For decades, the prevailing medical assumption was that sleep was a state of biological inactivity—a period where the brain and body simply “powered down” to conserve energy. We viewed it as the absence of wakefulness, a passive gap in our conscious lives that could be trimmed or sacrificed in the pursuit of productivity.
However, modern neuroscience has revealed a far more dynamic reality. Sleep is not a void, but an intensely active physiological process. Far from shutting down, the brain engages in a series of critical maintenance tasks that are impossible to perform while we are awake. From flushing out metabolic waste to restructuring our memories, sleep is the primary mechanism the body uses to ensure long-term survival and cognitive integrity.
As a physician, I have seen the downstream effects of treating sleep as an optional luxury. When we deprive ourselves of rest, we aren’t just feeling “tired”; we are actively inhibiting the brain’s ability to clean itself and the body’s ability to repair its most basic cellular structures. The cost of this deficit is not merely a foggy morning, but a systemic breakdown of neurological and physical health.
The Brain’s Midnight Cleaning Crew
One of the most significant breakthroughs in sleep science is the discovery of the glymphatic system. While the rest of the body relies on the lymphatic system to clear waste, the brain—protected by the blood-brain barrier—requires a specialized mechanism. During deep sleep, the space between brain cells increases, allowing cerebrospinal fluid to flush through the brain’s tissues more efficiently.
This “power wash” removes metabolic byproducts that accumulate during the day, including beta-amyloid, a protein associated with the development of Alzheimer’s disease. When we cut sleep short, this cleaning cycle is interrupted. The resulting buildup of cellular debris can impair neuronal communication and, over years of chronic deprivation, may contribute to the onset of neurodegenerative diseases.
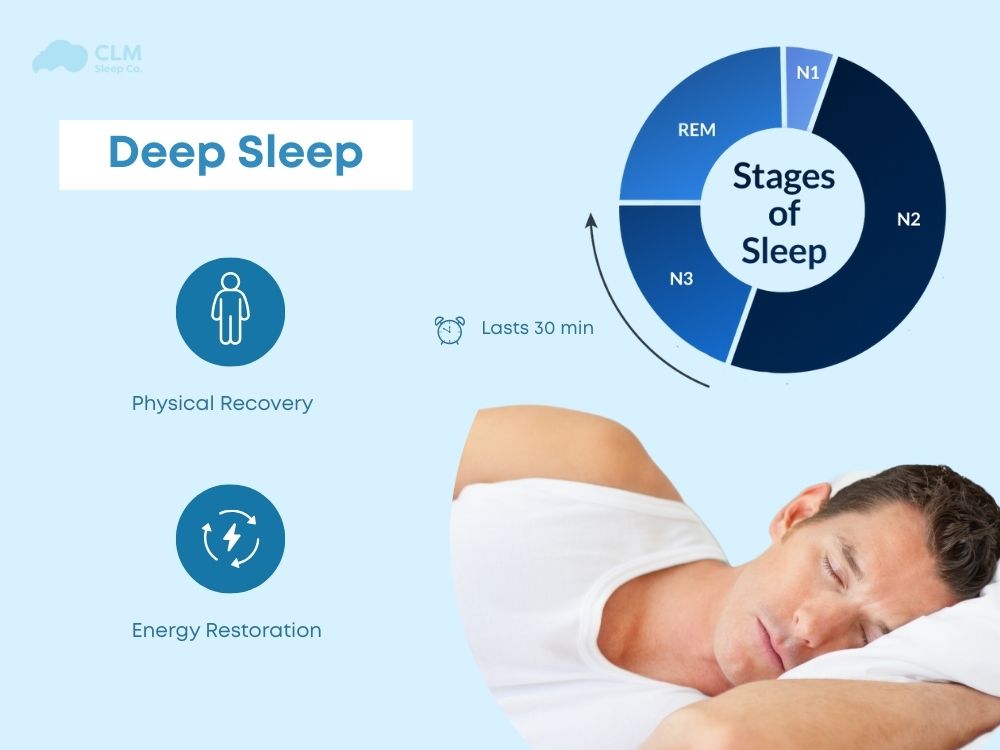
This process is most efficient during non-rapid eye movement (NREM) sleep, particularly the deep-sleep stages. This represents why a few hours of fragmented sleep cannot replace the restorative value of a full night’s rest; the brain requires specific, uninterrupted cycles to complete its chemical housekeeping.
The Architecture of Memory and Learning
Beyond physical cleaning, sleep serves as the brain’s primary filing system. Throughout the day, we encounter a deluge of information that is stored in the hippocampus—a region of the brain that acts as a short-term buffer. However, the hippocampus has limited capacity. To make room for new information, the brain must move these memories into the neocortex for long-term storage.
This process, known as memory consolidation, happens primarily during sleep. The brain doesn’t just save everything; it selectively strengthens vital connections and “prunes” irrelevant ones. This synaptic pruning is essential for learning. Without it, the brain would become saturated with noise, making it nearly impossible to distinguish critical patterns from random data.
The different stages of sleep handle different types of processing:
- Deep Sleep: Primarily focuses on declarative memory, such as facts, names, and dates.
- REM Sleep: Plays a critical role in emotional regulation and procedural memory, helping us process complex experiences and refine skills.
The Systemic Toll of Sleep Deprivation
The consequences of ignoring these biological mandates extend far beyond the mind. Sleep is a systemic requirement. During sleep, the endocrine system releases growth hormones essential for tissue repair and muscle growth. Simultaneously, the immune system produces cytokines, proteins that help the body fight infection and inflammation.
When sleep is chronically restricted, the body enters a state of stress. Cortisol levels remain elevated, which can lead to insulin resistance and an increased risk of Type 2 diabetes. The lack of REM sleep often manifests as emotional instability, as the amygdala—the brain’s emotional center—becomes hyper-reactive without the calming influence of nocturnal processing.
| Duration of Loss | Primary Cognitive Impact | Physical/Systemic Effect |
|---|---|---|
| 24 Hours | Impaired judgment, slowed reaction time | Increased cortisol, mild glucose intolerance |
| 48 Hours | “Microsleeps” (uncontrollable brief naps) | Significant immune system suppression |
| 72+ Hours | Hallucinations, severe cognitive fragmentation | Extreme hormonal imbalance, cardiovascular stress |
| Chronic (Long-term) | Increased risk of dementia/Alzheimer’s | Obesity, hypertension, heart disease |
Practical Steps for Sleep Hygiene
While the science of sleep is complex, the application is straightforward. To optimize the glymphatic system and memory consolidation, the goal is to maximize the quality and consistency of sleep cycles. Medical consensus suggests several evidence-based adjustments:

- Maintain a Consistent Wake Time: This anchors the circadian rhythm, making it easier to fall asleep at a set time each night.
- Optimize Light Exposure: Seek bright sunlight within 30 minutes of waking to trigger cortisol release and set the timer for melatonin production later in the evening.
- Cool the Environment: A slight drop in core body temperature is a biological signal that it is time to sleep; a cool room (around 65°F or 18°C) typically facilitates this.
- Limit Blue Light: Screen use before bed suppresses melatonin, tricking the brain into thinking it is still daytime.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult a healthcare provider for diagnosis or treatment of sleep disorders.
The scientific community is currently shifting its focus toward “precision sleep”—the study of how individual genetic markers influence sleep needs and the development of targeted therapies for insomnia and apnea. As we uncover more about the relationship between sleep and longevity, the societal view of rest is likely to evolve from a sign of weakness to a recognized pillar of peak performance.
We want to hear from you. Have you noticed a tangible difference in your cognitive clarity after improving your sleep habits? Share your experience in the comments or share this article with someone who treats sleep as an afterthought.