For decades, the clinical approach to obesity was defined by a frustratingly simple metric: the Body Mass Index (BMI). Patients were often told to “eat less and move more,” a directive that ignored the complex endocrine and genetic drivers of weight gain. However, a new framework from the European Association for the Study of Obesity (EASO), published May 13, 2026, in Nature Medicine, signals a definitive shift toward a more nuanced, pharmacological approach that treats obesity not as a lifestyle failure, but as a chronic metabolic disease.
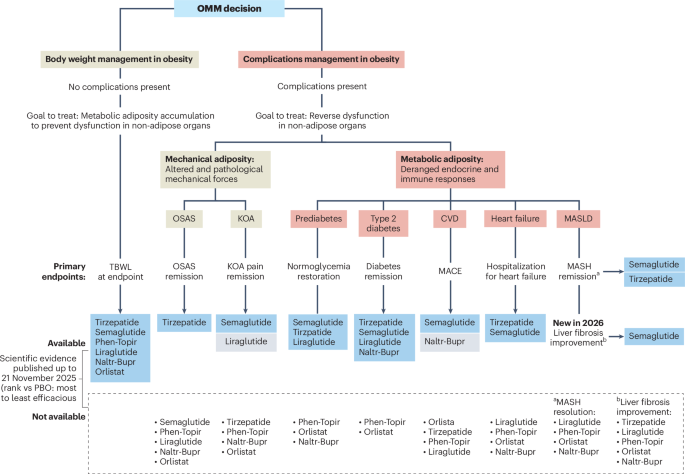
The 2026 update refines the EASO treatment algorithm, moving beyond simple weight loss targets to prioritize the resolution of obesity-related complications. Most notably, the framework integrates new trial evidence regarding the intersection of obesity and liver disease, specifically Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) and its more severe form, MASH. By shifting the goalpost from the scale to the organ, the guidelines provide clinicians with a roadmap for using pharmacological interventions to prevent irreversible systemic damage.
As a physician, I have seen the gap between clinical guidelines and the reality of the exam room. For too long, the “treatment” for obesity was a suggestion of willpower. The EASO update acknowledges that for many, the biological set point of the body resists weight loss. By formalizing the use of emerging drug classes—including dual and triple incretin agonists—the framework legitimizes the use of medicine to reset metabolic homeostasis, provided it is paired with comprehensive lifestyle support.
Prioritizing Metabolic Health Over the Scale
The core of the 2026 EASO update is the transition toward a “complications-led” treatment model. While weight reduction remains a primary goal, the framework emphasizes that the quality of weight loss—specifically the reduction of ectopic fat in the liver and pancreas—is a more critical predictor of long-term survival than the total number of kilograms lost.
The updated algorithm suggests that patients with high-risk comorbidities, such as Type 2 diabetes or advanced liver fibrosis, should be fast-tracked to more potent pharmacological interventions. This is a departure from older models that required patients to “fail” multiple rounds of diet and exercise before qualifying for medication. The EASO now argues that delaying pharmacological intervention in high-risk patients may lead to preventable organ failure, particularly in the liver.
The integration of liver disease data is perhaps the most significant addition to the 2026 framework. Recent trials have demonstrated that the newest generation of obesity medications does more than suppress appetite; they actively reduce hepatic inflammation and fibrosis. This transforms the pharmacological treatment of obesity into a preventative strategy against cirrhosis and hepatocellular carcinoma.
The Evolution of the Pharmacological Toolkit
The EASO framework categorizes the current pharmacological landscape by efficacy and metabolic impact. The shift has moved rapidly from older, sympathomimetic drugs to the sophisticated incretin mimetics that dominate the current conversation. The 2026 update specifically addresses the titration and sequencing of these agents to maximize efficacy while minimizing gastrointestinal side effects.

The framework highlights the emergence of “triple agonists”—drugs that target the GLP-1, GIP, and glucagon receptors simultaneously. These agents are noted for their ability to produce weight loss results that previously required bariatric surgery, while simultaneously improving insulin sensitivity and reducing liver fat. The EASO guidelines provide a structured sequence for these medications, recommending they be reserved for patients who do not respond to dual agonists or those with severe metabolic dysfunction.
| Drug Class | Primary Mechanism | Key Clinical Focus | Liver Impact |
|---|---|---|---|
| GLP-1 Receptor Agonists | Satiety & Insulin secretion | Weight loss & Glucose control | Moderate reduction in fat |
| Dual Agonists (GLP-1/GIP) | Synergistic metabolic regulation | Enhanced weight loss | Significant reduction in steatosis |
| Triple Agonists (GLP-1/GIP/GCG) | Energy expenditure & Satiety | Severe obesity & Metabolic syndrome | High impact on fibrosis/inflammation |
Implementation Challenges and Stakeholder Impact
While the clinical roadmap is clear, the practical application of the EASO 2026 framework faces significant headwinds. The primary tension lies between clinical necessity and healthcare accessibility. For patients, the promise of these medications is life-changing, but the cost and supply chain instabilities of newer agonists remain a barrier to equitable care.
Healthcare providers are now tasked with a more complex role: they must act as metabolic managers, monitoring not just weight, but liver enzymes, cardiovascular markers, and muscle mass preservation. The EASO framework warns against “sarcopenic obesity”—where rapid weight loss leads to a dangerous loss of lean muscle—and recommends the integration of resistance training and high-protein nutrition as a mandatory adjunct to pharmacological therapy.
Insurance providers and national health systems are also key stakeholders. The 2026 guidelines provide the evidentiary basis for these entities to shift their coverage models. By framing obesity medication as a means to prevent expensive future interventions—such as liver transplants or dialysis—the EASO is making a financial argument for early and aggressive pharmacological treatment.
What Remains Unknown
Despite the progress, the framework acknowledges critical gaps in the data. The long-term “maintenance” phase of these medications is still under scrutiny. It remains unclear whether patients can sustain their metabolic gains after discontinuing these drugs, or if the current pharmacological trajectory necessitates lifelong therapy to prevent weight regain and the return of liver dysfunction.
the interaction between these medications and other chronic disease treatments—such as chemotherapy or immunosuppressants—requires more robust, real-world evidence. The EASO calls for more diverse longitudinal studies to ensure that the treatment algorithm is effective across different ethnicities and genetic backgrounds.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next major milestone for the obesity community will be the upcoming 2027 Global Metabolic Summit, where the results of multi-year longitudinal studies on triple agonists are expected to be presented. These findings will likely dictate whether the EASO framework moves toward an even more aggressive “first-line” pharmacological approach for all patients with a BMI over 30 and metabolic dysfunction.
We want to hear from you. How have these evolving guidelines changed your approach to health or your conversations with your doctor? Share your thoughts in the comments below.