Imagine drifting toward sleep, the world around you fading into a quiet hum, when suddenly a sound like a bomb detonating, a cymbal crashing, or a door slamming shut erupts inside your skull. You bolt upright, heart racing, searching the room for the source of the noise, only to find a heavy, undisturbed silence. For those experiencing Exploding Head Syndrome (EHS), this is not a nightmare, but a startlingly real sensory phenomenon.
Despite its alarming name, Exploding Head Syndrome is a benign parasomnia—a category of sleep disorders that involve unusual movements or perceptions during sleep. While the experience can be profoundly disorienting and often triggers intense anxiety or a fear of stroke or brain aneurysm, it is physically harmless. As a physician, I often see patients who are terrified by these episodes, unaware that they are experiencing a documented, albeit rare, neurological glitch during the transition between wakefulness and sleep.
The hallmark of Exploding Head Syndrome is the perception of a loud, imagined noise that occurs during the hypnagogic state (falling asleep) or the hypnopompic state (waking up). Because the event happens internally, there is no external sound for a partner to hear, which often leads patients to worry that they are experiencing a psychiatric break or a severe medical crisis. However, clinical evidence suggests that EHS is more common than previously thought, often underreported simply because patients are too embarrassed or frightened to describe it.
The Mechanics of a Sensory Glitch
While the exact etiology of EHS remains a subject of clinical debate, the prevailing theory involves a “misfire” in the brain’s reticular formation. Normally, as we transition into sleep, the brain shuts down various sensory systems in a coordinated sequence. In a person experiencing EHS, it is believed that there is a delay in this shutdown process. Instead of the auditory neurons silencing gradually, they fire all at once in a massive, synchronized burst, creating the perception of a sudden, loud noise.

This phenomenon is closely related to other sleep-onset experiences, such as the hypnic jerk—that sudden feeling of falling that snaps you awake. In both cases, the brain is struggling to navigate the boundary between consciousness and unconsciousness. Some patients also report seeing a flash of light accompanying the sound, suggesting that the neural surge may occasionally affect the visual cortex as well.
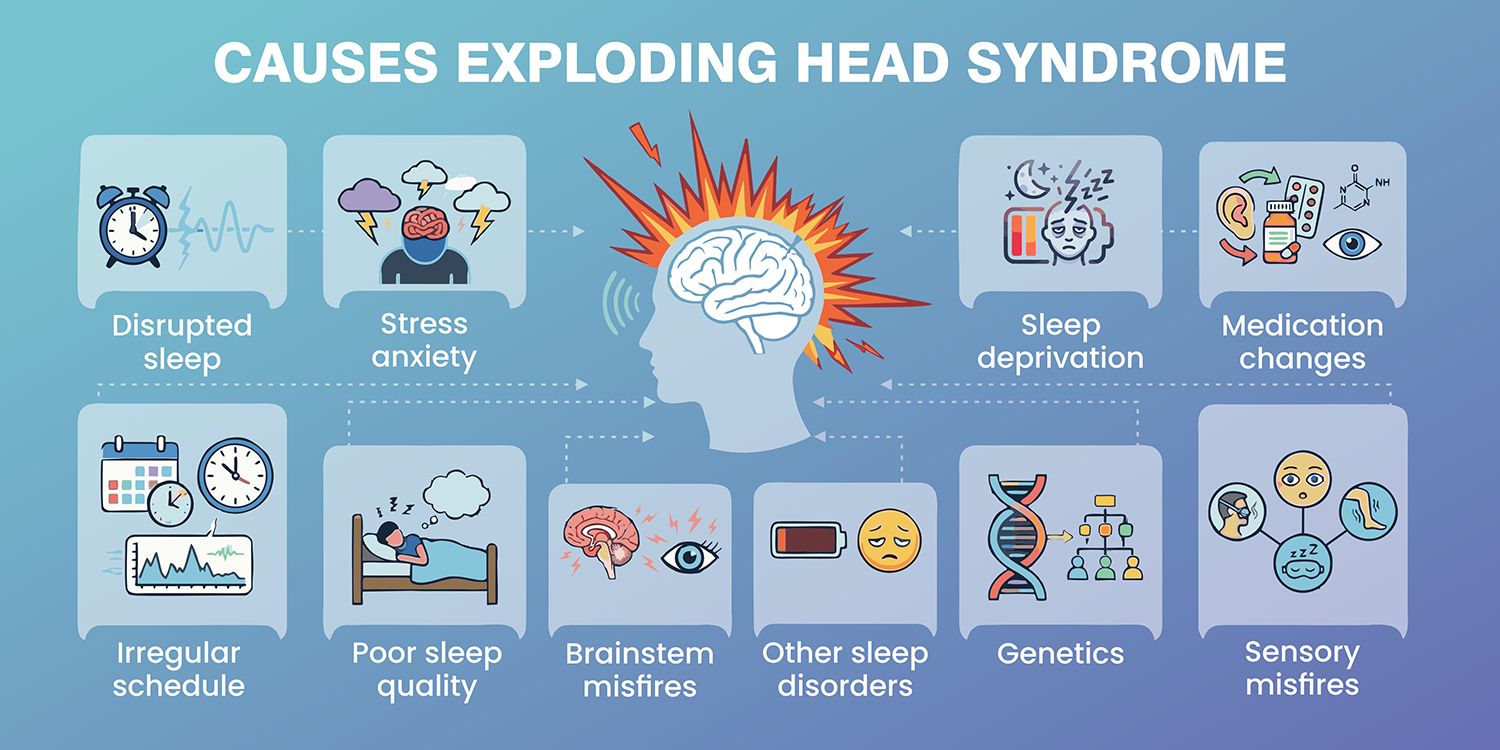
Research indicates that certain triggers can increase the frequency of these episodes. High levels of stress, chronic anxiety, and severe sleep deprivation are the most common catalysts. When the nervous system is hyper-aroused, the transition into sleep becomes more volatile, increasing the likelihood of these sensory bursts.
Identifying and Diagnosing the Phenomenon
Diagnosing EHS is primarily a clinical process based on a patient’s history. Because the episodes are sporadic and occur during the transition to sleep, they are notoriously difficult to capture in a traditional clinical setting. However, several tools are used to rule out other conditions and confirm the pattern of the disorder.
Physicians often recommend a sleep diary, where patients record the timing, frequency, and nature of the sounds, as well as their stress levels and caffeine intake leading up to the event. In more complex cases, a referral to a sleep laboratory for polysomnography—a comprehensive study of brain waves, oxygen levels, and heart rate—may be necessary. While EHS typically does not produce a distinct signature on an EEG, these tests are vital to ensure the patient is not experiencing nocturnal seizures or obstructive sleep apnea.
Differentiating EHS from Other Conditions
It is critical to distinguish EHS from other neurological or auditory issues. The primary differentiator is the absence of pain and the specific timing of the event. The following table outlines the key distinctions between EHS and similar sensory experiences.
| Feature | Exploding Head Syndrome | Tinnitus | Nocturnal Seizures |
|---|---|---|---|
| Timing | Sleep onset or awakening | Constant or intermittent | Variable/During sleep |
| Sound Type | Sudden “bang” or “crash” | Ringing, buzzing, hissing | Variable/Often rhythmic |
| Pain | None | None (usually) | Possible post-ictal headache |
| Duration | Instantaneous | Continuous or prolonged | Seconds to minutes |
Management and Practical Relief
For the vast majority of people, the most effective “treatment” for EHS is simply education. Understanding that the condition is benign and non-dangerous often reduces the anxiety associated with the episodes, which in turn reduces their frequency.

When episodes become frequent enough to disrupt sleep quality or cause significant daytime anxiety, a focus on sleep hygiene and stress reduction is recommended. Practical steps include:
- Establishing a consistent sleep schedule: Waking and sleeping at the same time every day helps stabilize the brain’s transition phases.
- Reducing stimulants: Limiting caffeine and nicotine, especially in the afternoon and evening, lowers the state of neural hyper-arousal.
- Stress management: Incorporating mindfulness, progressive muscle relaxation, or cognitive behavioral therapy (CBT) can lower the baseline anxiety that often triggers EHS.
- Optimizing the sleep environment: Using white noise machines can sometimes mask the transition and provide a soothing auditory backdrop that prevents the “startle” response.
In rare, severe cases where EHS leads to chronic insomnia, physicians may consider low-dose medications to stabilize sleep patterns, though this is generally a last resort given the benign nature of the syndrome. Most patients find that as their overall stress levels decrease, the episodes naturally subside.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As sleep science evolves, researchers are looking closer at the intersection of sensory processing and the architecture of the dreaming brain. Future studies focusing on functional MRI (fMRI) during sleep transitions may provide a clearer picture of why some individuals are predisposed to these auditory bursts. For now, the medical consensus remains clear: while the “explosion” feels catastrophic, it is merely a noisy hiccup in the brain’s journey toward rest.
Have you or a loved one experienced these startling sleep events? We invite you to share your experience in the comments or share this article with someone who may be searching for answers.

