A rare and severe manifestation of scrub typhus has highlighted the critical importance of early diagnostic suspicion in patients presenting with neurological distress and systemic failure. A documented case of scrub typhus presenting with meningoencephalitis and multiorgan dysfunction syndrome demonstrates how a common zoonotic infection can rapidly evolve into a life-threatening emergency when the bacteria breach the blood-brain barrier.
Scrub typhus is caused by the bacterium Orientia tsutsugamushi and is typically transmitted to humans through the bite of infected larval mites, known as chiggers. While many cases present as a self-limiting febrile illness, a small percentage of patients develop severe complications. The intersection of central nervous system (CNS) involvement and multiorgan dysfunction syndrome (MODS) creates a complex clinical picture that can easily be mistaken for other forms of bacterial meningitis or viral encephalitis.
As a physician and medical writer, I have seen how “diagnostic overshadowing” can occur when a patient presents with a whirlwind of symptoms—fever, altered mental status, and kidney failure—leading clinicians to overlook the possibility of a rickettsial infection. In this specific case, the progression from a simple fever to a state of coma and systemic collapse underscores the narrow window for effective intervention.
The Clinical Cascade: From Fever to Systemic Failure
The progression of the disease in this instance followed a perilous trajectory. The patient initially presented with non-specific symptoms, including high-grade fever, and malaise. However, the clinical picture shifted rapidly toward neurological impairment. The development of meningoencephalitis—inflammation of both the brain and the surrounding membranes—led to a diminished level of consciousness and eventual coma.
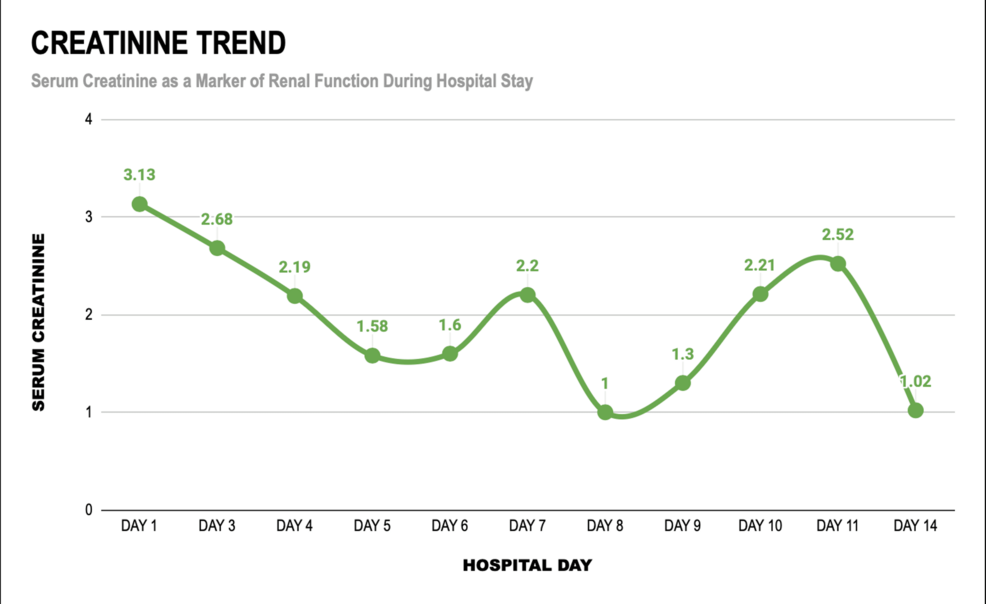
Simultaneously, the patient entered a state of multiorgan dysfunction syndrome. MODS occurs when the body’s inflammatory response to an infection becomes systemic, leading to the failure of two or more organ systems. In this case, the impact was seen across the renal and respiratory systems, necessitating intensive care interventions such as mechanical ventilation and renal replacement therapy.
The diagnostic challenge in these cases often stems from the absence of the “classic” sign of scrub typhus: the eschar. An eschar is a small, painless, cigarette-burn-like scab that forms at the site of the mite bite. When this hallmark is missing or overlooked during a physical examination, clinicians may not consider Orientia tsutsugamushi until the patient is already in critical condition.
Understanding the Pathogen and Transmission
The bacteria responsible for this condition are obligate intracellular pathogens, meaning they must live inside host cells to survive and replicate. They primarily target the endothelial cells lining the blood vessels, causing widespread vascular leakage and inflammation. This systemic vasculitis is what leads to the “leaky” organs characteristic of multiorgan dysfunction.
The geography of risk is primarily the “tsutsugamushi triangle,” an area encompassing Southeast Asia, China, Japan, and parts of Northern Australia. However, as global travel increases and environmental conditions shift, the risk of encountering these larval mites extends to anyone spending time in scrublands, grasslands, or forested areas. According to the Centers for Disease Control and Prevention (CDC), rickettsial diseases often require specific antibiotic treatments that differ from standard pneumonia or meningitis protocols.
| Stage | Common Symptoms | Severe Complications |
|---|---|---|
| Early Phase | Fever, headache, myalgia | Eschar formation |
| Neurological Phase | Confusion, irritability | Meningoencephalitis, Coma |
| Systemic Phase | Low blood pressure, edema | MODS, ARDS, Acute Kidney Injury |
The Critical Role of Doxycycline
The turning point in the management of scrub typhus presenting with meningoencephalitis and multiorgan dysfunction syndrome is the administration of appropriate antimicrobial therapy. Doxycycline, a tetracycline antibiotic, remains the gold standard for treatment. Because the bacteria reside inside cells, the drug must be able to penetrate the cellular membrane effectively.
In severe cases, the delay in starting doxycycline can lead to irreversible organ damage. In the reported case, the initiation of targeted therapy was the catalyst for the patient’s stabilization. Once the bacterial load was reduced, the inflammatory cascade began to subside, allowing for the gradual weaning of ventilatory support and the recovery of renal function.
Medical professionals are urged to maintain a high index of suspicion for scrub typhus in any febrile patient returning from an endemic area, even if the presentation seems “atypical” or purely neurological. Waiting for laboratory confirmation—which can be gradual or produce false negatives—can be fatal. Empiric treatment is often recommended while awaiting results.
Long-term Implications and Recovery
Recovery from a state of MODS and meningoencephalitis is rarely instantaneous. Patients often face a prolonged period of rehabilitation to regain cognitive functions and physical strength. The neurological impact of the inflammation can leave lasting deficits if the brain was deprived of oxygen or suffered significant swelling (cerebral edema) during the acute phase.
Public health efforts focus on prevention through the leverage of insect repellents containing DEET and the wearing of protective clothing in high-risk areas. Because there is currently no widely available vaccine for scrub typhus, avoidance of the larval mite remains the only foolproof prevention strategy.
For those seeking more information on zoonotic infections and travel health, the World Health Organization (WHO) provides updated guidelines on managing emerging infectious diseases in endemic regions.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult a licensed healthcare provider for diagnosis and treatment of any medical condition.
The medical community continues to monitor the prevalence of Orientia tsutsugamushi as climate patterns alter the habitats of the mite vectors. Future updates from regional health ministries are expected to clarify if current antibiotic resistance patterns are affecting the efficacy of doxycycline in specific geographic clusters.
Do you have questions about zoonotic diseases or travel safety? Share this article or leave a comment below to join the conversation.