It often begins as a sudden, inexplicable tightening in the chest or a sharp spike in heart rate. Within seconds, the world can feel as though This proves closing in, accompanied by a dizzying sense of detachment or an overwhelming conviction that something catastrophic is happening. For those experiencing a panic attack, the sensation is not merely psychological; it is a visceral, full-body takeover that can feel indistinguishable from a medical emergency.
While the experience is terrifying, the biological reality is a paradox: a panic attack is essentially a survival mechanism functioning perfectly, but at the wrong time. It is the body’s “fight-or-flight” response—a system evolved to save ancestors from predators—triggering in the absence of an actual physical threat. When this system misfires, the brain perceives a crisis where there is none, flooding the body with chemicals designed for immediate action, not sedentary endurance.
Understanding the mechanics of this response is the first step in dismantling its power. By shifting the perspective from “I am dying” to “my amygdala is overreacting,” individuals can begin to employ specific physiological and cognitive tools to signal to their brain that the danger has passed. The goal is not to fight the panic—which often fuels the fire—but to steer the nervous system back toward a state of equilibrium.
The Biological Misfire: When Survival Instincts Overreach
The catalyst for a panic attack resides in the amygdala, a small, almond-shaped structure in the brain that acts as a sentinel for danger. When the amygdala detects a threat—whether it is a genuine physical hazard or a perceived emotional stressor—it sends an immediate distress signal to the hypothalamus. This trigger initiates a cascade of events through the sympathetic nervous system, designed to prepare the body for an explosive burst of energy.
The adrenal glands release a surge of epinephrine (adrenaline), which causes the heart to beat faster to pump more oxygenated blood to the large muscles. Simultaneously, the respiratory system shifts; breathing becomes shallow and rapid to maximize oxygen intake. However, in a non-emergency setting, this rapid breathing leads to a drop in carbon dioxide levels in the blood, resulting in the lightheadedness, tingling in the extremities, and chest tightness that often lead people to fear they are having a heart attack.
This physiological state creates a dangerous feedback loop. The physical sensations of panic are interpreted by the mind as evidence of a crisis, which in turn signals the amygdala to release more adrenaline. This “fear of the fear” is what transforms a momentary spike of anxiety into a full-scale panic attack.
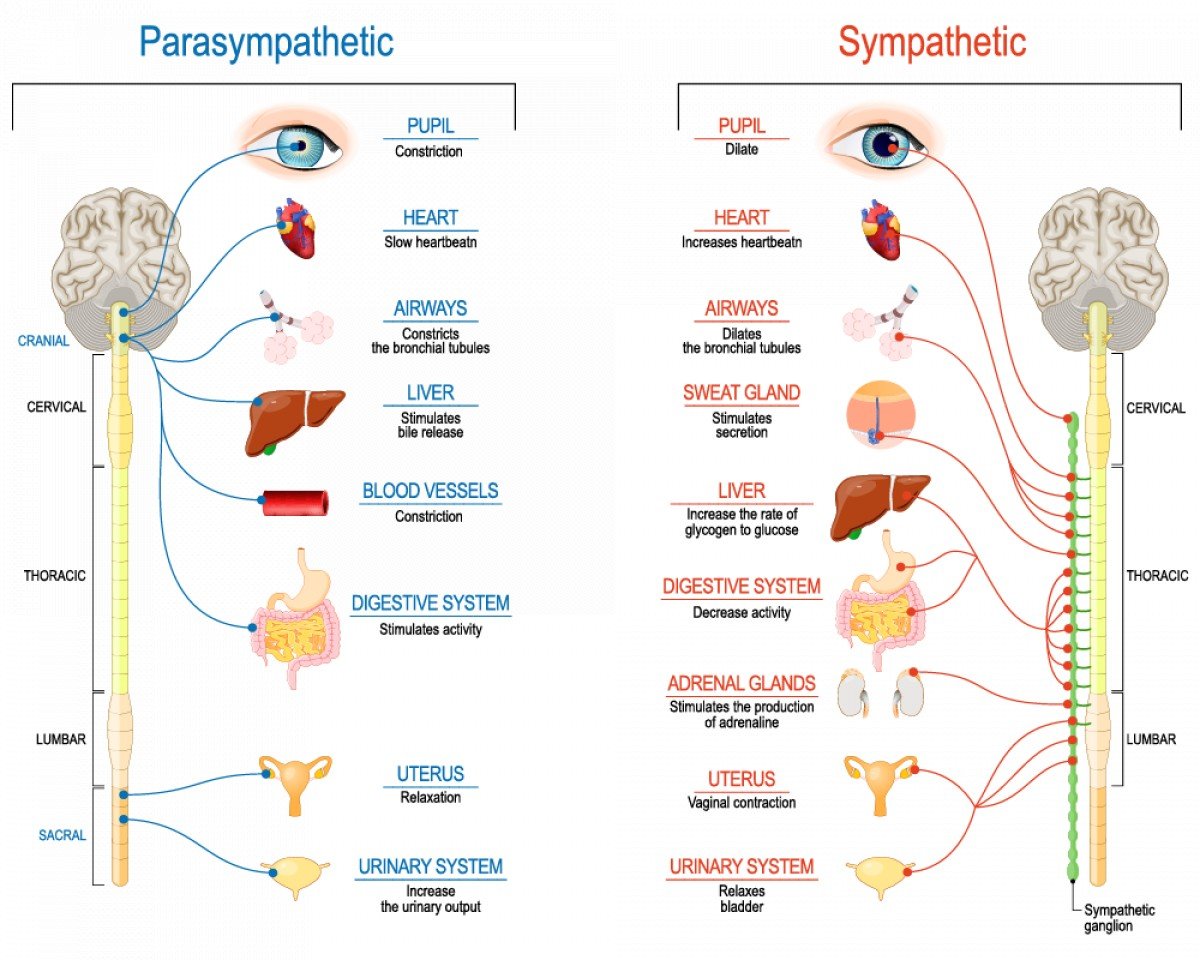
Sympathetic vs. Parasympathetic Response
To stop a panic attack, one must consciously shift the body from the sympathetic nervous system (the accelerator) to the parasympathetic nervous system (the brake). The following table outlines the primary differences in how these two systems affect the body during a stress event.
| Physiological Function | Sympathetic (Fight-or-Flight) | Parasympathetic (Rest-and-Digest) |
|---|---|---|
| Heart Rate | Rapid increase; pounding | Slows to baseline |
| Respiration | Rapid, shallow (hyperventilation) | Slow, deep, rhythmic |
| Blood Flow | Redirected to skeletal muscles | Redirected to digestive organs |
| Mental State | Hyper-vigilance; tunnel vision | Calm; expanded awareness |
Practical Interventions: Breaking the Feedback Loop
Because a panic attack is a physiological event, the most effective ways to stop it are often physiological. The objective is to provide the brain with “bottom-up” evidence that the body is safe, which eventually overrides the “top-down” panic signal from the amygdala.
Controlled Breathing and the CO2 Balance
The most immediate tool is the regulation of breath. Since hyperventilation causes the dizziness and tingling associated with panic, slowing the breath helps restore the balance of carbon dioxide in the blood. Techniques such as “box breathing”—inhaling for four seconds, holding for four, exhaling for four, and holding for four—force the diaphragm to engage and signal the vagus nerve to activate the parasympathetic response.
The 5-4-3-2-1 Grounding Method
Panic often causes a sense of derealization, where the person feels detached from their surroundings. Grounding techniques pull the mind out of the internal spiral and back into the physical environment. The 5-4-3-2-1 method is a gold standard for this process:
- 5: Acknowledge five things you see around you (e.g., a clock, a tree, a blue pen).
- 4: Acknowledge four things you can touch (e.g., the fabric of your clothes, a cold tabletop).
- 3: Acknowledge three things you hear (e.g., traffic outside, a humming refrigerator).
- 2: Acknowledge two things you can smell (or two smells you enjoy).
- 1: Acknowledge one thing you can taste (or the current taste in your mouth).
Cognitive Reframing and Acceptance
Attempting to “force” a panic attack to stop often increases anxiety because it treats the panic as a threat that must be defeated. Instead, psychologists recommend a strategy of paradoxical acceptance. By acknowledging the sensation—“My heart is racing and I feel dizzy because my body is in fight-or-flight mode, and while Here’s uncomfortable, it is not dangerous”—the individual strips the attack of its power. This shift from resistance to observation prevents the feedback loop from escalating.

Identifying the Stakes: When to Seek Professional Help
While occasional panic attacks can be triggered by acute stress or grief, recurring attacks without an obvious trigger may indicate Panic Disorder or other anxiety-related conditions. The primary danger of untreated panic attacks is not the attacks themselves—which are not physically lethal—but the “avoidance behavior” they create. People may begin avoiding places where they previously had an attack, leading to agoraphobia and a significantly diminished quality of life.
Clinical interventions, such as Cognitive Behavioral Therapy (CBT), are highly effective. CBT helps patients identify the distorted thought patterns that trigger the amygdala and uses “exposure therapy” to desensitize the body to the physical sensations of panic, effectively retraining the brain’s alarm system.
Disclaimer: This content is for informational purposes only and does not constitute medical advice. If you are experiencing chest pain or shortness of breath, seek immediate medical attention to rule out cardiac or respiratory emergencies.
The next step for those experiencing frequent episodes is typically a consultation with a licensed mental health professional or primary care physician to establish a diagnostic baseline. Many find that a combination of mindfulness-based stress reduction (MBSR) and professional therapy provides long-term resilience against future episodes.
Do you have a grounding technique that works for you? Share your experience in the comments below or share this guide with someone who might need it.

