The intersection of kidney disease and systemic vasculitis presents a complex challenge for clinicians, particularly in patients already reliant on dialysis. A recent case report published in Cureus details the unusual presentation of systemic IgA vasculitis with leukocytoclastic features in a 68-year-old man with pre-existing primary IgA nephropathy who was dependent on hemodialysis. This case highlights the need for heightened awareness of atypical presentations of vasculitis in vulnerable patient populations.
IgA nephropathy, also known as Berger’s disease, is a common form of glomerulonephritis – inflammation of the kidney’s filtering units – worldwide. It’s characterized by deposits of immunoglobulin A (IgA) in the glomeruli. Over time, this can lead to kidney failure, necessitating dialysis. Systemic IgA vasculitis, formerly known as Henoch-Schönlein purpura, is a systemic inflammatory condition involving small blood vessels, often affecting the skin, joints, gut, and kidneys. Although typically seen in children, it can occur in adults, and its presentation can be varied. The National Kidney Foundation provides comprehensive information on Henoch-Schönlein purpura and its impact on kidney health.
Atypical Presentation in a Dialysis Patient
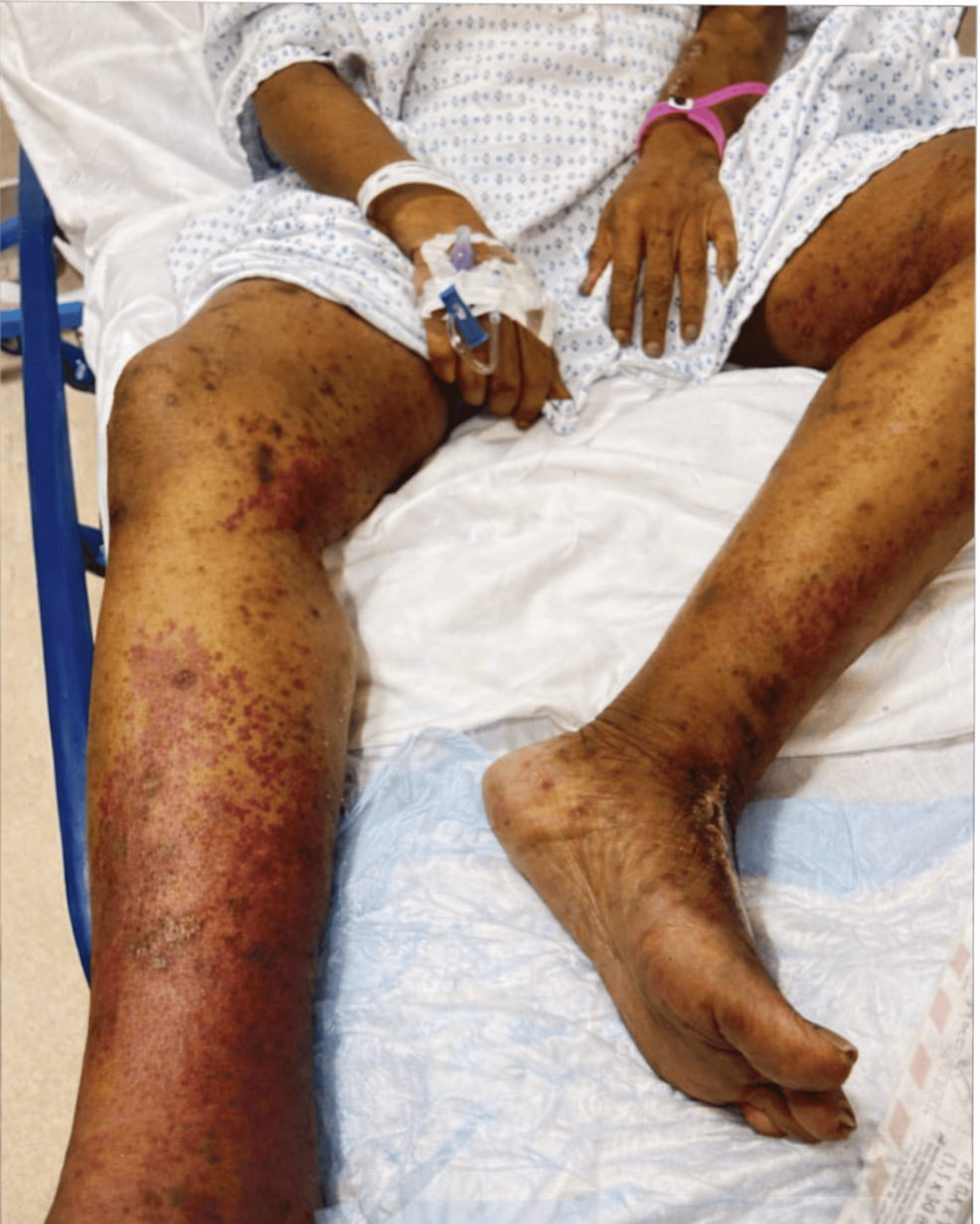
The patient in this case, as detailed in the Cureus report, initially presented with a skin rash and joint pain. However, unlike typical presentations of IgA vasculitis, he lacked gastrointestinal involvement. Crucially, the skin biopsy revealed leukocytoclastic vasculitis – inflammation of small blood vessels with fragments of white blood cells – alongside IgA deposits. This finding, coupled with his history of IgA nephropathy and dialysis dependence, prompted further investigation. The patient had been undergoing hemodialysis for approximately five years prior to the onset of these recent symptoms.
According to the report, laboratory tests showed elevated inflammatory markers, including C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR), indicating systemic inflammation. Renal biopsy, though challenging in a dialysis-dependent patient, confirmed the presence of IgA deposits and vasculitic changes in the remaining kidney tissue. The authors emphasize that the atypical presentation – the absence of gastrointestinal symptoms and the leukocytoclastic vasculitis – made the diagnosis less straightforward.
Diagnostic Challenges and Treatment Considerations
Diagnosing vasculitis in patients with pre-existing kidney disease can be particularly difficult. The symptoms of vasculitis can overlap with those of kidney disease itself, and the inflammatory markers can be chronically elevated in dialysis patients. The American College of Rheumatology offers detailed information about different types of vasculitis and their symptoms.
The patient was treated with a course of corticosteroids, a common approach to managing systemic IgA vasculitis. The report indicates that his symptoms improved with treatment, although the long-term prognosis remains uncertain. The authors note the importance of careful monitoring for potential complications, such as infections, which are more common in patients receiving immunosuppressive therapy. They also highlight the need to balance the benefits of immunosuppression with the risks of worsening kidney function.
The Significance of Early Recognition
This case underscores the importance of considering systemic IgA vasculitis in the differential diagnosis of any new symptom – such as a skin rash or joint pain – in patients with IgA nephropathy, even those on dialysis. Early recognition and prompt treatment can potentially prevent disease progression and improve outcomes. The authors suggest that clinicians should have a high index of suspicion for vasculitis in this patient population and be prepared to perform appropriate diagnostic tests, including skin biopsies and renal biopsies when feasible.
The interplay between primary IgA nephropathy and the development of systemic IgA vasculitis is not fully understood. Some researchers believe that the underlying immune dysregulation in IgA nephropathy may predispose individuals to developing systemic vasculitis. Further research is needed to elucidate the mechanisms underlying this association and to identify potential therapeutic targets.
The case also raises questions about the optimal management of systemic IgA vasculitis in dialysis-dependent patients. Traditional treatment regimens may need to be modified to account for the unique challenges posed by kidney failure and the increased risk of complications. The authors advocate for a multidisciplinary approach involving nephrologists, rheumatologists, and dermatologists to ensure comprehensive care.
As medical understanding of autoimmune and inflammatory conditions evolves, cases like this one serve as critical learning opportunities. The authors emphasize the need for continued vigilance and a willingness to consider atypical presentations, particularly in complex patient populations.
Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with a qualified healthcare professional for diagnosis and treatment of any medical condition.
The next step in understanding this complex interplay will likely involve larger-scale studies investigating the prevalence of systemic IgA vasculitis in patients with IgA nephropathy and evaluating the effectiveness of different treatment strategies. If you have concerns about kidney health or vasculitis, please discuss them with your doctor. Share this article with others who may find it helpful, and join the conversation in the comments below.