In the sterile corridors of modern healthcare, the most dangerous threats are often the ones that cannot be seen. For decades, hospitals and long-term care facilities have fought a grueling battle against Clostridioides difficile, a bacterium that turns a routine hospital stay into a life-threatening ordeal. While medical teams focus on treating the patient, a secondary, invisible war is waged on the bedrails, call buttons, and flooring where resilient spores linger long after a room appears clean.
The fundamental challenge in eradicating this pathogen is a simple matter of visibility. Traditional cleaning protocols rely on checklists and visual inspections, but detecting C. Diff spores on surfaces is impossible with the naked eye. This gap in oversight often leads to “re-contamination,” where a freshly cleaned room is inadvertently re-seeded with spores, perpetuating a cycle of healthcare-associated infections (HAIs).
To address this systemic vulnerability, the LIV Process has introduced a patented, water-based solution designed to make the invisible visible. By allowing staff to see live C. Diff spores on surfaces in approximately two minutes, the technology shifts the paradigm of environmental hygiene from an educated guess to a verified science.
The Persistence of the Spore
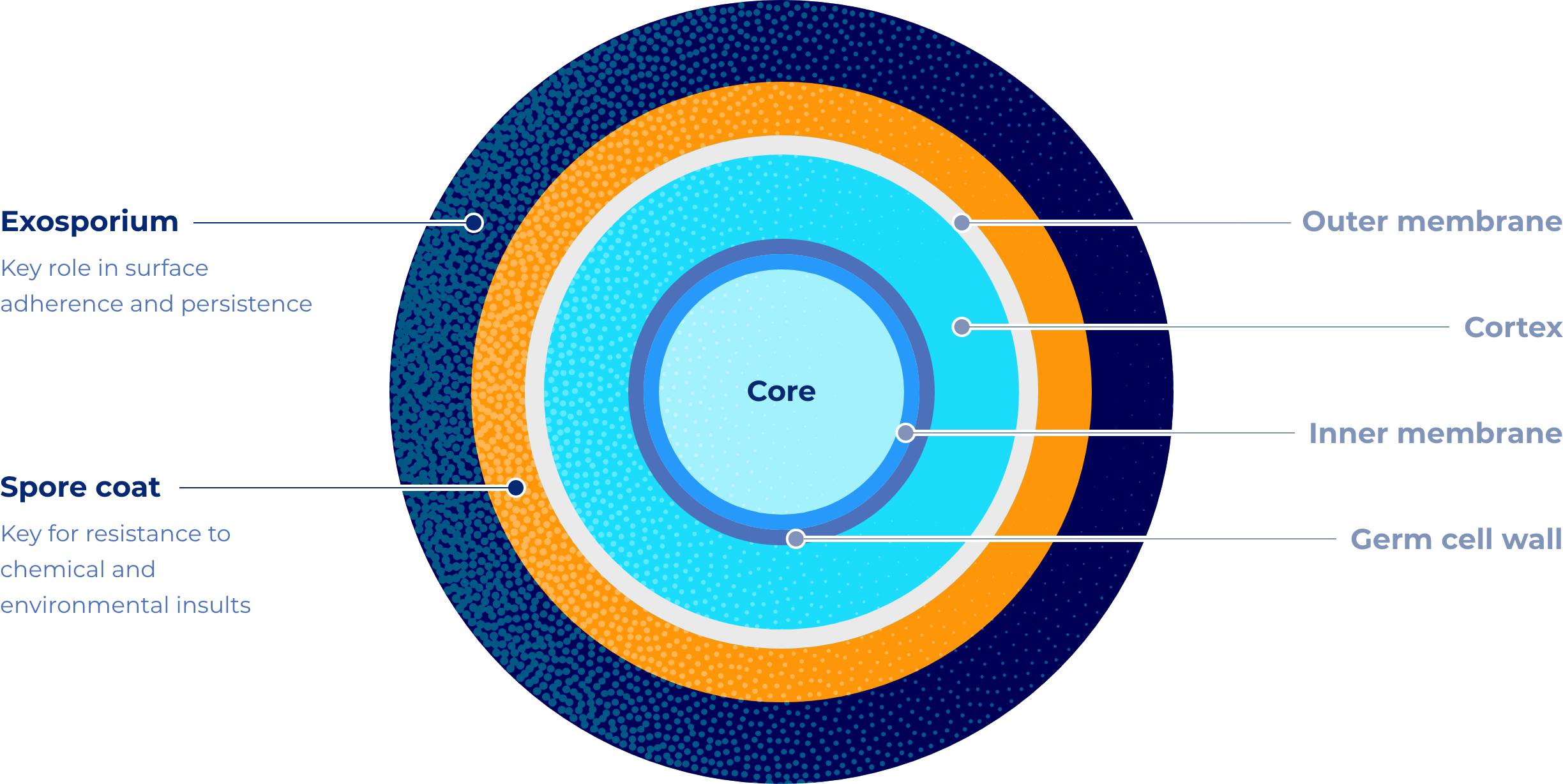
To understand why a visualization tool is necessary, one must understand the biology of C. Difficile. Unlike many bacteria that are easily neutralized by standard alcohol-based sanitizers, C. Diff produces spores—dormant, hardy structures that act as biological armor. These spores can survive for months on dry surfaces, resisting many common disinfectants.
According to the Centers for Disease Control and Prevention (CDC), C. Diff is a leading cause of healthcare-associated diarrhea and can lead to severe colitis or systemic inflammation. Given that the spores are microscopic and colorless, cleaning crews may believe a surface is sterile when it remains heavily contaminated. This “invisible” presence means that the very environment meant to heal the patient can instead become the vector for their next infection.
For clinicians, the frustration lies in the limitation of current audit tools. Many facilities use ATP (adenosine triphosphate) testing or fluorescent markers to check for cleanliness. But, ATP tests measure general organic matter—not specific pathogens—and fluorescent markers only show where a cleaner did wipe, not where a live spore actually remains.
Bridging the Gap with LIV Process
The LIV Process operates on a different premise: if you can see the problem, you can solve it. The patented water-based solution interacts with the live spores, triggering a visible reaction that alerts staff to the presence of the pathogen in real-time. The speed of the reaction—roughly two minutes—allows for immediate corrective action during the terminal cleaning process.
This immediacy transforms the role of the environmental services (EVS) team. Rather than following a static checklist, staff can target specific “hot spots” that are failing to clear. This targeted approach reduces the waste of chemicals and labor while increasing the actual safety of the patient environment.
In long-term care facilities, where patients are often immunocompromised and reside in the same space for extended periods, the stakes are even higher. The ability to verify the absence of spores before a recent resident is admitted to a room can significantly lower the rate of facility-wide outbreaks.
Comparison of Surface Verification Methods
| Method | What it Detects | Time to Result | Specific to C. Diff? |
|---|---|---|---|
| Visual Inspection | Visible dirt/debris | Instant | No |
| ATP Testing | General organic matter | Seconds/Minutes | No |
| Fluorescent Markers | Cleaning coverage/wipe | Instant (UV light) | No |
| LIV Process | Live C. Diff spores | ~2 Minutes | Yes |
The Impact on Patient Safety and Policy
The integration of rapid spore visualization into hospital workflows has implications that extend beyond a single room. When a facility can prove its surfaces are free of C. Diff, it reduces the reliance on restrictive contact precautions that can lead to patient isolation and psychological distress.
the financial burden of HAIs is staggering. Hospitals face significant penalties and increased costs associated with treating C. Diff infections, which often prolong hospital stays by several days. By implementing a system that ensures detecting C. Diff spores on surfaces is a standard part of the discharge process, facilities can mitigate these risks.
From a public health perspective, the LIV Process represents a shift toward “evidence-based cleaning.” This approach mirrors the way physicians treat patients—using diagnostic tools to confirm a condition before applying a treatment—rather than applying a blanket solution and hoping for the best.
Challenges and Constraints
While visualization technology provides a critical advantage, it is not a replacement for comprehensive infection control. The efficacy of the LIV Process still depends on the quality of the subsequent disinfection. Once spores are visualized, the facility must use an EPA-registered sporicidal agent, such as bleach or specialized hydrogen peroxide vapors, to eliminate them.
The primary constraint for many facilities remains the adoption curve. Moving from traditional cleaning to a verification-based model requires training and a shift in organizational culture. However, as regulatory bodies increase their scrutiny of HAI rates, the pressure to adopt verifiable cleaning standards is likely to grow.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a certified infection control professional or healthcare provider for clinical protocols regarding C. Diff management.
The next phase for environmental hygiene will likely involve the integration of these rapid detection tools with automated reporting systems, allowing hospital administrators to track “cleanliness trends” across different wards in real-time. As more data emerges on the reduction of infection rates linked to spore visualization, the industry may see a move toward mandated verification for high-risk units.
Do you think rapid visualization tools should be mandatory in all long-term care facilities? Share your thoughts in the comments or share this article with your healthcare network.

