It began with a small, frustrating realization: a hand that wouldn’t quite obey, a reach for a TV remote that ended in a clumsy miss. For one individual sharing their story during World Stroke Day, the inability to grab a TV box wasn’t just a momentary lapse in coordination—it was the first signal of a neurological emergency. This subtle failure of motor control is often the only warning a person gets before a stroke fundamentally alters their life.
As a physician, I have seen this pattern countless times. The tragedy of stroke is not just the event itself, but the time lost to doubt. Patients often describe a “denial phase,” where they attribute sudden weakness or confusion to fatigue, age, or a temporary dizzy spell. However, in the context of a stroke, hesitation is the enemy. When a blood clot blocks an artery to the brain or a vessel ruptures, the brain begins to lose millions of neurons every minute.
World Stroke Day serves as a critical annual reminder that stroke recognition is a survival skill. While the HBVL report highlights the personal nature of these symptoms, the broader medical imperative is clear: recognizing the “small” signs—like the inability to reach for an object—can be the difference between a full recovery and permanent disability.
The Anatomy of a Warning: Why Subtle Signs Matter
Most people imagine a stroke as a dramatic collapse, but the reality is often more insidious. The incident involving the TV box is a classic example of hemiparesis—weakness on one side of the body. This occurs when the motor cortex in one hemisphere of the brain is deprived of oxygen, causing the opposite side of the body to lose strength or coordination.

These “micro-failures” are often overlooked because they don’t feel like a crisis. A slight slur in speech might be dismissed as tiredness; a drooping eyelid might be ignored as a lack of sleep. Yet, these are the brain’s distress signals. Whether it is a Transient Ischemic Attack (TIA)—often called a “mini-stroke”—or a full-scale ischemic event, these symptoms indicate that the brain’s blood supply is compromised.
The danger of the TIA is that symptoms often resolve quickly, leading patients to believe the danger has passed. In reality, a TIA is a profound warning shot; it suggests that a more severe stroke is imminent and requires immediate medical intervention to prevent a catastrophic outcome.
Decoding Quick: The Gold Standard of Recognition
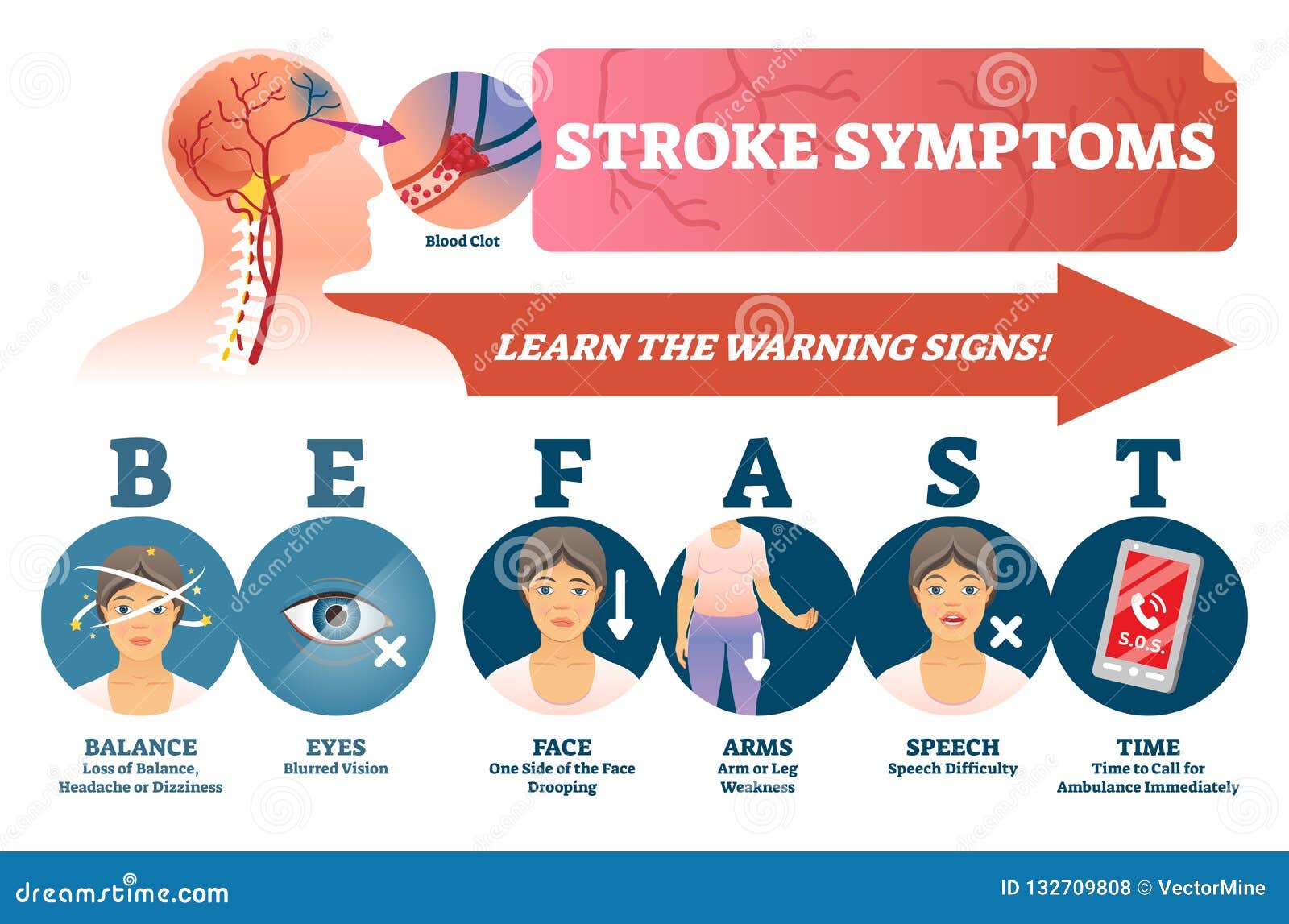
To strip away the guesswork, medical professionals worldwide promote the FAST acronym. It is designed to be intuitive, allowing bystanders or the patients themselves to identify a stroke in seconds. When a person experiences a symptom like the one described in the HBVL account, the FAST check should be the immediate next step.
- Face: Ask the person to smile. Does one side of the face droop? Is the smile uneven?
- Arms: Ask the person to raise both arms. Does one arm drift downward? Is there a noticeable lack of strength in one limb?
- Speech: Ask the person to repeat a simple phrase. Is their speech slurred or strange? Do they seem confused or unable to find the right words?
- Time: If any of these signs are present, call emergency services immediately. Time is the most critical variable in stroke treatment.
The “Time” element is not merely about getting to the hospital; it is about the specific window for life-saving interventions. For certain types of strokes, the administration of clot-busting medications is only effective within a few hours of the onset of symptoms.
The Medical Race: Time is Brain
Once a patient reaches the emergency department, the primary goal is to determine the type of stroke. This represents usually done via a CT scan or MRI to differentiate between an ischemic stroke (a blockage) and a hemorrhagic stroke (a bleed). The treatments for these two events are diametrically opposed; giving a clot-buster to someone with a brain bleed could be fatal.
| Stroke Type | Primary Cause | Key Intervention | Critical Window |
|---|---|---|---|
| Ischemic | Blood clot blocking an artery | tPA (Thrombolysis) or Thrombectomy | Typically 3 to 4.5 hours for tPA |
| Hemorrhagic | Ruptured blood vessel (bleed) | Blood pressure control / Surgery | Immediate / Emergency surgical eval |
For ischemic strokes, the “golden hour” is the priority. Thrombolytic agents, such as alteplase (tPA), work by dissolving the clot and restoring blood flow. In more severe cases, a mechanical thrombectomy—where a surgeon physically removes the clot using a catheter—can be performed, sometimes extending the treatment window for specific large-vessel occlusions.
Mitigating Risk and Long-Term Recovery
While the immediate focus is on emergency response, the long-term strategy is prevention. Stroke is not an inevitable part of aging; many risk factors are modifiable. Managing hypertension (high blood pressure) is the single most effective way to reduce stroke risk, as it prevents both the buildup of plaques in the arteries and the weakening of vessel walls that leads to hemorrhage.
Other critical preventative measures include:
- Atrial Fibrillation (AFib) Management: An irregular heartbeat can allow clots to form in the heart, which then travel to the brain.
- Cholesterol Control: Reducing LDL cholesterol prevents the atherosclerosis that leads to ischemic blockages.
- Lifestyle Adjustments: Smoking cessation and the reduction of highly processed sodium-rich foods significantly lower vascular strain.
For those who have already survived a stroke, the journey shifts to neuroplasticity. Through intensive physical, occupational, and speech therapy, the brain can often “rewire” itself, allowing other areas to take over the functions of the damaged tissue. The success of this recovery is heavily dependent on how quickly the initial stroke was treated.
Disclaimer: This article is provided for informational purposes only and does not constitute professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Looking ahead, health organizations continue to push for expanded access to “stroke units”—specialized hospital wards that have shown significantly better patient outcomes than general wards. The next major milestone in public health awareness will be the continued integration of AI-driven triage in ambulances, allowing imaging to begin before the patient even reaches the hospital doors.
Do you or a loved one have a plan for recognizing stroke symptoms? Share this guide with your family or leave a comment below to help spread awareness.

