Elon Musk is known for timelines that stretch the boundaries of possibility, from Mars colonies to fully autonomous taxis. His latest assertion—that within three years, expert surgical robots will outnumber human surgeons on Earth—has sparked a familiar wave of excitement and skepticism. But, for those of us who spend our days in the operating room and the research lab, the gap between a programmed movement and a surgical decision is a chasm that cannot be bridged by a few years of software updates.
The debate over the autonomous surgery timeline often centers on precision. To the casual observer, a robot’s ability to stitch a wound with sub-millimeter accuracy looks like the finish line. But in clinical practice, precision is the easy part. The true challenge of surgery is adaptability—the ability to pivot in real-time when a patient’s anatomy doesn’t match the textbook, or when a sudden hemorrhage turns a routine procedure into a crisis.
While we are seeing breathtaking leaps in surgical AI, the transition from “robot-assisted” to “fully autonomous” is not a linear path. It is a fundamental shift in how we handle biological unpredictability.
The Precision Paradox: Why Accuracy Isn’t Enough
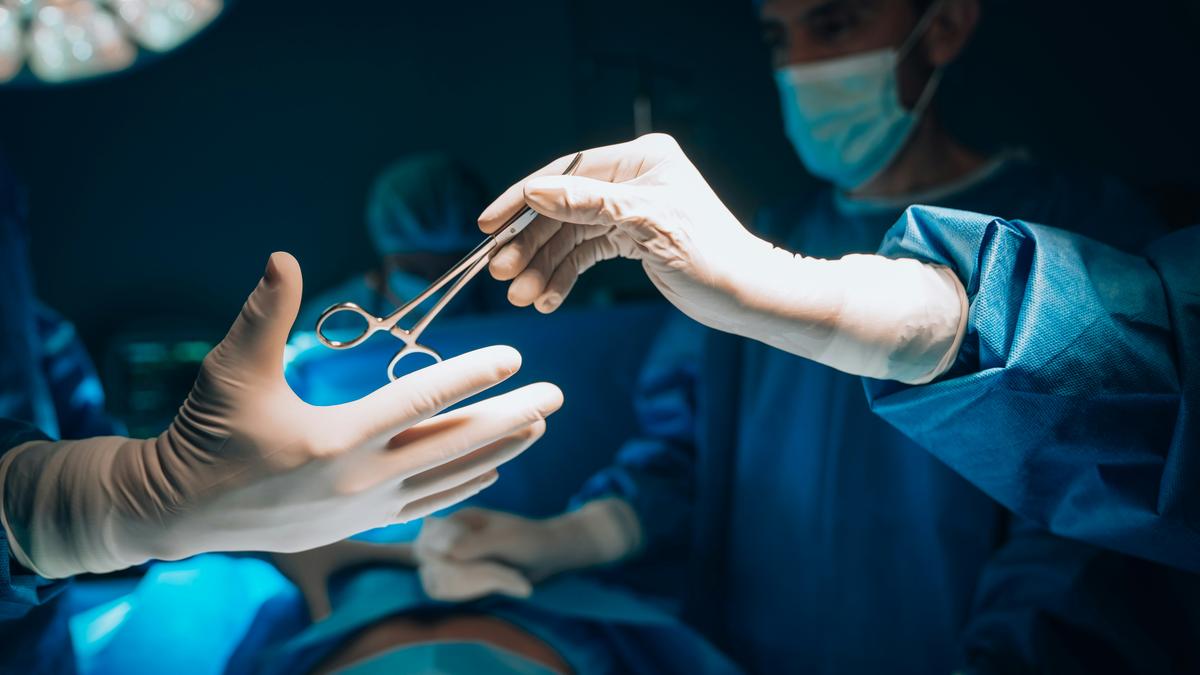
Current robotic-assisted surgery, dominated by systems like the da Vinci surgical system, is not autonomous. These are teleoperated tools; they act as sophisticated extensions of the surgeon’s hands, filtering out tremors and providing high-definition 3D views. The human is the pilot; the robot is the aircraft.
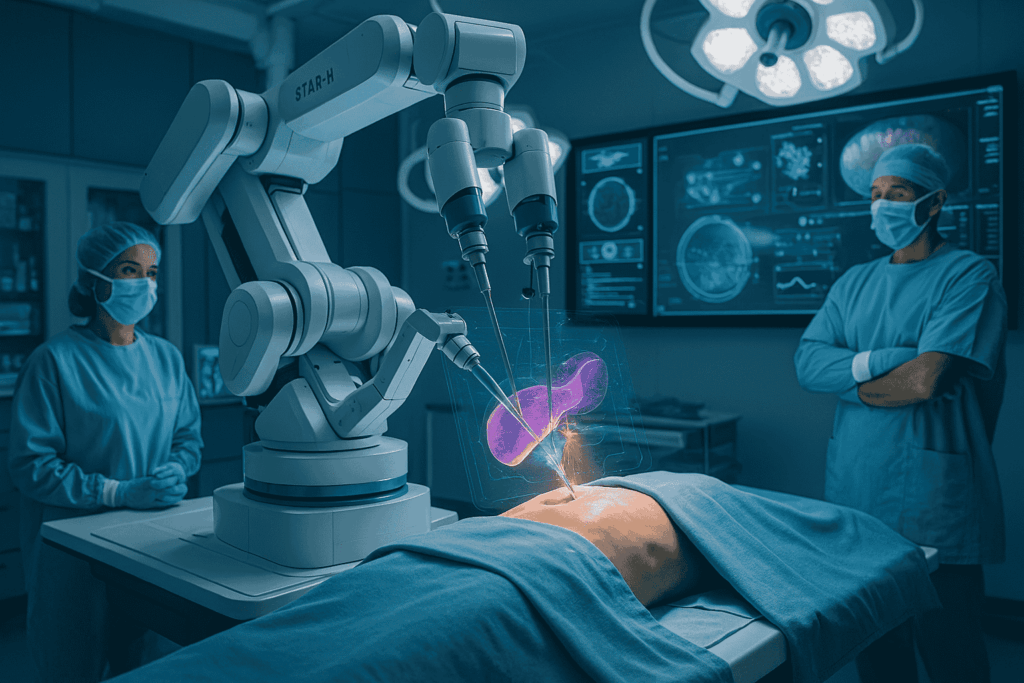
True autonomous surgery requires the machine to perform intraoperative decision-making. We have seen glimpses of this in research settings. For example, the Smart Tissue Autonomous Robot (STAR) developed at Johns Hopkins University has successfully performed soft-tissue suturing in pigs with more consistency than human surgeons. These milestones prove that surgical precision is a solved problem.
However, a pig’s intestine in a controlled lab is not a human patient in a chaotic operating room. In a real-world scenario, a surgeon must account for “out-of-distribution” data—anomalies the AI wasn’t trained on. This includes variations in patient anatomy, the presence of dense scar tissue from previous surgeries, or the subtle change in tissue color that signals a lack of perfusion.
The Biology of Unpredictability
As a physician, I can advise you that no two bodies are the same. A gallbladder removal in a 25-year-old athlete is a fundamentally different operation than the same procedure in an 80-year-old with advanced diabetes and cardiovascular disease. The tissue is more fragile, the anatomy is often shifted by age or disease, and the risk of sudden complications is exponentially higher.

Autonomous systems currently struggle with haptic feedback—the “perceive” of the tissue. A surgeon knows by the resistance of the scalpel or the tension of the suture whether a vessel is healthy or about to rupture. Translating this tactile intuition into machine learning algorithms requires sensors and processing speeds that do not yet exist at a clinical scale.
Beyond the physical, there is the cognitive load of surgery. When a complication occurs, a surgeon doesn’t just follow a script; they synthesize years of training, the specific history of the patient, and the immediate visual evidence to develop a judgment call. This level of adaptability is what separates a technician from an expert surgeon.
The Regulatory and Ethical Wall
Even if the technology were ready tomorrow, the FDA medical device approval process is designed to move slowly for a reason. For a fully autonomous robot to be cleared for general use, it would need to undergo massive, multi-year clinical trials to prove it is not only as safe as a human but superior in a statistically significant way.
This brings us to the question of medical liability. If a teleoperated robot makes a mistake, the responsibility lies with the surgeon. If a fully autonomous robot causes a fatal injury, who is liable? The software developer? The hospital? The manufacturer? Our current legal frameworks are entirely unprepared for “algorithmic malpractice.”
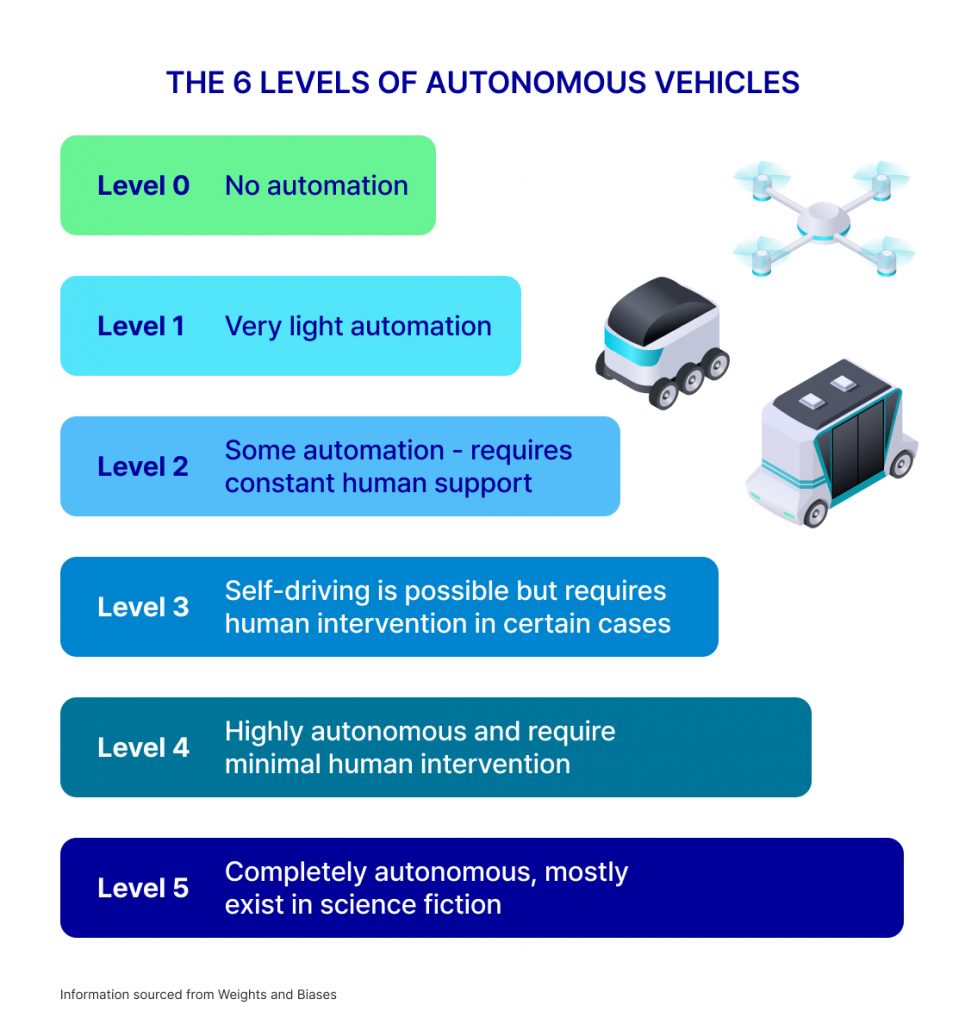
| Level | Type | Role of Surgeon | Decision Making |
|---|---|---|---|
| Level 0-1 | Teleoperated | Full Control | 100% Human |
| Level 2-3 | Semi-Autonomous | Supervisor | Shared/Collaborative |
| Level 4-5 | Fully Autonomous | Observer | 100% AI |
The Realistic Path Forward: Co-pilots, Not Pilots
The future of the autonomous surgery timeline is likely not the replacement of the surgeon, but the evolution of the “surgical co-pilot.” We are moving toward a hybrid model where AI handles the tedious, repetitive tasks—such as closing a long incision or maintaining a clear field of view—while the surgeon focuses on the critical, high-stakes portions of the operation.
This augmented approach leverages the strengths of both: the tireless precision of machine learning and the nuanced judgment of human expertise. By integrating real-time data from medical research journals and live imaging, AI can alert a surgeon to a hidden artery or suggest an optimal cutting path, reducing errors without removing the human from the loop.
To suggest that this transition will happen in three years is to ignore the biological complexity of the human body and the rigorous safety standards of modern medicine. We are moving toward a future where robots make us better surgeons, but we are decades away from a world where the robot is the surgeon.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next major milestone in this field will be the results of upcoming expanded clinical trials for semi-autonomous soft-tissue systems, which are expected to provide more data on how AI handles anatomical variance in human subjects. We will continue to track these regulatory filings as they emerge.
Do you believe AI can eventually replicate surgical intuition, or will the “human touch” always be mandatory in the OR? Share your thoughts in the comments below.