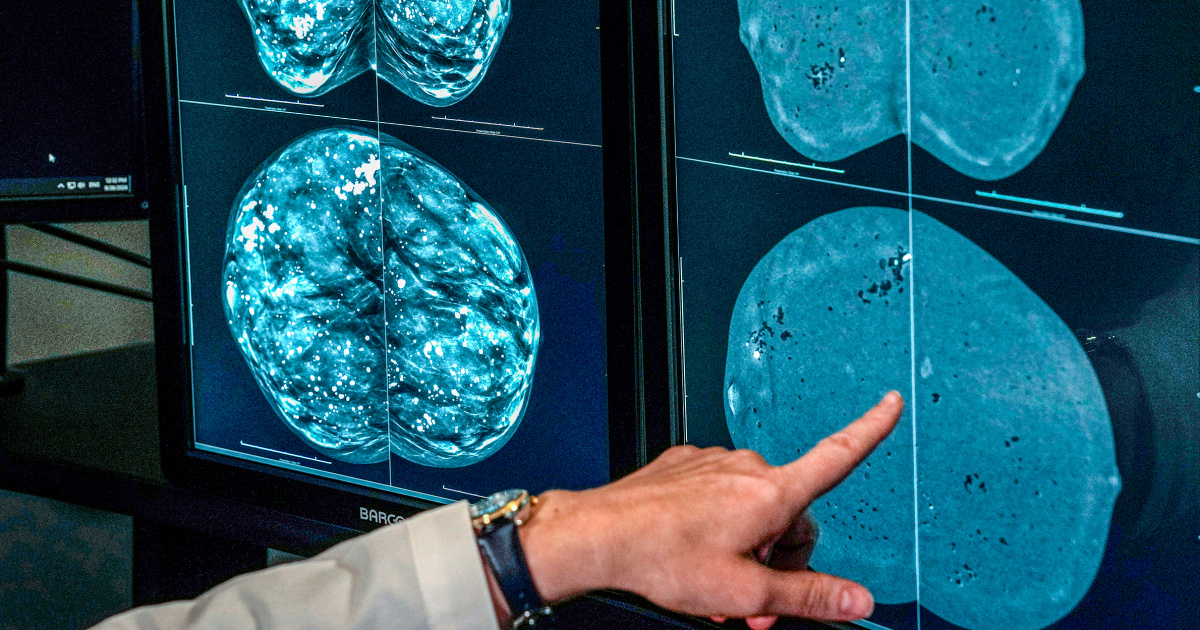
For many women, the annual wellness visit often brings a familiar, frustrating question: When exactly should I start getting mammograms?
Depending on which health organization’s website you visit, the answer varies. Some suggest starting at age 40, others at 45, and some at 50. The disagreement doesn’t end with the starting line; experts also clash over whether the scans should happen every year or every other year. This lack of consensus can leave patients feeling anxious, wondering if they are screening too late or submitting themselves to unnecessary procedures.
As a physician, I see this confusion daily. The tension exists because breast cancer screening is a balancing act. On one side is the goal of early detection, which saves lives. On the other is the risk of “overdiagnosis”—finding small, slow-growing tumors that might never have caused harm, leading to unnecessary biopsies, radiation, and psychological stress. Because guidelines are designed for women at “average risk,” they often fail to account for the biological diversity of individual patients.
Understanding when should you get a mammogram requires looking past the broad numbers and understanding the risk factors that make your health profile unique.
The Great Divide: Comparing Current Guidelines
The discrepancy in advice stems from how different medical bodies weigh the benefits of early detection against the potential harms of false positives. The U.S. Preventive Services Task Force (USPSTF), one of the most influential bodies in primary care, recently updated its guidance to recommend that women begin biennial (every other year) screening at age 40. This was a shift from previous advice that suggested starting at 50.
Other organizations maintain different thresholds. The American Cancer Society (ACS) has long advocated for a more aggressive approach for women in their late 40s, while the American College of Physicians (ACP) suggests a more conservative timeline for those under 50.
| Organization | Recommended Start Age | Frequency | Notes |
|---|---|---|---|
| USPSTF | 40 | Every 2 years | Updated in 2024 to lower start age. |
| American Cancer Society | 45 (optional at 40) | Yearly (45-54) | Suggests biennial after age 55. |
| American College of Physicians | 50 | Every 2 years | Ages 40-49 should discuss pros/cons with a doctor. |
The American Cancer Society’s preference for yearly scans between ages 45 and 54 is rooted in data showing that breast cancer incidence in the 45-to-49 age group is significantly higher than in the early 40s, mirroring the risk seen in women aged 50 to 54.
Why Experts Disagree on the Timing
The central conflict is that breast cancer is not a single disease, but a collection of different subtypes with varying growth rates. Dr. Laura Esserman of the University of California, San Francisco, notes that screening everyone the same way is logically flawed because not everyone shares the same risk.

For a woman with high genetic risk, screening every year (or even more frequently) is a lifesaver. For a woman at very low risk, screening every year may increase the likelihood of a “false positive”—a suspicious finding that leads to a stressful biopsy only to reveal a benign cyst. Dr. Carolyn Crandall of the University of California, Los Angeles, who chaired the ACP report, explains that for women in their 40s, there is a “narrower balance” between the potential benefits and the harms of screening.
Beyond the common BRCA1 and BRCA2 gene mutations, it is often tough for patients to know their true risk level. Until now, age has served as the primary proxy for risk, as the likelihood of developing breast cancer increases as a woman grows older.
The Complexity of Breast Density
Another variable that complicates the “one size fits all” approach is breast density. Nearly half of women over 40 have dense breast tissue, meaning they have more glandular and fibrous tissue than fatty tissue.
On a mammogram, both dense tissue and tumors appear white, creating a “masking effect” that can make it harder for radiologists to spot a malignancy. High breast density is itself a slight risk factor for developing cancer. While the use of supplemental screening—such as ultrasound or MRI—for women with dense breasts is still debated, the ACP suggests considering 3D mammography, known as digital breast tomosynthesis (DBT), which provides a more layered, detailed view of the tissue.
The Shift Toward Precision Screening
The future of breast cancer detection is moving away from age-based milestones and toward risk-based precision. The goal is to identify who needs aggressive surveillance and who can safely space out their appointments.
A significant step in this direction is the WISDOM trial, a study of nearly 46,000 women led by Dr. Esserman. By combining genetic testing, lifestyle data, health history, and breast density, researchers classified women into low, average, elevated, or high-risk categories. Those in the highest risk group were screened twice a year with both mammography and MRI. The findings, published in JAMA, indicated that this risk-based approach worked as well as standard yearly screening for the general population.
One surprising revelation from the trial was that roughly 30% of women with a genetically increased risk had no family history of breast cancer, highlighting the danger of relying solely on family trees to determine when to start screening.
Looking ahead, AI tools are being developed to analyze subtle patterns in existing mammograms to predict a woman’s risk of developing cancer in the subsequent few years. This could allow doctors to dynamically adjust a patient’s screening interval based on the “clues” left in their imaging.
Practical Steps for Patients
Until risk-based screening becomes the standard of care, the best approach is a shared decision-making process between a patient and their provider. When discussing when should you get a mammogram with your doctor, be prepared to discuss:

- Detailed family history, including relatives who had cancer at a young age.
- Your overall health history and reproductive milestones, such as the age at which you had children.
- Your breast density, if you have had a previous scan.
- Your personal tolerance for the anxiety associated with potential false positives.
the most critical factor is consistency. As Robert Smith, a public health researcher and expert on early detection for the American Cancer Society, emphasizes, breast screening is most effective when it is performed regularly, regardless of the specific interval chosen.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Medical researchers continue to refine these guidelines as more data from the WISDOM trial and AI-driven studies become available. The next major shift in guidance is expected as genomic risk scores become more integrated into primary care settings.
Do you find the current screening guidelines confusing? Share your experience in the comments or share this guide with a friend who is navigating their health options.