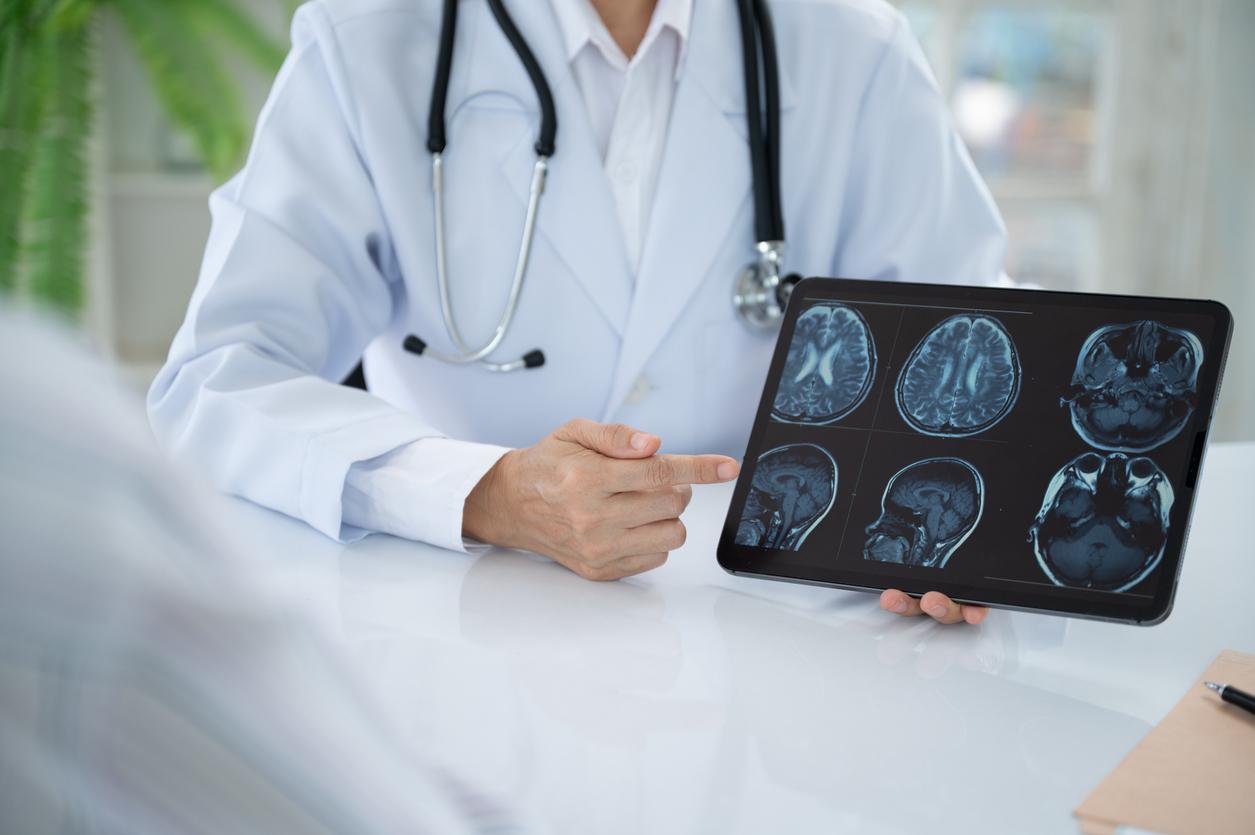
For parents and pediatricians, a diagnosis of childhood epilepsy often brings a primary focus to seizure management and safety. However, new research suggests that the neurological landscape for these children is often more complex than a single diagnosis. A significant correlation exists between epilepsy and autism spectrum disorder (ASD), meaning children managing seizures are substantially more likely to also navigate the challenges of autism.
The findings, published in the journal Developmental Medicine & Child Neurology, stem from an extensive study conducted by researchers at the Mayo Clinic. By analyzing a massive cohort of more than 30,000 children, the team sought to quantify the overlap between these two conditions and identify the risk factors that often go unnoticed during early clinical visits. The results serve as a critical reminder that neurological conditions rarely exist in a vacuum.
As a physician, I have seen how “diagnostic overshadowing” can occur in clinical practice—where the presence of a prominent condition, like epilepsy, inadvertently masks the symptoms of another, such as ASD. When a child is experiencing seizures, the immediate medical priority is stabilization and medication. Yet, this study underscores that the underlying brain circuitry affected by epilepsy may be the same circuitry involved in the development of autism, making proactive screening a clinical necessity rather than an option.
Quantifying the Correlation: The Mayo Clinic Findings
The study’s strength lies in its scale and its nuanced approach to diagnosis. The researchers didn’t rely on a single definition of autism; instead, they applied three different levels of clinical criteria to see how the prevalence shifted. Across every metric, children with epilepsy showed a markedly higher likelihood of having ASD than their non-epileptic peers.
The disparity was most pronounced when using broad research criteria, where the prevalence jumped from 3.2% in the general pediatric population to 21.4% in children with epilepsy. Even under the strictest clinical diagnostic standards, the risk remained significantly elevated, with 7.9% of children with epilepsy meeting the criteria compared to just 0.7% of those without the condition.
| Diagnostic Criteria | Non-Epileptic Children | Children with Epilepsy |
|---|---|---|
| Broad Research Criteria | 3.2% | 21.4% |
| Strict Research Criteria | 1.6% | 14.0% |
| Clinical Diagnosis | 0.7% | 7.9% |
The Overlap of Intellectual Disability and Gender
Beyond the primary link between epilepsy and ASD, the Mayo Clinic researchers identified a troubling synergy with intellectual disabilities. The data revealed that children presenting with both epilepsy and autism were far more likely to struggle with intellectual impairments. Specifically, 56.5% of the comorbid group faced intellectual disabilities, compared to only 15.4% of those who had epilepsy but not ASD.

One of the more surprising findings involves gender distribution. While autism is traditionally diagnosed more frequently in boys, this study observed a higher prevalence of girls within the group of children suffering from both epilepsy and ASD (38.2% compared to 25.8% in the non-autistic group). This suggests that the intersection of these two pathologies may manifest differently across genders or that girls with epilepsy may be more susceptible to the developmental disruptions that lead to ASD.
The World Health Organization (WHO) defines epilepsy as a chronic brain disorder characterized by recurrent seizures resulting from excessive electrical discharges in groups of brain cells. When these electrical disturbances occur during critical windows of brain development, they can potentially disrupt the formation of neural pathways responsible for social communication and sensory processing—the hallmarks of autism.
Closing the Diagnostic Gap: The 18-Month Window
The ultimate goal of this research is to shorten the time between the first signs of developmental delay and a formal diagnosis. Current medical guidelines suggest that ASD can be screened as early as 18 months of age. However, in practice, the road to a diagnosis often takes years, particularly for children whose medical history is dominated by the urgency of seizure control.
Elaine C. Wirrell, a co-author of the study, emphasizes that detecting autism in children with epilepsy is often more difficult, despite their higher risk. The symptoms of ASD—such as social withdrawal or repetitive behaviors—can sometimes be misinterpreted as side effects of anti-epileptic drugs or as a result of the cognitive fatigue that follows a seizure.
To improve long-term outcomes, the study advocates for a standardized screening protocol for all children diagnosed with epilepsy. Early intervention—including speech therapy, occupational therapy, and behavioral support—is most effective when implemented in the toddler years, as the brain remains highly plastic during this period.

For families, this means advocating for a holistic developmental assessment. If a child is being seen by a pediatric neurologist for epilepsy, it is reasonable to ask: “Given the known link between these conditions, should we be performing a formal autism screen now?”
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The medical community is now looking toward more granular genetic research to determine if a specific set of biomarkers predisposes certain children to both epilepsy and ASD. As personalized medicine advances, the next milestone will be the integration of genetic screening into the initial diagnostic workup for pediatric epilepsy to predict and preempt developmental delays.
Do you have experience navigating multiple diagnoses for your child? Share your story in the comments or share this article to help other parents advocate for early screening.