The case of a persistent gastropleural fistula—an abnormal connection between the stomach and the pleural space—complicated by necrosis of the left lower lobe of the lung represents one of the most challenging scenarios in modern gastrointestinal and thoracic surgery. Such fistulas are exceedingly rare, typically arising as a devastating complication of bariatric surgery, trauma, or severe infection, and their management demands a multidisciplinary approach at specialized centers equipped to handle both the gastrointestinal and pulmonary sequelae.
For patients and clinicians alike, the diagnosis often arrives as a shock: a routine procedure or an injury has led to a cascade of events culminating in a fistula that refuses to close, coupled with the added threat of lung tissue death. The stakes are high. Untreated, a gastropleural fistula can lead to chronic infection, respiratory failure, and even death. Yet, despite its rarity, the condition is not without precedent, and recent case reports and clinical studies offer critical insights into the complexities of diagnosis, treatment, and long-term management.
Following surgery, patients with this dual pathology are typically transferred to a specialized upper gastrointestinal center for ongoing care and definitive fistula management. These centers, such as those affiliated with major academic medical institutions, bring together teams of surgeons, interventional radiologists, pulmonologists, and nutritionists to address both the fistula and the underlying lung necrosis. The goal is not only to close the fistula but also to restore respiratory function and prevent further complications.
What follows is a closer look at the medical intricacies of managing a persistent gastropleural fistula with necrotic lung tissue, the challenges faced by clinicians, and the emerging strategies that offer hope for patients in this rare and high-risk scenario.
—
The Anatomy of a Rare Complication
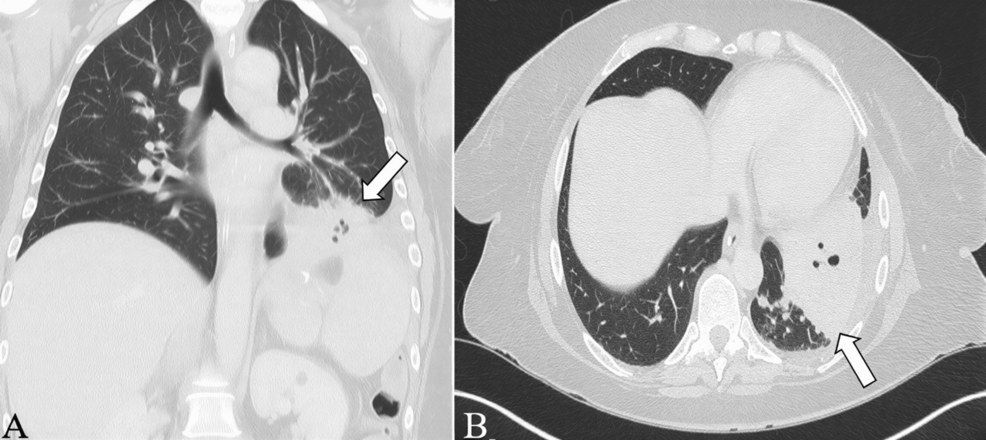
A gastropleural fistula occurs when an abnormal passage forms between the stomach and the pleural space, allowing gastric contents to leak into the chest cavity. This condition is most commonly reported after bariatric procedures such as Roux-en-Y gastric bypass or sleeve gastrectomy, though it can also result from blunt trauma, infection, or other surgical interventions. When accompanied by necrosis of the left lower lobe of the lung—a condition often linked to severe pneumonia, abscess formation, or multidrug-resistant infections—the clinical picture becomes even more complex.
Recent case studies, including those published in Clinical Case Reports and the Journal of the American College of Surgeons, highlight the rarity and severity of this dual pathology. In one notable report, a patient developed a gastropleural fistula following a sleeve gastrectomy, which was further complicated by left-sided pleural empyema—a purulent infection in the pleural space. The presence of necrotic lung tissue added another layer of difficulty, as it not only compromised respiratory function but also increased the risk of systemic infection and sepsis.
According to a 2023 case series, the development of such fistulas is often delayed, with symptoms—including chest pain, dyspnea, and persistent pleural effusion—emerging weeks or even months after the initial surgery or injury. This delayed presentation can lead to misdiagnosis, as clinicians may initially attribute symptoms to less severe conditions such as pleural effusion or chronic pneumonia.
—
Diagnosis: A Multidisciplinary Challenge
Accurate diagnosis of a gastropleural fistula with necrotic lung tissue requires a combination of imaging studies, endoscopic evaluations, and sometimes intraoperative findings. Computed tomography (CT) scans are typically the first line of investigation, revealing the presence of air or fluid in the pleural space—a hallmark of a fistula. Contrast studies, such as a gastrografin swallow, can further confirm the connection between the stomach and the pleural cavity.

However, the presence of necrotic lung tissue complicates the diagnostic process. Pulmonary imaging may show areas of cavitation, consolidation, or abscess formation, which can mimic other thoracic pathologies. In some cases, bronchoscopy or thoracoscopy may be necessary to directly visualize the affected lung tissue and assess the extent of necrosis.
Given the complexity of these cases, diagnosis often occurs in specialized centers where multidisciplinary teams can collaborate. For example, the Intestinal Failure Service at University College London Hospital (UCLH) is one such facility, known for its expertise in managing gastrointestinal fistulas and related complications.
—
Treatment: A Stepwise Approach to Closure and Recovery
Managing a persistent gastropleural fistula with necrotic lung tissue is a meticulous, often iterative process. The primary goals are to close the fistula, control infection, and restore respiratory and gastrointestinal function. Treatment typically involves a combination of surgical, endoscopic, and medical interventions.
Surgical Intervention: In many cases, surgical repair is the first step. This may involve re-anastomosis (reconnecting separated sections of the gastrointestinal tract), fistula takedown, or resection of necrotic lung tissue. However, surgery alone is often insufficient, particularly in the presence of extensive necrosis or infection.
Endoscopic Techniques: Endoscopic closure, using devices such as over-the-scope clips or endoscopic vacuum therapy, has emerged as a valuable adjunct to surgery. These techniques allow for minimally invasive closure of the fistula while minimizing trauma to surrounding tissues.
Medical Management: Broad-spectrum antibiotics are administered to control infection, while nutritional support is critical to ensure the patient has the strength to heal. In some cases, total parenteral nutrition (TPN) may be required to rest the gastrointestinal tract and promote fistula closure.
Interventional Radiology: Radiological drainage of pleural effusions or abscesses, combined with embolization techniques, can help stabilize the patient and reduce the risk of further complications.
A recent case report from the Henry Ford Jackson Hospital Research Symposium detailed the challenges of managing such a fistula after sleeve gastrectomy. The authors emphasized the importance of a tailored, stepwise approach, with close monitoring and adjustment of treatment based on the patient’s response.
—
Stakeholders and Support Systems
The management of a persistent gastropleural fistula with necrotic lung tissue involves a wide range of healthcare professionals, each playing a critical role in the patient’s care:
- Surgeons: Specialized in gastrointestinal and thoracic surgery, responsible for fistula repair and lung resection.
- Interventional Radiologists: Provide drainage and embolization to manage pleural effusions and abscesses.
- Pulmonologists: Monitor respiratory function and manage lung necrosis.
- Gastroenterologists: Assess and treat gastrointestinal complications.
- Nutritionists: Ensure adequate nutritional support for healing.
- Specialist Nurses: Provide ongoing care, education, and support for patients and families.
For patients, the emotional and physical toll of such a condition cannot be overstated. Support groups, psychological counseling, and clear communication from the medical team are essential components of care. Many specialized centers, such as those at Columbia University Irving Medical Center, offer comprehensive support services to help patients navigate this complex journey.
—
Why This Matters: The Broader Impact
The management of a persistent gastropleural fistula with necrotic lung tissue underscores the importance of specialized care in rare and complex medical conditions. For patients, the difference between life and death often hinges on access to a multidisciplinary team with the expertise and resources to address both the fistula and the underlying lung pathology.
From a public health perspective, these cases highlight the need for ongoing education and awareness among clinicians about the potential complications of bariatric surgery and other procedures that may lead to fistula formation. Early recognition and intervention can significantly improve outcomes and reduce the risk of long-term morbidity.
advances in endoscopic and interventional techniques are expanding the treatment options for patients with complex fistulas. As these technologies become more refined, the prognosis for individuals with persistent gastropleural fistulas may continue to improve.
—
Looking Ahead: The Next Steps in Care
For patients currently managing a persistent gastropleural fistula with necrotic lung tissue, the path to recovery is often long and uncertain. However, recent advancements in medical technology and a deeper understanding of fistula pathophysiology offer renewed hope. The next confirmed checkpoint in care typically involves:
- Regular follow-up imaging to monitor fistula closure and lung healing.
- Adjustments to medical or surgical treatment based on the patient’s progress.
- Ongoing nutritional and respiratory support to optimize recovery.
- Collaboration with specialized centers for innovative treatment options, such as advanced endoscopic techniques or experimental therapies.
Patients and families are encouraged to stay in close contact with their healthcare team and to participate in any clinical trials or research studies that may offer new avenues for treatment. For those seeking additional resources, organizations such as the Intestinal Failure Service at UCLH and the Columbia University Irving Medical Center provide comprehensive care and support.
—
If you or a loved one is facing a similar challenge, we invite you to share your experiences or questions in the comments below. Together, we can raise awareness and support those navigating the complexities of rare medical conditions.