As the respiratory virus season settles into a predictable annual rhythm, a recurring anxiety persists: the emergence of new variants. From the constant mutations of SARS-CoV-2 to the shifting strains of seasonal influenza, the viral landscape is in a state of perpetual flux. Yet, recent immunological data suggests a critical distinction between a virus’s ability to cause an infection and its ability to cause a catastrophe.
While new immune defenses against flu and COVID variants are frequently challenged by viral mutations, the human body’s secondary lines of defense remain remarkably resilient. Even when a new variant successfully “evades” the first wave of antibodies to cause a mild illness, the broader immune system—specifically T-cells—continues to blunt the progression toward severe disease, hospitalization and death.
This phenomenon explains a paradoxical trend observed in public health data: we are seeing frequent “waves” of infection, yet the rate of critical illness has plummeted compared to the early stages of the pandemic. This shift is not merely a result of viral attenuation, but a testament to the depth of “hybrid immunity” acquired through a combination of vaccination and prior exposure.
The Viral Shell Game: How Variants Evade Detection
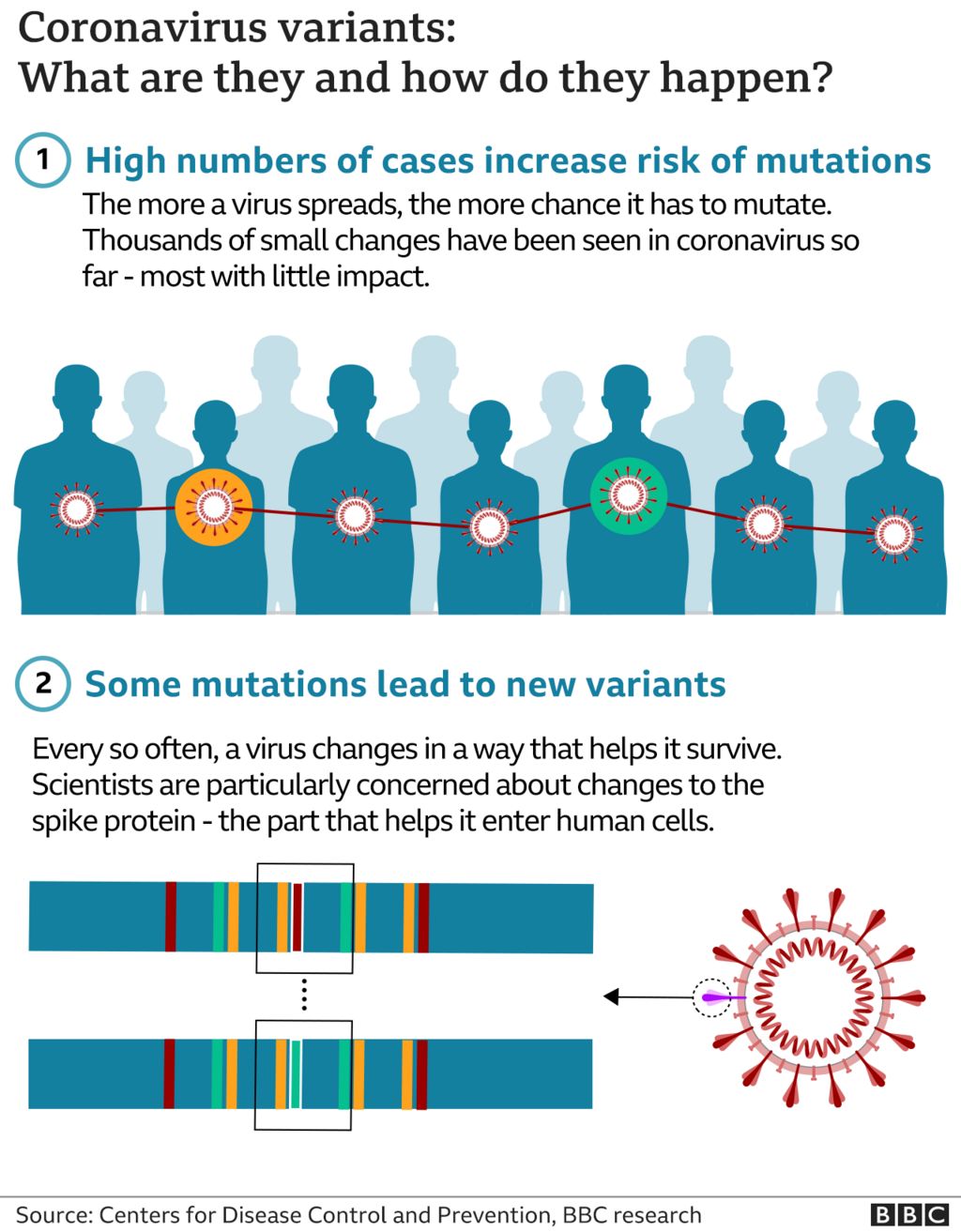
To understand why we still secure sick despite being vaccinated or previously infected, it is necessary to look at the “spike” of the virus. In the case of SARS-CoV-2, the spike protein is the key the virus uses to unlock and enter human cells. Antibodies, produced by B-cells, act like locks that snap onto these spikes, neutralizing the virus before it can enter a cell.
Viruses evolve through mutation, essentially changing the shape of that spike protein. When a variant like those in the Omicron lineage emerges, it often possesses mutations that make it “invisible” to the specific antibodies created by an older vaccine or a previous infection. This is known as immune evasion. When neutralizing antibodies cannot bind effectively, the virus gains a foothold, leading to the familiar symptoms of a cold or flu.
A similar process occurs with influenza. The flu virus undergoes “antigenic drift,” making compact changes to its surface proteins. This is why the CDC updates the annual flu vaccine to match the strains most likely to circulate each season.
T-Cells: The Body’s Internal Security Force
While antibodies are the first responders, T-cells are the specialized tactical units of the immune system. Unlike antibodies, which primarily target the exterior “shell” of the virus, T-cells recognize internal fragments of the virus that are presented on the surface of already-infected cells.
Crucially, these internal proteins are far more stable and less prone to mutation than the surface spikes. Even if a variant has completely redesigned its exterior to sneak past antibodies, its internal machinery remains largely the same. T-cells recognize these conserved regions and move in to destroy the infected cells, effectively halting the virus’s replication and preventing it from spreading deep into the lungs or other vital organs.
This is why the “blunting” effect occurs. You may feel the fever, fatigue, and congestion of an active infection because the antibodies failed to stop the initial entry, but the T-cells prevent the infection from escalating into pneumonia or systemic organ failure.
Comparing Immune Responses
| Feature | Neutralizing Antibodies (B-cells) | Cellular Immunity (T-cells) |
|---|---|---|
| Primary Goal | Prevent the virus from entering cells | Clear infected cells from the body |
| Target Area | Surface proteins (e.g., Spike protein) | Conserved internal viral proteins |
| Variant Sensitivity | High (easily evaded by mutations) | Low (remains effective across variants) |
| Clinical Outcome | Prevents mild/moderate infection | Prevents severe disease and death |
The Power of Hybrid Immunity
The current state of public health is heavily influenced by hybrid immunity—the synergistic effect of vaccination and natural infection. Research indicates that individuals with hybrid immunity often possess a more diverse “library” of antibodies and a more robust T-cell response than those who have only had one or the other.
This diversity acts as a safety net. By exposing the immune system to multiple versions of the virus, the body learns to recognize a wider array of viral patterns. This makes it significantly harder for any single mutation to completely bypass the immune system. While a new variant might bypass 60% of your antibodies, the remaining 40%, combined with a powerful T-cell response, is often enough to maintain the illness manageable.
This resilience is a primary reason why the World Health Organization and other health bodies continue to emphasize boosters. Boosters do not just “top up” antibody levels; they support refine the immune system’s ability to recognize emerging variants.
What This Means for Daily Health
For the average person, this scientific reality shifts the goalpost of “success” regarding respiratory viruses. In the early days of 2020, the goal was zero infection. Today, the clinical focus has shifted toward the prevention of severe outcomes.
It is important to recognize that “blunting severe disease” does not mean the virus is harmless. For high-risk populations—including the elderly, the immunocompromised, and those with chronic respiratory conditions—the gap between a “mild” case and a “severe” case is much narrower. For these individuals, the evasion of antibodies can still lead to dangerous complications if their T-cell response is sluggish or weakened.
Practical steps to maintain these defenses include:
- Staying current with vaccinations: Updated shots provide the most recent “blueprints” for antibodies to recognize new variants.
- Supporting general immune health: Adequate sleep, nutrition, and stress management support the production and function of T-cells.
- Strategic masking: In high-risk settings, reducing the initial viral load can make it easier for the immune system to manage the infection.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Looking ahead, health agencies are monitoring the genomic sequencing of current circulating strains to determine if the upcoming seasonal boosters will require further adjustments. The next major checkpoint will be the release of the seasonal vaccine compositions for the next cycle, which will be based on the variants currently dominating the Southern Hemisphere.
Do you have questions about the latest variants or how to protect your family this season? Share this article and join the conversation in the comments below.