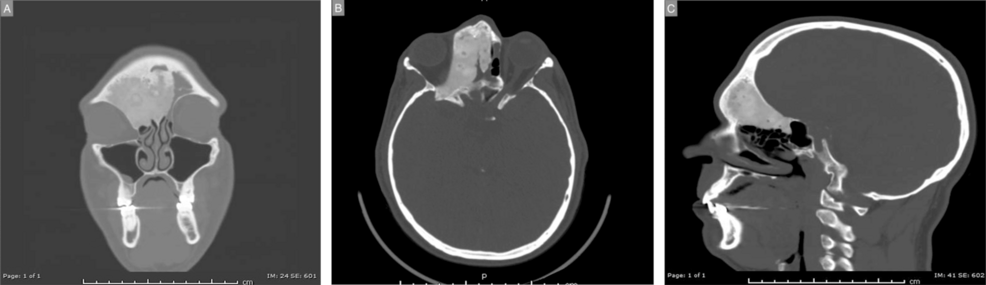
A rare surgical complication has highlighted the delicate balance required when reconstructing the orbital cavity after the removal of complex cranial tumors. In a detailed clinical case, surgeons documented a patient developing pulsatile exophthalmos due to inadequate orbital reconstruction following fronto-orbito-ethmoidal fibrous dysplasia resection, a condition where the eye visibly pulses in sync with the heartbeat.
The case centers on a patient suffering from fibrous dysplasia, a bone disorder where normal bone is replaced by fibrous tissue. In this specific instance, the growth affected the fronto-orbito-ethmoidal region—the area encompassing the forehead, the eye socket, and the ethmoid sinuses—leading to significant facial deformity and pressure on the ocular structures.
While the primary goal of the initial resection was to remove the dysplastic bone and relieve pressure, the subsequent failure to fully seal the orbital walls created a communication between the intracranial space and the orbit. This allowed cerebrospinal fluid (CSF) and arterial pulsations to transmit directly to the globe of the eye, resulting in the rhythmic protrusion known as pulsatile exophthalmos.
As a physician and medical writer, I recognize that this case serves as a critical reminder for surgical teams: the success of a resection is not merely defined by the removal of a lesion, but by the integrity of the reconstruction that follows. When the “container” of the eye is compromised, the physiological pressures of the brain can manifest in startling ways.
Understanding the Mechanics of Pulsatile Exophthalmos
To understand why this occurs, one must look at the anatomy of the orbit. The eye sits in a bony socket that is designed to protect the globe and maintain a specific pressure environment. When a large portion of this bone is removed—as is often necessary in cases of extensive fibrous dysplasia—the structural integrity of the orbit is lost.

If the reconstruction is inadequate, a “gap” or defect remains. This creates a pathway for the pulsations of the cerebrospinal fluid and the arterial blood flow from the cavernous sinus or carotid artery to push the eye forward. This is distinct from standard exophthalmos (protrusion of the eye), as the movement is rhythmic and coincides exactly with the patient’s pulse.
In this specific patient’s journey, the timeline of events underscores the complexity of the recovery process:
- Initial Diagnosis: Identification of fronto-orbito-ethmoidal fibrous dysplasia causing ocular displacement.
- Primary Surgery: Extensive resection of the fibrous bone to debulk the mass and restore facial symmetry.
- Post-Operative Phase: Appearance of pulsatile movement of the eye, indicating a failure in the orbital wall reconstruction.
- Corrective Intervention: A second surgical procedure to seal the orbital defect and isolate the eye socket from intracranial pulsations.
The Challenge of Fibrous Dysplasia Resection
Fibrous dysplasia is an unpredictable condition. Because the abnormal bone is often porous and poorly vascularized, it can be difficult for surgeons to determine where the “diseased” bone ends and healthy bone begins. In the fronto-orbito-ethmoidal region, the proximity to the brain, the optic nerve, and the sinuses makes the surgery high-risk.
The surgical objective is a “debulking” process. However, removing too much bone can leave the orbit unstable. The case emphasizes that using grafts or synthetic materials to rebuild the orbital floor and walls is not optional—it is a requirement to prevent the transmission of intracranial pressure to the orbital contents.
| Feature | Pre-Resection (Dysplasia) | Post-Resection (Inadequate) | Post-Corrective Reconstruction |
|---|---|---|---|
| Eye Position | Displaced/Protruding | Pulsatile Protrusion | Stable/Neutral |
| Orbital Wall | Thickened/Deformed | Deficient/Open | Reconstructed/Closed |
| Symptom | Pressure/Deformity | Rhythmic Pulsation | Resolution of Pulsation |
Clinical Implications and Surgical Takeaways
The resolution of this case came through a secondary reconstruction. By utilizing autologous bone grafts or biocompatible implants to close the gap in the orbital wall, surgeons were able to stop the transmission of the pulse. This effectively “re-contained” the eye, returning it to a stable position and eliminating the pulsatile movement.
For clinicians and patients, this case highlights several key diagnostic and therapeutic points:
First, any patient presenting with a pulsing eye following cranial or orbital surgery must be evaluated for a CSF leak or an orbital wall defect. This is a medical urgency, as a communication between the brain and the external environment increases the risk of meningitis.
Second, the use of advanced imaging, such as CT scans and MRIs, is essential not just for planning the resection, but for verifying the “watertight” nature of the reconstruction. The absence of a visible pulse during a physical exam does not always signify the reconstruction is sufficient; subtle defects can still lead to long-term complications.
Finally, the multidisciplinary approach—combining the skills of a neurosurgeon, an ophthalmologist, and a plastic surgeon—is the gold standard for managing these complex craniofacial anomalies. The coordination between these specialties ensures that while the tumor is removed, the functional and aesthetic integrity of the eye is preserved.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should consult with a qualified healthcare provider for diagnosis and treatment of any medical condition.
The medical community continues to refine the materials used for orbital reconstruction, with ongoing research into 3D-printed patient-specific implants that may reduce the risk of inadequate closure in future cases. The next phase of clinical improvement will likely involve the integration of real-time intraoperative imaging to ensure orbital wall integrity before the patient leaves the operating room.
Do you have experience with complex facial surgeries or rare bone disorders? We invite you to share your thoughts or questions in the comments below.