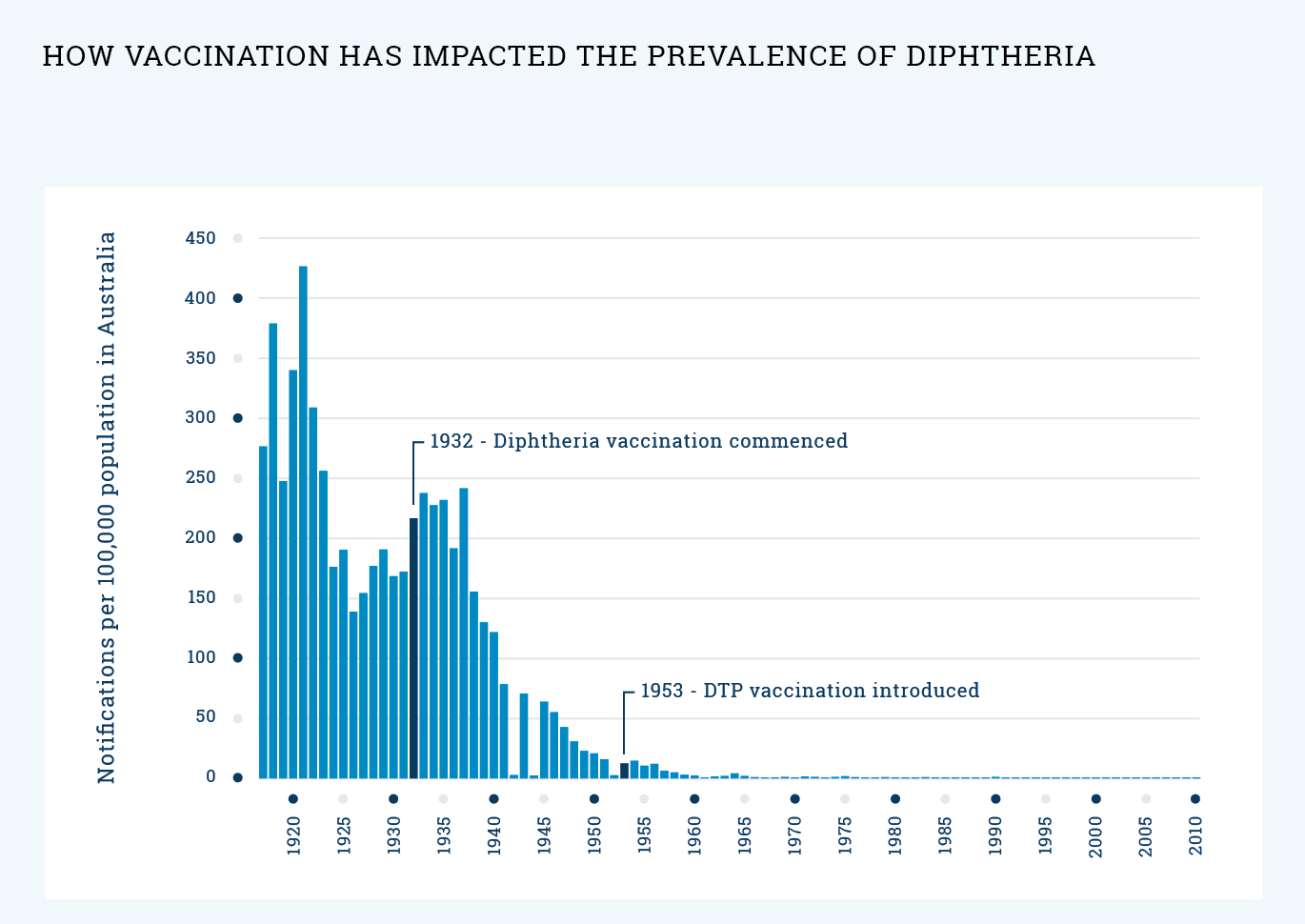
Health officials in Australia are responding to a diphtheria outbreak in Northern Territory remote communities, marking a stark return of a disease that had been largely dormant in the region for decades. The situation has turned critical with the report of the country’s first diphtheria-related death in nearly ten years, an event that underscores the fragility of immunity in isolated populations.
The death, which occurred several weeks ago in a remote area, serves as a grim reminder that vaccine-preventable diseases can resurface when gaps in healthcare access and immunization schedules widen. While Australia has long maintained high childhood vaccination rates, this latest cluster suggests a dangerous decline in adult immunity and a failure in the delivery of critical booster shots to the most vulnerable citizens.
According to reports from health authorities, the Northern Territory declared an outbreak in March, the first of its kind since the 1990s. Nationwide, approximately 161 cases have been reported, with more than 100 of those concentrated within the Territory. The impact has been disproportionately severe among Indigenous residents, who account for more than 98 percent of locally acquired cases, primarily in outer regional and remote areas.
The Clinical Danger of Diphtheria
As a physician, I view diphtheria not merely as a historical footnote, but as a potent bacterial infection caused by Corynebacterium diphtheriae. The bacteria produce a toxin that affects the respiratory system and can lead to the formation of a thick, gray pseudomembrane in the throat. This membrane can obstruct the airway, leading to respiratory failure—the primary cause of death in severe cases.

The disease is highly contagious, spreading through respiratory droplets or direct contact with infected lesions. If left untreated, the toxin can enter the bloodstream, causing myocarditis (inflammation of the heart muscle) or neuropathy (nerve damage), which can lead to paralysis. Because the World Health Organization classifies diphtheria as a vaccine-preventable disease, these fatalities are entirely avoidable with a consistent immunization strategy.
Addressing the Immunity Gap in Remote Communities
The concentration of this outbreak in remote Indigenous communities highlights a persistent disparity in public health outcomes. While the initial childhood series of the DTP (diphtheria, tetanus, and pertussis) vaccine is widely administered, immunity is not lifelong. It wanes over time, necessitating booster doses during adolescence and every ten years into adulthood.
Medical experts indicate that the most severe cases in the current outbreak are appearing among individuals who are either completely unvaccinated or significantly overdue for their boosters. Several systemic factors have contributed to this vulnerability:
- Access Barriers: The geographic isolation of remote communities often makes the consistent delivery of healthcare and scheduled vaccinations a logistical challenge.
- Post-Pandemic Hesitancy: The aftermath of the COVID-19 pandemic saw a global rise in vaccine skepticism, which often bleeds into the acceptance of routine immunizations.
- Healthcare Disruption: Pandemic-era lockdowns and resource reallocation may have led to missed appointments for adult boosters.
Standard Australian Immunization Timeline
To understand where the gaps occur, it is helpful to look at the recommended Australian Government Department of Health guidelines for diphtheria protection.
| Life Stage | Vaccination Requirement | Purpose |
|---|---|---|
| Infancy/Childhood | Primary series (multiple doses) | Establish baseline immunity |
| Adolescence | Booster dose | Reinforce waning childhood immunity |
| Adulthood | Booster every 10 years | Maintain lifelong protection |
The Path Toward Containment
Containment of the current outbreak requires a two-pronged approach: immediate case management and a long-term restoration of trust in preventative medicine. Health officials are currently working to identify close contacts of infected individuals to provide prophylactic antibiotics and emergency vaccinations.
Beyond the immediate crisis, there is a pressing need for “catch-up” clinics in the Northern Territory. For those in remote areas, this means moving away from centralized clinics and toward mobile health units that can reach the most isolated residents. Addressing the 98 percent infection rate among Indigenous populations requires culturally safe healthcare delivery that acknowledges the historical distrust some communities may feel toward government medical interventions.
For those residing in or traveling to the Northern Territory, it is advisable to check your immunization history. If it has been more than a decade since your last tetanus-diphtheria-pertussis shot, a booster is clinically indicated to prevent infection and transmission.
Disclaimer: This article is for informational purposes only and does not constitute individual medical advice. Please consult a licensed healthcare provider for vaccination guidance and medical diagnosis.
Health authorities are expected to provide further updates on case numbers and the progress of the vaccination drive as the outbreak response continues through the winter months. We will monitor the official reports from NT Health for further developments.
Do you have questions about vaccine boosters or healthcare access in remote areas? Share your thoughts in the comments or share this article to help spread awareness.