For Bryan Maples, the warning signs didn’t arrive with a dramatic crash or a sudden collapse. Last December, the 40-year-old Riverton, Utah, resident simply felt “off.” There was no acute pain, no fever, and no feeling of sickness—only a persistent, unsettling weakness on the left side of his body.
Maples acted on a gut feeling and sought care at Intermountain Health Riverton Hospital. It was there he learned he had suffered a stroke. While the experience was jarring, Maples credits his quick decision to seek medical attention for his recovery. “I was lucky enough to get there as quickly as I did,” Maples said, noting that those who ignore symptoms often face far more permanent disabilities.
His experience underscores a critical reality in emergency medicine: when it comes to recognizing stroke symptoms, minutes are the only currency that matters. A stroke occurs when the brain’s blood supply is interrupted, depriving neurons of oxygen and nutrients. Because brain cells begin to die almost immediately, the window for effective intervention is narrow.
According to the Centers for Disease Control and Prevention (CDC), stroke remains a leading cause of death and long-term disability in the United States, accounting for approximately one in 20 adult deaths and ranking as the fifth leading cause of death overall. However, medical professionals emphasize that the outcome of a stroke is heavily dictated by the speed of treatment.
The Biological Clock: Ischemic vs. Hemorrhagic
Not all strokes are the same, and the distinction is vital for determining the correct treatment. Physicians generally categorize strokes into two primary types: ischemic and hemorrhagic.
An ischemic stroke occurs when an artery supplying blood to the brain becomes clogged or closed off by a clot. This is the most common form, accounting for approximately 85% of all cases. In contrast, a hemorrhagic stroke happens when a blood vessel ruptures, causing blood to leak into or around the brain tissue, creating pressure and damage.
| Stroke Type | Primary Cause | Approximate Prevalence |
|---|---|---|
| Ischemic | Blood clot or artery blockage | ~85% |
| Hemorrhagic | Ruptured blood vessel/bleeding | ~15% |
Because the treatments for these two types are diametrically opposed—one aims to dissolve a clot, while the other aims to stop bleeding—rapid diagnostic imaging in an emergency department is the only way to ensure a patient receives the correct intervention.
The BE FAST Framework for Recognition
Because stroke symptoms can be subtle or vary depending on which part of the brain is affected, neurology experts recommend a simple mnemonic to help the public identify a crisis in real time. Jennelle Newman, NP, an Advanced Practice Provider with Intermountain Health Neurology, advocates for the “BE FAST” method.
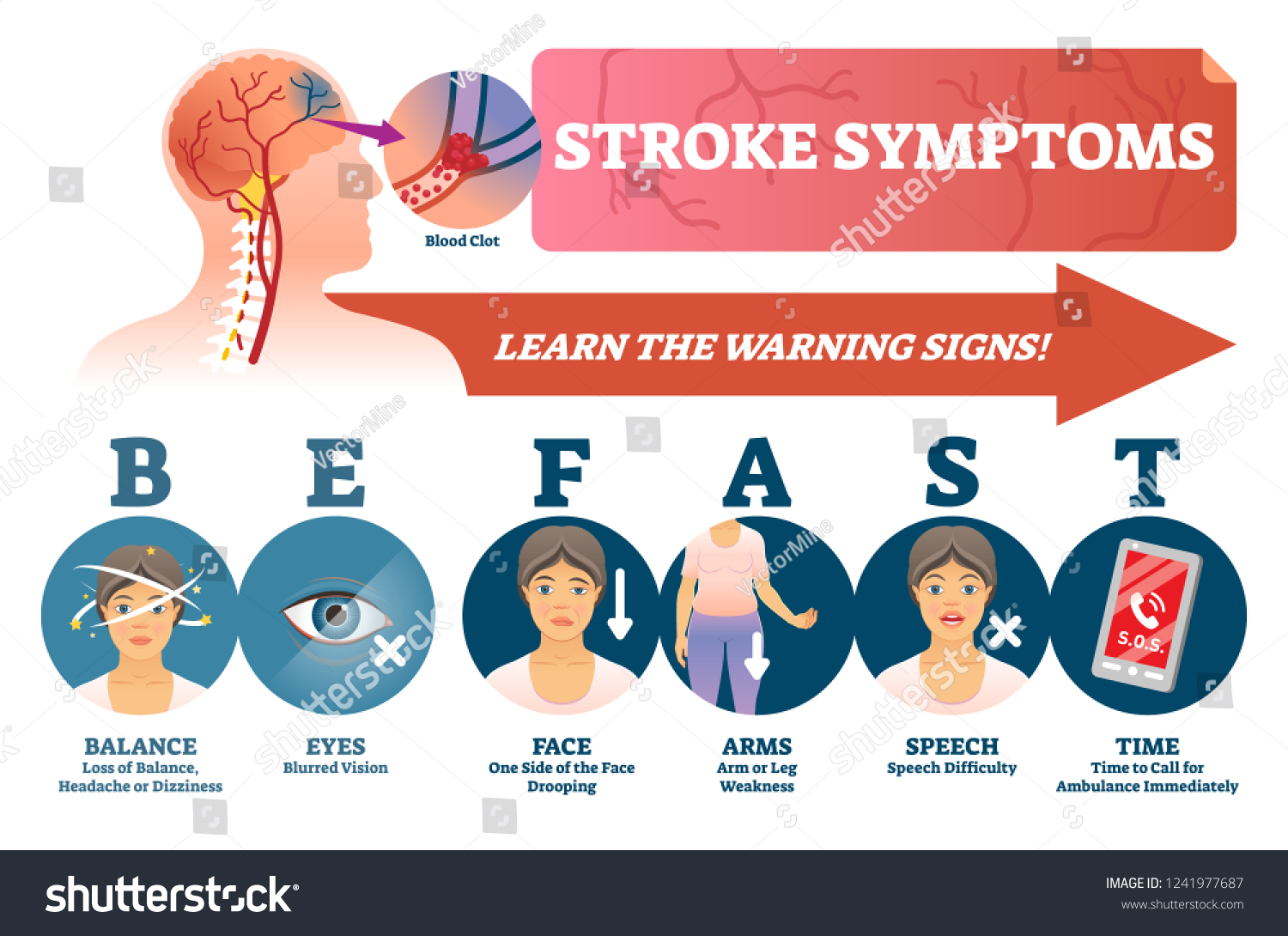
Balance: Watch for a sudden loss of coordination or difficulty with balance. This can manifest as stumbling or an inability to stand straight.
Eyes: Look for sudden blurred vision, double vision, or a complete loss of vision in one or both eyes that occurs without pain.
Face: Check for drooping or numbness on one side of the face. A common test is to ask the person to smile; if one side of the mouth lags, it is a red flag.
Arm: Note any sudden weakness or numbness in one arm. Asking the person to raise both arms can reveal if one drifts downward.
Speech: Listen for slurring, difficulty finding words, or a total inability to speak. The person may also struggle to understand simple commands.
Time: This is the most critical element. Note the exact time when the person last exhibited normal symptoms and call 911 immediately. Do not drive the person to the hospital yourself; paramedics can begin the triage process and alert the stroke team before the patient even arrives at the doors.
Time-Sensitive Interventions and Recovery
Once a patient reaches the hospital, the goal is the immediate restoration of blood flow to prevent further brain tissue death. For those suffering from ischemic strokes, two primary treatments are often utilized, both of which are strictly time-dependent.
The first is tissue plasminogen activator (tPA), a powerful medication designed to dissolve the blood clot and reopen the artery. The second is a mechanical thrombectomy, a procedure where surgeons use a catheter to physically pull the clot out of a large artery in the brain.
“Quick medical treatment during a stroke is one of the most important factors in determining a good outcome,” Newman said. She noted that while these treatments can significantly reduce long-term disability, they must be administered within a very specific window following the onset of symptoms to be safe and effective.
Reducing the Risk: The 80% Preventability Factor
While some risk factors are genetic or tied to family history, the vast majority of strokes are not inevitable. Public health data suggests that approximately 80% of strokes in America are preventable through a combination of medication adherence and lifestyle modifications.
The single most significant risk factor for stroke is high blood pressure (hypertension). When blood pressure remains chronically elevated, it damages the arteries, making them more likely to clog or burst. Managing this through blood pressure medications, statins for cholesterol, and blood thinners like aspirin—when prescribed by a physician—can drastically lower a person’s risk profile.
Beyond medication, neurologists recommend several evidence-based lifestyle changes to protect brain health:
- Physical Activity: Engaging in at least 30 minutes of moderate exercise on most days of the week, provided it is cleared by a doctor.
- Dietary Shifts: Prioritizing fruits, vegetables, and low-fat dairy while reducing the intake of refined grains (such as white bread), sweets, and saturated meats.
- Sodium Reduction: Lowering salt intake to help manage blood pressure.
- Substance Control: Stopping smoking and limiting alcohol consumption (no more than one drink per day for women and two for men).
- Weight Management: Working toward a healthy weight to reduce the strain on the cardiovascular system.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As May marks Stroke Awareness Month, health providers are encouraging individuals to schedule routine check-ups with primary care providers. Establishing a baseline for blood pressure and cholesterol now allows patients and doctors to create a preventative plan before a crisis occurs.
We invite you to share this guide with your family and friends to help them recognize the signs of a stroke. Have you or a loved one navigated a stroke recovery? Share your experience in the comments below.

