For women living with rheumatoid arthritis (RA), the journey toward motherhood often involves a complex balancing act between managing a chronic autoimmune disease and the biological demands of conception. New clinical evidence suggests that a more aggressive, personalized approach to disease management—known as “treat-to-target”—can significantly reduce the time it takes for these women to achieve pregnancy.
The findings, led by senior author Radboud Dolhain, MD, PhD, indicate that the treat-to-target (T2T) strategy is more effective than standard care in accelerating the path to conception. By prioritizing the achievement of low disease activity or complete remission before pregnancy, clinicians can potentially remove inflammatory barriers that hinder fertility.
This shift in approach moves away from a “one-size-fits-all” medication schedule and toward a rigorous, data-driven cycle of assessment and adjustment. According to Dr. Dolhain, the strength of these data is “definitely enough to change guidelines,” suggesting a fundamental pivot in how rheumatologists support women of childbearing age.
The Mechanics of Treat-to-Target
In traditional RA management, patients often follow a stable medication regimen with periodic check-ups. While effective for many, this approach may not be sensitive enough to the fluctuations of autoimmune activity that can impact reproductive health. Treat-to-target, by contrast, is a proactive management strategy that sets a specific clinical goal—usually remission or very low disease activity—and adjusts therapy frequently until that goal is met.
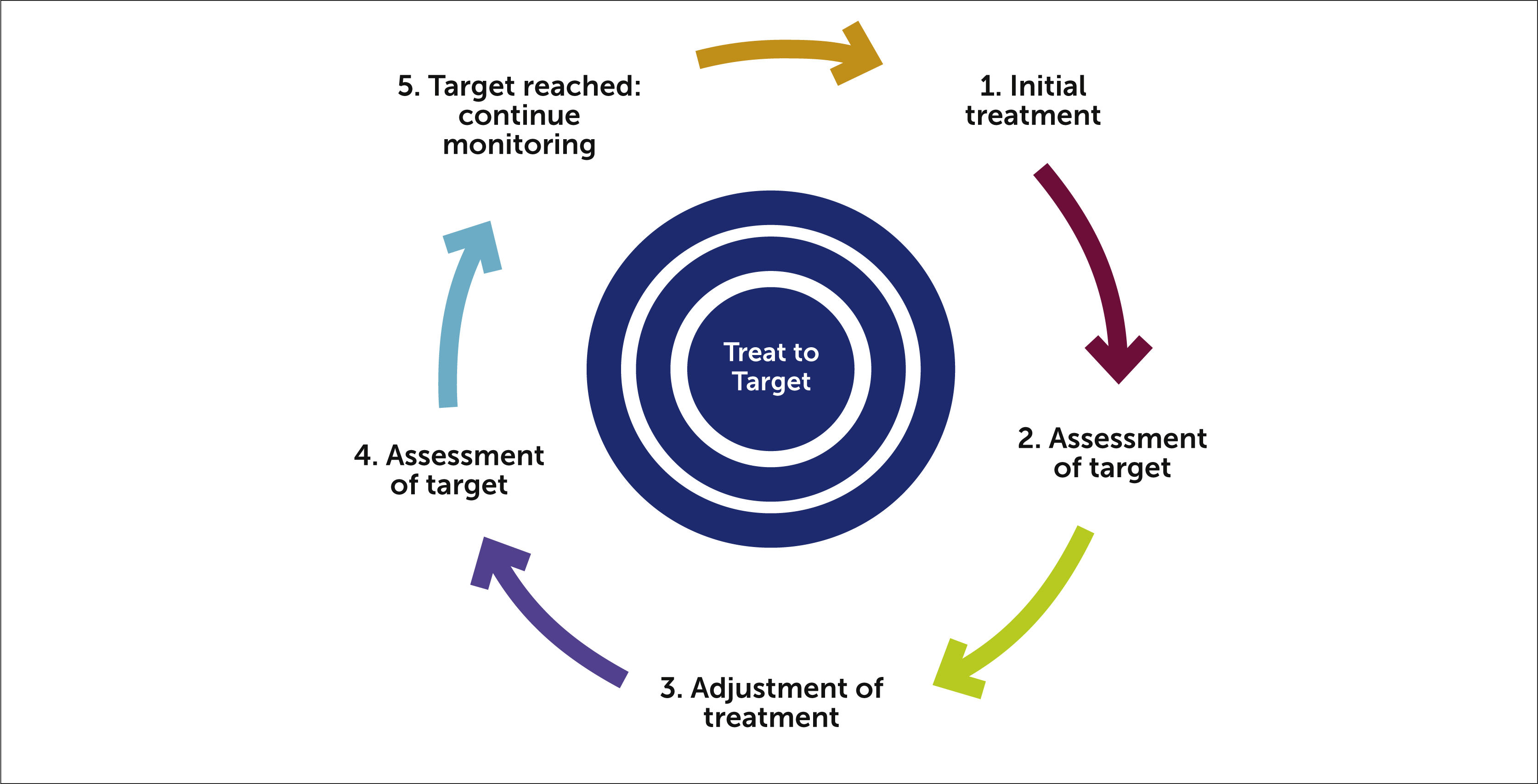
For women attempting to conceive, this means more frequent monitoring of inflammatory markers and joint swelling. If the “target” is not being hit, the physician quickly escalates or switches medications rather than waiting for the next scheduled quarterly visit. This ensures that the body is in the most stable biological state possible before the physical stress of pregnancy begins.
The physiological reasoning is grounded in the impact of systemic inflammation. High levels of disease activity in rheumatoid arthritis can disrupt ovulation and create a suboptimal uterine environment, making it more difficult for an egg to be fertilized or implanted. By aggressively suppressing this inflammation, T2T effectively clears the biological path for conception.
Comparing Management Strategies
The trial highlighted a clear divergence in outcomes between those receiving conventional care and those under the T2T protocol. While both groups received evidence-based medications, the frequency and intent of the interventions differed.

| Feature | Standard Care | Treat-to-Target (T2T) |
|---|---|---|
| Primary Goal | Symptom management | Remission or low disease activity |
| Monitoring | Periodic/Scheduled | Frequent and intensive |
| Medication Adjustments | Reactive (based on flares) | Proactive (based on target metrics) |
| Impact on TTP | Baseline conception rate | Shortened time to pregnancy |
Why This Matters for Reproductive Health
The “time to pregnancy” (TTP) is a critical metric in fertility. For women with RA, a prolonged TTP can lead to increased psychological distress and a higher likelihood of resorting to expensive or invasive assisted reproductive technologies. The discovery that a management shift alone can shorten this window provides a non-invasive way to improve fertility outcomes.
Beyond the act of conception, achieving remission via T2T is vital for the health of the pregnancy itself. Uncontrolled RA is associated with a higher risk of preterm birth and low birth weight. By ensuring the mother is in a state of low disease activity before the first trimester, the T2T approach potentially lowers these risks, creating a safer environment for both the parent and the developing fetus.
However, this strategy requires a delicate coordination between rheumatologists and obstetricians. Many RA medications, particularly certain disease-modifying antirheumatic drugs (DMARDs), must be tapered or switched before conception due to potential teratogenic risks. The T2T framework provides a structured timeline for these transitions, ensuring that the disease does not flare during the critical window when certain medications are withdrawn.
Challenges and Clinical Implementation
Despite the clear benefits, implementing a T2T strategy globally presents logistical challenges. It requires more clinic visits, more frequent blood operate and a higher level of coordination between healthcare providers. In overstretched health systems, the intensity of T2T can be difficult to sustain.
the psychological burden on the patient is a consideration. Constant monitoring and the pressure to reach a “target” can be stressful for women already dealing with the anxiety of infertility. Clinicians are encouraged to pair the T2T medical protocol with supportive mental health resources to ensure the process remains empowering rather than overwhelming.
The research suggests that the most successful outcomes occur when the patient is an active participant in the T2T process, tracking their own symptoms and communicating closely with their care team. This collaborative model transforms the patient from a passive recipient of care into a partner in their reproductive journey.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should consult with their healthcare provider or a board-certified rheumatologist before making changes to their medication or treatment plan.
The next step for the medical community involves the formal integration of these findings into international clinical guidelines. Experts expect that upcoming updates from organizations such as the European Alliance of Associations for Rheumatology (EULAR) and the American College of Rheumatology (ACR) will reflect the necessity of a treat-to-target approach for women planning a pregnancy.
We invite readers to share their experiences with RA management and pregnancy in the comments below or share this article with others who may find this research helpful.

