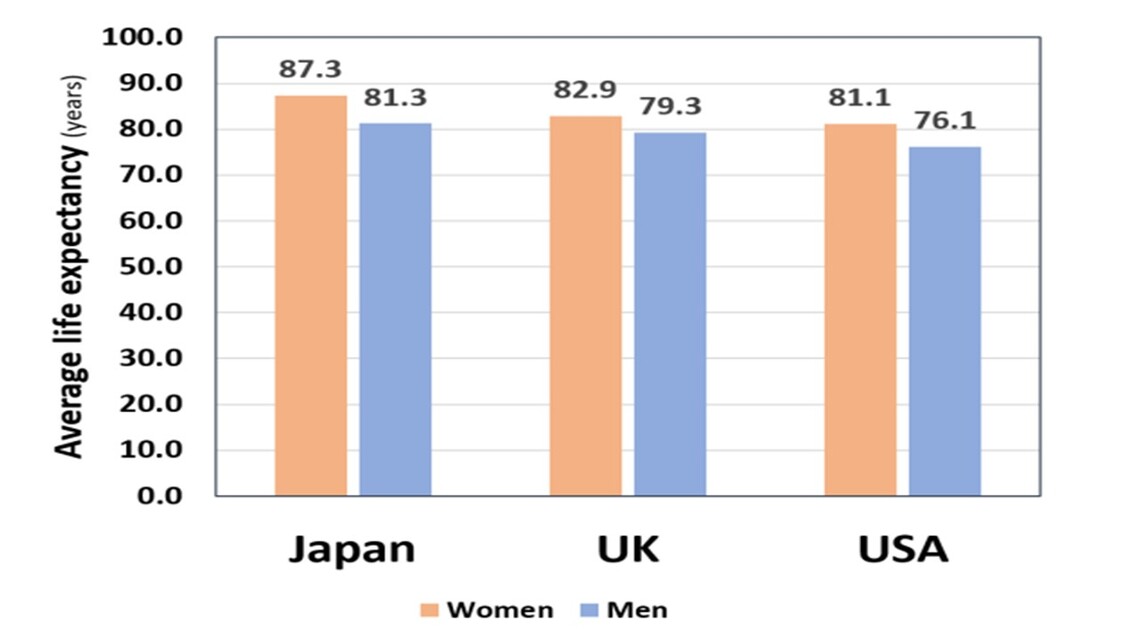
Japan consistently ranks among the countries with the highest life expectancy globally. Even as factors like diet and lifestyle are often cited, a novel study published in Geriatrics & Gerontology International suggests a crucial, and often overlooked, element: lower death rates within elder care facilities compared to other developed nations. This isn’t simply about living longer, but about experiencing better quality of life in later years, and the Japanese model of elder care may hold valuable lessons for aging populations worldwide.
The research, conducted by a team at the University of Tokyo, analyzed data from long-term care facilities in Japan, the United States, England, and Sweden. It found that Japanese facilities demonstrated significantly lower rates of mortality, even after accounting for the age and health status of residents. This finding challenges the assumption that simply investing more resources into elder care automatically translates to better outcomes. The key, researchers believe, lies in a holistic approach that prioritizes preventative care, social engagement, and a uniquely Japanese cultural emphasis on respect for the elderly.
A Different Approach to Elder Care
Traditional Western models of elder care often focus on medical intervention and managing chronic conditions. While essential, this approach can sometimes lead to a more clinical and less person-centered environment. In contrast, Japanese long-term care emphasizes maintaining independence and dignity for as long as possible. This is reflected in the design of facilities, which often incorporate communal spaces for social activities, and a staffing model that prioritizes consistent caregiver-resident relationships. According to the study, the Japanese system places a strong emphasis on “rehabilitation” – not necessarily restoring full physical function, but maximizing remaining abilities and promoting active participation in daily life.
A core component of this philosophy is the concept of kaigo, which translates roughly to “care” but encompasses a broader sense of nurturing and support. Kaigo workers aren’t simply tasked with administering medication or providing physical assistance; they are expected to build genuine connections with residents, understand their individual histories and preferences, and create a stimulating and supportive environment. This is supported by a national certification system for kaigo workers, requiring extensive training in both practical skills and compassionate care. The Ministry of Health, Labour and Welfare oversees this system, ensuring a baseline level of quality across facilities. More information about the ministry and its initiatives can be found on its website.
The Role of Social Connection and Diet
Beyond the structure of care facilities, broader cultural factors also contribute to Japan’s success in supporting healthy aging. Strong family ties and a deeply ingrained respect for elders are prevalent throughout Japanese society. While multigenerational households are becoming less common, regular visits and active involvement of family members in the care of their loved ones remain the norm. This social support network provides emotional comfort and reduces feelings of isolation, which are known risk factors for declining health in older adults.
Diet also plays a significant role. The traditional Japanese diet, rich in fish, vegetables, and fermented foods, is associated with numerous health benefits, including reduced risk of cardiovascular disease and certain types of cancer. These dietary habits, maintained throughout life, contribute to a healthier baseline for older adults entering long-term care. Research consistently demonstrates the link between the Mediterranean diet and longevity, and the Japanese diet shares many similar principles, emphasizing whole, unprocessed foods. The National Institutes of Health provides further information on the health benefits of traditional Japanese cuisine.
Implications for Global Aging Populations
As countries around the world grapple with rapidly aging populations, the Japanese experience offers valuable insights. The United States, for example, faces significant challenges in providing affordable and high-quality elder care. Costs are rising, staffing shortages are common, and many facilities struggle to provide the level of personalized attention that residents need. England and Sweden, while having well-developed welfare systems, also face similar pressures. The study suggests that simply increasing funding isn’t enough; a fundamental shift in philosophy is required.
This isn’t to say that the Japanese model is without its challenges. Japan’s aging population is among the most rapidly aging in the world, placing a strain on its social security system and healthcare infrastructure. The kaigo workforce is also facing its own demographic challenges, with an aging workforce and difficulty attracting younger workers. However, the lower mortality rates observed in Japanese elder care facilities demonstrate that a different approach is possible – one that prioritizes preventative care, social engagement, and a deep respect for the dignity of older adults.
Researchers emphasize that replicating the Japanese model wholesale may not be feasible or desirable in other cultural contexts. However, the underlying principles – person-centered care, strong social support networks, and a focus on maintaining independence – are universally applicable. Further research is needed to identify the specific elements of the Japanese system that are most effective and to adapt them to different settings. The University of Tokyo team plans to continue its research, focusing on the long-term impact of different care models on the quality of life of older adults.
The next phase of the study will involve a comparative analysis of caregiver burnout rates across the four countries, aiming to identify factors that contribute to a more sustainable and fulfilling work environment for those providing elder care. This information will be crucial for developing policies that attract and retain qualified caregivers, ensuring that older adults receive the compassionate and attentive care they deserve.
What lessons can other nations learn from Japan’s success in supporting healthy aging? Share your thoughts in the comments below, and please share this article with anyone interested in the future of elder care.