For millions of people living with chronic spontaneous urticaria (CSU), the condition is far more than a dermatological nuisance. It’s an exhausting cycle of relentless itching, swelling wheals, and profound sleep deprivation that can dismantle a person’s quality of life. While the first line of defense is typically H1-antihistamines, a significant portion of the patient population finds that even high-dosage regimens fail to provide adequate relief.
This therapeutic gap has led researchers to look beyond conventional pharmacology toward integrative strategies. Recent meta-analyses suggest that the integration of Traditional Chinese Medicine (TCM)—specifically acupuncture and targeted herbal protocols—may offer a viable path forward for those with therapy-resistant chronic Nesselsucht, focusing not just on suppressing symptoms but on modulating the underlying immune response.
The evidence suggests a shift in how clinicians approach the disease. By combining standard care with evidence-based TCM interventions, patients are seeing a marked reduction in both the severity of their flares and the frequency of relapses, offering a new level of stability for those who previously felt their condition was untreatable.
The Clinical Impact of Acupuncture on Relapse Rates
The efficacy of acupuncture in treating CSU has moved from anecdotal evidence to quantifiable data. An analysis of eight randomized controlled trials involving 564 participants indicates that acupuncture significantly improves clinical outcomes when compared to antihistamine therapy alone. The data highlights a relative risk of 1.19 in favor of the acupuncture groups, suggesting a superior overall response rate.
Perhaps more critical for long-term patient management is the impact on recurrence. The findings show a dramatic drop in relapse rates, with the risk of new flares falling to 0.25 compared to control groups. From a medical perspective, this suggests that acupuncture may do more than simply block histamine; it appears to exert a regulatory influence on the immune system, potentially stabilizing the mast cell activation that drives the disease.
Targeted Intervention: Ear Acupuncture and the ‘Wind-Heat’ Type
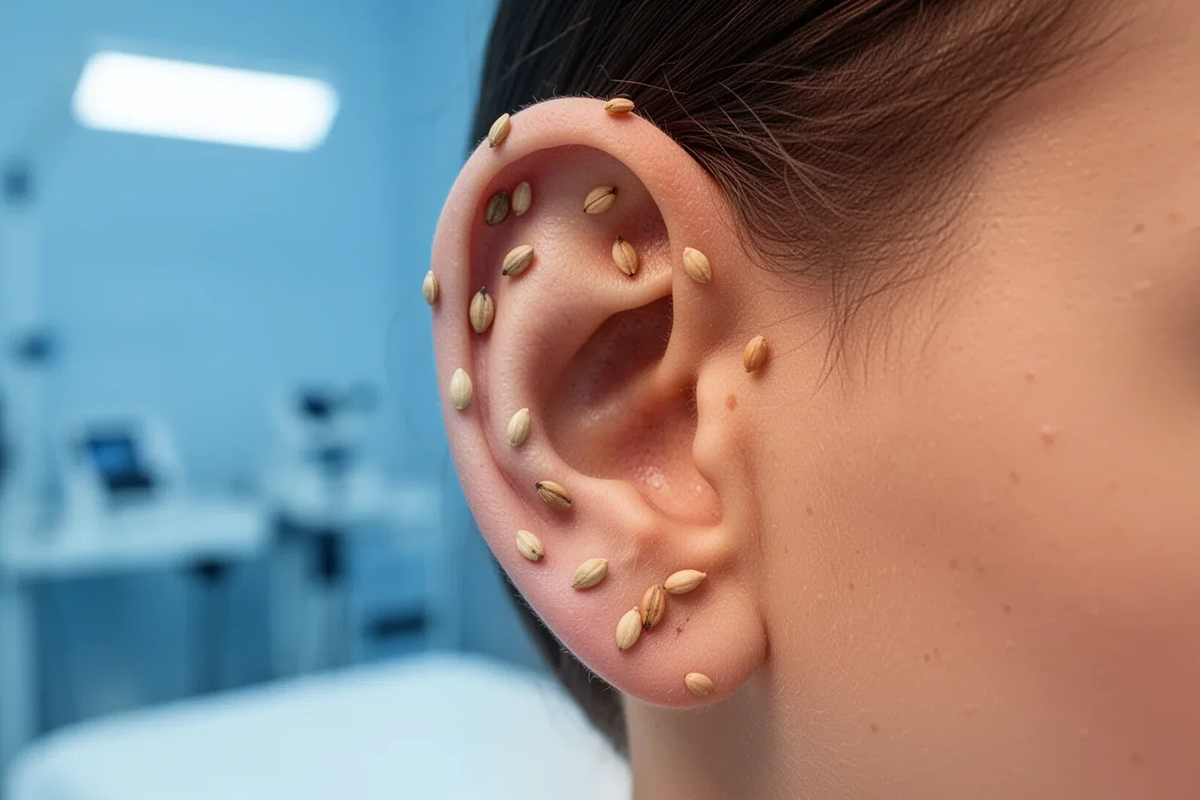
In the realm of integrative dermatology, precision is key. TCM practitioners often categorize urticaria into different “syndromes,” such as the “Wind-Heat” type. For these patients, a specialized form of acupressure using Vaccaria seeds—small, naturally occurring seeds used as tactile stimulants—is being utilized to target specific neurobiological pathways.
This approach involves placing seeds on five strategic points of the ear to modulate the body’s stress and inflammatory responses:
- Shenmen (TF4): Used to reduce anxiety and systemic inflammation.
- Sympathetic Point (AH6): Targeted to balance the autonomic nervous system.
- Endocrine Point (CO18): Aimed at hormonal regulation.
- Adrenal Point (TG2): Targeted to manage the body’s cortisol and stress response.
- Lung Point (CO14): Traditionally associated with skin health and respiratory balance.
Patients stimulate these points several times a day through light pressure, with the goal of reducing the Urticaria Activity Score (UAS7)—a standardized metric that tracks the daily number of wheals and the intensity of itching. Researchers believe this process inhibits the release of inflammatory mediators, providing a non-pharmacological method to dampen the allergic cascade.
Herbal Synergy and Therapy-Resistant Cases
For patients who do not respond to double doses of H1-antihistamines, systematic reviews have identified specific herbal formulations that may bridge the gap. Analysis of over 1,100 patients across 14 studies has pointed to a core group of botanical agents that consistently appear in successful treatment protocols.

Key ingredients include Saposhnikovia divaricata (Windbreaker), Glycyrrhiza uralensis (Licorice), and Angelica sinensis (Dong Quai). One particular formula, Guizhi Tang (Cinnamon Twig Decoction), has demonstrated a safety and efficacy profile that rivals some conventional medications in controlled settings, particularly in its ability to improve the Dermatology Life Quality Index (DLQI).
The benefit of these botanical interventions extends beyond the skin. Because chronic urticaria is frequently comorbid with anxiety and insomnia—affecting more than half of all CSU patients—the combination of internal herbal medicine and external therapies like “fire needle” therapy has been shown to significantly reduce psychological distress and improve sleep architecture.
The Shift Toward Integrative Dermatology
The movement toward an integrative approach is driven largely by the side-effect profiles of current gold-standard treatments. In certain regions, up to 54 percent of chronic urticaria patients are prescribed oral corticosteroids. While effective in the short term, the long-term risks of steroids—including osteoporosis, glucose intolerance, and adrenal suppression—are well-documented.
Integrating TCM offers a lower-risk alternative. Some meta-analyses indicate that the overall effectiveness of TCM interventions can be up to 23 percent higher than standard therapy alone, with significantly fewer adverse effects. For clinicians, this represents an opportunity to increase patient satisfaction and adherence by offering a toolkit that addresses both the physical and emotional toll of the disease.
| Intervention | Primary Mechanism | Key Clinical Goal |
|---|---|---|
| Acupuncture | Immune Modulation | Reduced Relapse Rates |
| Ear Seeds (Vaccaria) | Neurobiological Signaling | Lower UAS7 Score |
| Herbal Formulae | Systemic Anti-inflammatory | Improved DLQI / Sleep |
| Antihistamines | H1-Receptor Blockade | Symptom Suppression |
Despite these promising results, the medical community emphasizes the need for rigorous standardization. Because acupuncture techniques and herbal concentrations can vary widely between practitioners, the data remains heterogeneous. The next critical step for the field is the implementation of larger, double-blind, placebo-controlled trials to integrate these findings into international clinical guidelines and treatment algorithms.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As researchers move toward a deeper understanding of immunofailure and regulation, the focus is shifting from merely masking symptoms to correcting the underlying dysfunction. The coming months will likely see more data on the viability of ear acupuncture as a home-based “maintenance therapy” to prevent the onset of new flares.
We invite you to share your experiences with integrative dermatology in the comments below or share this article with others seeking alternative options for chronic skin conditions.