For millions of adults, the sensation of a dull ache or a sharp, stabbing pain in the lower back is more than a temporary inconvenience. it is a defining feature of their daily existence. Once viewed primarily as a condition of the elderly or those in labor-intensive trades, chronic back pain has evolved into a widespread public health challenge affecting people of all ages, and professions.
The modern landscape of work—characterized by prolonged sitting, static postures, and a general decline in daily physical activity—has created a perfect storm for musculoskeletal dysfunction. As a physician, I have seen the shift in patient demographics firsthand; the “desk-bound” injury is now as common as the “heavy-lift” strain. Understanding chronic back pain treatment options requires a shift in perspective, moving away from the outdated notion of bed rest toward a model of active recovery and systemic wellness.
Current clinical data underscores the scale of the issue. Low back pain remains the leading cause of disability worldwide, contributing significantly to years lived with disability across various socioeconomic groups, according to research published in The Lancet. The complexity of the condition lies in its etiology; pain is rarely the result of a single event but is often the culmination of degenerative changes, lifestyle habits, and psychological stressors.
The Mechanics of Chronic Back Pain
To treat back pain effectively, one must first understand what is happening beneath the skin. The human spine is a complex architecture of vertebrae, discs, ligaments, and muscles. When this system fails, the pain is typically categorized as either mechanical or non-mechanical.
Mechanical pain is the most common form, resulting from the physical movement of spinal structures. This includes degenerative disc disease, where the cushions between vertebrae wear down, or herniated discs that press against adjacent nerves. Spinal stenosis—the narrowing of the spaces within the spine—can also lead to pressure on the spinal cord, often manifesting as pain that radiates down the legs, a condition known as sciatica.
However, the “everyone’s problem” aspect of modern back pain often stems from muscular imbalances. Prolonged sitting leads to shortened hip flexors and weakened gluteal and core muscles. This imbalance forces the lumbar spine to grab on loads it was not designed to support, leading to chronic strain and inflammation of the soft tissues.
A Tiered Approach to Treatment
The gold standard for managing back pain has shifted toward a conservative-first approach. The goal is to avoid invasive procedures unless absolutely necessary, focusing instead on restoring function and reducing the nervous system’s sensitivity to pain.
Non-Pharmacological Interventions
The first line of defense is almost always physical therapy. Rather than generic exercise, targeted rehabilitation focuses on core stability and proprioception. Techniques such as the McKenzie Method help patients identify specific movements that “centralize” pain, moving it from the extremities back toward the spine where it is more manageable.
Low-impact aerobic activity, such as swimming or walking, is equally critical. Movement increases blood flow to the spinal structures, facilitating the delivery of nutrients to discs that lack their own direct blood supply. Cognitive Behavioral Therapy (CBT) is also increasingly integrated into treatment plans to address the psychological component of chronic pain, helping patients break the cycle of fear-avoidance—where the fear of pain leads to inactivity, which in turn leads to more stiffness and pain.
Medical and Interventional Options
When conservative measures are insufficient, medical interventions are introduced. This typically begins with non-steroidal anti-inflammatory drugs (NSAIDs) to manage acute flare-ups. However, the medical community has moved aggressively away from long-term opioid use due to the risk of dependency and the lack of evidence that they improve long-term functional outcomes.
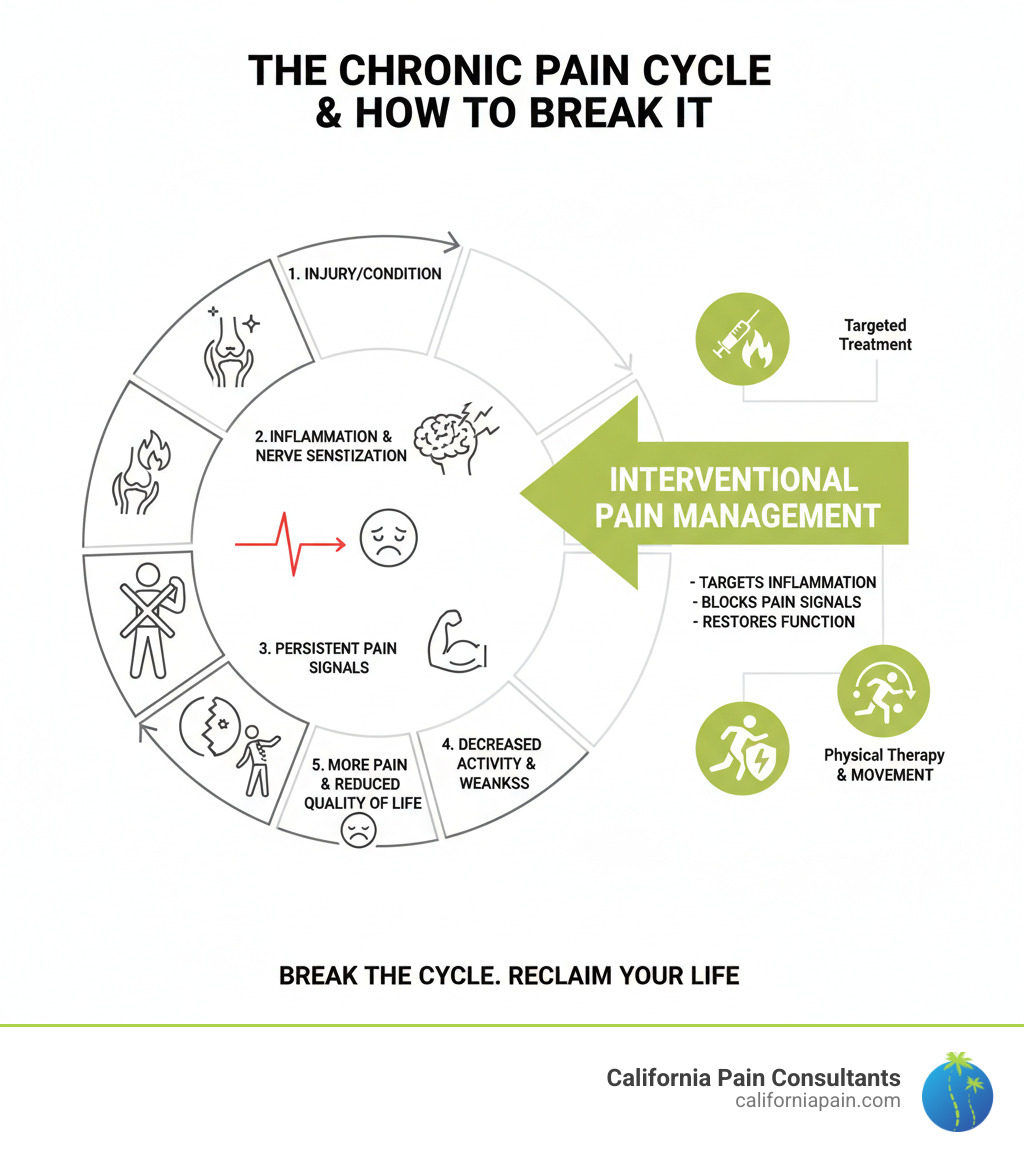
For targeted relief, physicians may utilize epidural steroid injections or nerve blocks. These are not “cures” but are intended to reduce inflammation enough to allow the patient to engage more effectively in physical therapy. Surgery, such as a laminectomy or spinal fusion, is reserved for specific indications: severe neurological deficits, cauda equina syndrome, or failure of all other modalities over a prolonged period.
| Treatment Tier | Primary Goal | Common Modalities | Typical Indication |
|---|---|---|---|
| Conservative | Functional Restoration | Physical Therapy, Yoga, CBT | Mild to Moderate Chronic Pain |
| Pharmacological | Symptom Management | NSAIDs, Muscle Relaxants | Acute Flare-ups, Inflammation |
| Interventional | Localized Inflammation Reduction | Epidural Injections, Nerve Blocks | Radiculopathy, Failed Conservative Care |
| Surgical | Structural Decompression | Discectomy, Spinal Fusion | Severe Nerve Compression, Instability |
Preventing the Cycle of Recurrence
Treating the current episode of pain is only half the battle; preventing recurrence requires a fundamental change in how we interact with our environment. The concept of “ergonomics” is often dismissed as a luxury, but it is a medical necessity for those spending eight or more hours a day at a desk.
Key adjustments include ensuring the monitor is at eye level to prevent cervical strain and utilizing chairs that support the natural inward curve of the lower back. More importantly, the “best posture is the next posture.” Static positions, even “correct” ones, lead to tissue ischemia. Integrating “movement snacks”—two-minute stretches or walks every hour—is more effective than a single hour of exercise at the end of the day.
Building core strength is not about achieving a six-pack; it is about creating a biological corset. Strengthening the transverse abdominis and multifidus muscles provides the internal stability necessary to protect the lumbar spine during everyday movements, such as bending or lifting.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Looking forward, the field of spinal health is moving toward personalized medicine. Researchers are currently exploring the use of genetic markers to predict who is most susceptible to chronic pain and utilizing AI-driven wearable sensors to provide real-time ergonomic feedback to workers. The next major milestone in public health will likely be the integration of these preventative technologies into standard workplace wellness programs to stem the tide of spinal disability.
Do you have a strategy that helped you manage chronic back pain? Share your experience in the comments or share this guide with someone navigating their own recovery.