed to acute cellular rejection or drug toxicity from immunosuppressants. These are the “usual suspects,” and treating them first is standard protocol. However, if the root cause is actually a mechanical obstruction, immunosuppressive treatments will fail, and the graft will continue to deteriorate.
According to clinical guidelines from the National Kidney Foundation, maintaining the patency of the urinary tract is as critical as preventing immune rejection. When the drainage is compromised, the resulting pressure can lead to atrophy of the renal parenchyma, the functional tissue of the kidney.
Recognizing the Red Flags
While the signs are subtle, there are specific clinical indicators that should prompt a deeper investigation into the distal ureter:
- Isolated Creatinine Creep: A slow, steady increase in creatinine levels that does not respond to standard adjustments in anti-rejection medication.
- Low-Grade Fever: Obstruction often leads to urinary stasis, which increases the risk of urinary tract infections (UTIs). A recurring fever without a clear source can be a telltale sign.
- Flank Pain: While difficult to communicate in extremely young children, tenderness or discomfort in the area of the transplant can indicate pressure buildup.
- Fluctuating Urine Output: Changes in the volume or frequency of urination that do not align with fluid intake.
Navigating the Diagnostic Toolkit
When a clinician suspects a partial blockage, they must move beyond the basic ultrasound. The diagnostic process typically follows a sequence of increasing invasiveness to pinpoint the location and severity of the obstruction.
A diuretic renogram, often using a tracer like Technetium-99m MAG3, is frequently the next step. By administering a diuretic, doctors can determine if the kidney is simply slow to drain or if there is a physical barrier preventing the flow of urine. This functional imaging provides a more accurate picture of the “washout” time than a static image can offer.
In cases where imaging remains ambiguous, the gold standard for diagnosis is often a retrograde pyelogram or a cystoscopy. These procedures allow surgeons to visualize the anastomosis directly and check for strictures—narrowed areas of the ureter caused by scar tissue or surgical kinking.
| Tool | What it Detects | Limitation |
|---|---|---|
| Ultrasound | Gross hydronephrosis | May miss partial/mild blockages |
| MAG3 Scan | Urinary flow and function | Requires specialized nuclear medicine |
| CT Urography | Anatomical narrowing | Radiation exposure in children |
| Cystoscopy | Direct visual of the blockage | Invasive; requires sedation/anesthesia |
Treatment and Long-Term Graft Survival
Once a partial distal ureteral obstruction is confirmed, the goal is immediate decompression. The most common intervention is the placement of a ureteral stent—a thin, flexible tube that holds the ureter open and allows urine to bypass the blockage.
For some children, the stent provides a temporary fix, allowing the inflammation to subside. For others, a more permanent surgical revision of the ureteroneocystostomy is required. This involves removing the narrowed segment of the ureter and re-attaching it to the bladder to ensure a wide, unobstructed opening.
The long-term success of a pediatric kidney transplant depends heavily on early detection. When obstruction is caught early, the kidney can often recover fully. However, chronic obstruction leads to irreversible fibrosis, effectively “suffocating” the graft from the inside out.
Ongoing monitoring remains the best defense. Pediatric transplant teams typically employ a rigorous schedule of follow-up blood work and imaging to catch these “silent” obstructions before they manifest as graft failure. For parents and caregivers, the key is vigilance regarding any change in the child’s energy levels, temperature, or urinary habits.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult a board-certified pediatric nephrologist or transplant surgeon for diagnosis and treatment.
Medical researchers are currently exploring the apply of biodegradable stents and advanced robotic-assisted revisions to reduce the trauma of repeat surgeries in pediatric patients. Further data on the efficacy of these new techniques is expected in upcoming clinical trial reports later this year.
Do you have experience navigating pediatric transplant recovery? Share your thoughts or questions in the comments below.