A twisted ankle is one of the most common reasons patients seek immediate medical attention. Whether it happens during a weekend soccer game, a misstep on a curb, or a gym accident, the “rolled ankle” is a staple of the urgent care waiting room. For most, the injury is a simple sprain, but for a small percentage, it is a fracture that requires immobilization or surgery.
The challenge for clinicians in a rapid-paced environment is determining who actually needs an X-ray. While imaging provides certainty, the management of ankle sprains in urgent care often grapples with a tension between evidence-based guidelines and the impulse toward defensive medicine. When providers order imaging for every patient, the result is not necessarily better care, but rather increased healthcare costs and unnecessary radiation exposure.
To standardize this process, the medical community relies on the Ottawa Ankle Rules (OAR), a set of clinical decision tools designed to identify patients with a high probability of a fracture. When applied correctly, these rules allow providers to safely rule out the necessitate for imaging in the vast majority of patients, streamlining the path to recovery and reducing the burden on diagnostic resources.
The Science of the Ottawa Ankle Rules
Developed to reduce the volume of unnecessary radiographs, the Ottawa Ankle Rules are based on a specific physical examination of the ankle and midfoot. The rules are not based on a hunch, but on validated clinical markers that correlate strongly with the presence of a bone break. According to research hosted by the National Center for Biotechnology Information, the OAR maintain an incredibly high sensitivity, meaning they rarely miss a significant fracture.
The process involves a targeted assessment of bone tenderness and the patient’s ability to bear weight. If a patient does not meet the specific criteria for bone tenderness and can walk four steps—even with a limp—the likelihood of a fracture is clinically negligible. This allows the clinician to move directly to the treatment of a sprain, such as compression, elevation, and early mobilization, rather than waiting for imaging results.
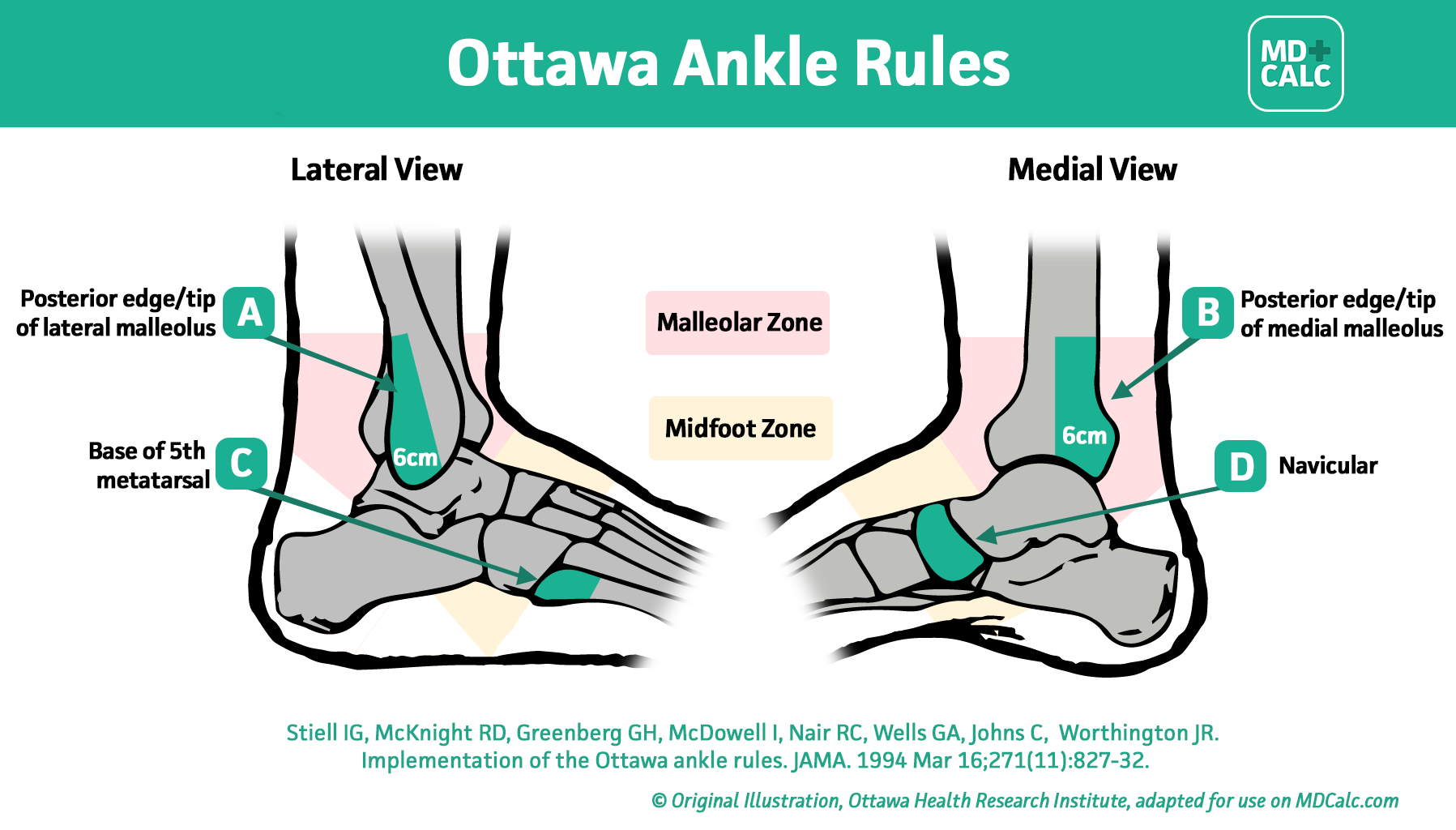
The criteria are divided between the ankle and the midfoot to ensure that fractures of the base of the fifth metatarsal or the navicular bone are not overlooked, as these injuries can mimic the pain of a standard sprain but require different management.
| Assessment Area | Criteria for X-ray Requirement |
|---|---|
| Ankle | Bone tenderness at the posterior edge or distal 6 cm of the lateral malleolus OR medial malleolus. |
| Midfoot | Bone tenderness at the base of the 5th metatarsal OR the navicular bone. |
| Weight Bearing | Inability to bear weight both immediately after the injury and in the clinic. |
The Gap Between Guidelines and Practice
Despite the proven efficacy of the OAR, adherence in urgent care settings is not universal. Many providers continue to order X-rays for patients who do not meet the clinical criteria. This phenomenon is often driven by “defensive medicine”—the practice of ordering tests to avoid potential litigation or the perceived risk of missing a rare injury, even when the statistical probability is near zero.

Patient expectations likewise play a significant role. In a consumer-driven healthcare model, patients often equate a “thorough” exam with the apply of technology. A patient may experience that their injury isn’t being taken seriously if they leave the clinic without an image of their bone. This pressure can lead clinicians to deviate from evidence-based protocols to satisfy the patient’s desire for visual confirmation.
But, this deviation has tangible consequences. While a single ankle X-ray carries a low dose of radiation, the cumulative effect of millions of unnecessary scans across the population is significant. The financial cost of unnecessary imaging contributes to the rising price of emergency and urgent care, often increasing the out-of-pocket expense for the patient without improving the clinical outcome.
Improving Outcomes Through Adherence
Bridging the gap between evidence and practice requires a shift in both clinic culture and operational workflows. Integrating the Ottawa Ankle Rules directly into Electronic Health Records (EHR) is one of the most effective ways to increase adherence. When a provider is prompted to check off specific OAR criteria before an imaging order can be submitted, the “default” becomes the evidence-based path.
Education also plays a critical role. When clinicians can confidently explain to a patient why an X-ray is not necessary—citing the high sensitivity of the OAR—patients are more likely to trust the diagnosis. This transforms the conversation from “I don’t think you need this” to “The clinical evidence shows that imaging will not change your treatment plan.”
The goal of modern musculoskeletal care is to move away from the “X-ray everything” mentality toward a model of precision diagnostics. By focusing on the physical exam and validated rules, urgent care centers can prioritize resources for patients who truly need surgical or orthopedic intervention, while guiding sprain patients toward faster, more efficient recovery paths.
For those managing a suspected sprain at home before visiting a clinic, the Mayo Clinic recommends the RICE method (Rest, Ice, Compression, and Elevation) to manage swelling, though a professional evaluation remains necessary to rule out instability or fracture.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As healthcare systems continue to integrate AI-driven decision support tools, the next step in the evolution of urgent care will likely involve real-time adherence monitoring to ensure that evidence-based guidelines are applied consistently across all patient populations. This shift promises to lower costs and reduce unnecessary radiation while maintaining the highest standards of patient safety.
Do you think healthcare providers rely too heavily on imaging, or is the “better safe than sorry” approach justified? Share your thoughts in the comments below.