A sudden surge of Ebola virus disease has claimed at least 65 lives in the eastern region of the Democratic Republic of Congo (DRC), sparking an urgent mobilization of international health resources. The outbreak, centered in areas already destabilized by chronic conflict, presents a complex challenge for medical teams attempting to contain a highly lethal pathogen in a landscape of deep mistrust and fragmented infrastructure.
The current Ebola outbreak in eastern DR Congo highlights the persistent vulnerability of the region to viral hemorrhagic fevers. For public health officials, the primary goal is now the rapid identification of new cases and the implementation of “ring vaccination” strategies to create a human buffer around infected individuals. However, the high mortality rate among the initial cluster of patients suggests that many may have reached treatment centers too late, or avoided them entirely due to security concerns.
As a physician, I have seen how the intersection of poverty and pathology creates a perfect storm. Ebola is not merely a biological event; it is a social and political one. In the eastern DRC, where displaced populations live in crowded conditions and healthcare facilities are often underfunded or targeted by armed groups, the virus finds an ideal environment to propagate. The loss of 65 people is not just a statistic—it represents a catastrophic blow to families already enduring the hardships of war.
The Mechanics of Transmission and Containment
Ebola virus disease is caused by an infection with a group of viruses within the genus Ebolavirus. It spreads through direct contact with the blood, secretions, organs, or other bodily fluids of infected people, as well as with surfaces and materials contaminated with these fluids. In the eastern DRC, traditional burial practices—which often involve touching the deceased—remain a significant driver of transmission, as the viral load in a body is highest immediately after death.
To combat this, the World Health Organization (WHO) and the DRC Ministry of Health have deployed specialized teams to conduct contact tracing. This involves identifying every person who came into contact with a confirmed case and monitoring them for 21 days—the maximum incubation period of the virus. If a contact develops a fever, they are immediately isolated to prevent further community spread.
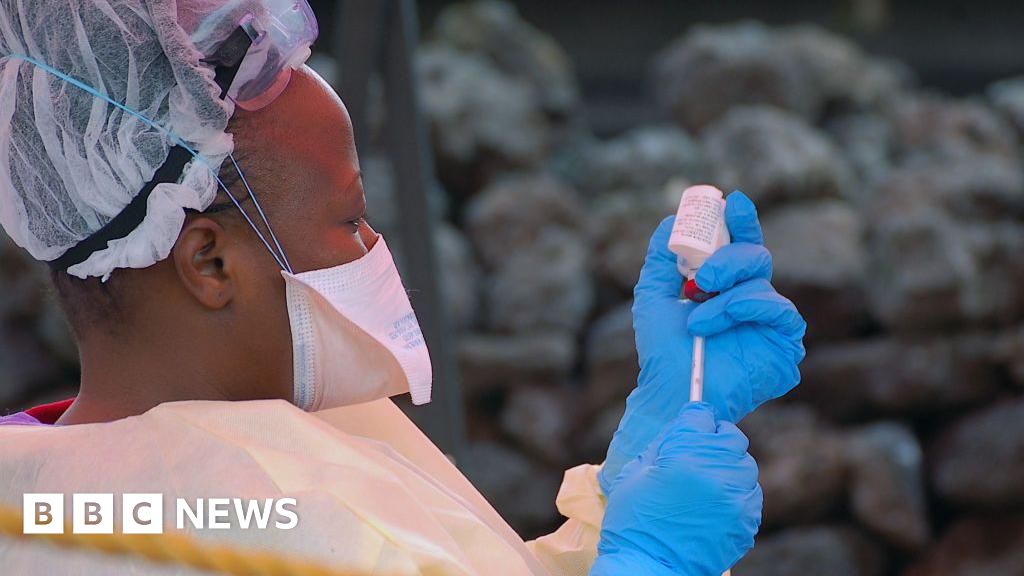
The deployment of the rVSV-ZEBOV vaccine has been a turning point in previous outbreaks. This vaccine, which has shown high efficacy in preventing the Zaire ebolavirus strain, is typically administered to frontline workers and the “rings” of contacts. However, the logistical hurdle of maintaining a strict cold chain—keeping vaccines at ultra-low temperatures—remains a daunting task in the tropical heat and rugged terrain of North Kivu and Ituri provinces.
The Conflict Catalyst
The geography of this outbreak is inextricably linked to the security situation in eastern DR Congo. The presence of various armed factions and the ongoing displacement of civilians create “blind spots” for surveillance. When villages are attacked or forced to flee, the continuity of care is broken, and patients with early symptoms may go unnoticed until they reach a more populated hub, effectively transporting the virus across provincial lines.
the “infodemic”—the rapid spread of misinformation—often accompanies these outbreaks. In regions where the state is viewed with suspicion, foreign medical teams in white hazmat suits can be perceived as intruders rather than healers. This mistrust has historically led to attacks on treatment centers and the hiding of sick relatives, which directly contributes to the rising death toll.
The current crisis underscores the need for “community-led” responses. Public health experts are increasingly prioritizing the involvement of local chiefs and religious leaders to communicate the safety of vaccines and the necessity of safe burials. Without the endorsement of trusted local voices, the most advanced medical interventions can be rendered ineffective.
Outbreak Summary and Current Metrics
The following table provides a snapshot of the current status of the outbreak based on available health reports.
| Metric | Verified Status | Primary Driver |
|---|---|---|
| Confirmed Deaths | 65 | Delayed treatment/Late presentation |
| Primary Location | Eastern DRC | High population mobility/Conflict |
| Primary Intervention | Ring Vaccination | rVSV-ZEBOV vaccine deployment |
| Risk Level | High (Regional) | Cross-border movement potential |
Clinical Outlook and Prevention
From a clinical perspective, early supportive care significantly improves the survival rate of Ebola patients. This includes aggressive fluid resuscitation, maintaining oxygen levels, and treating secondary infections. The introduction of monoclonal antibody treatments in recent years has further shifted the prognosis for those diagnosed early.
For those in or traveling to the affected regions, the guidelines remain strict:
- Avoid direct contact with the blood or bodily fluids of people who are sick or have died from Ebola.
- Practice rigorous hand hygiene using soap and water or alcohol-based rubs.
- Avoid contact with wildlife, particularly fruit bats and non-human primates, which can act as natural reservoirs for the virus.
- Report symptoms immediately, including fever, severe headache, muscle pain, and unexplained bleeding, to the nearest health authority.
Disclaimer: This article is for informational purposes only and does not constitute professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The international community is now closely monitoring the movement of people across the borders into Uganda and Rwanda to prevent a wider regional epidemic. The next critical checkpoint will be the upcoming weekly epidemiological report from the DRC Ministry of Health, which will determine if the growth curve of the outbreak has begun to flatten or if new clusters have emerged in previously unaffected villages.
We invite you to share this report to raise awareness and join the conversation in the comments below regarding the intersection of global health and regional stability.