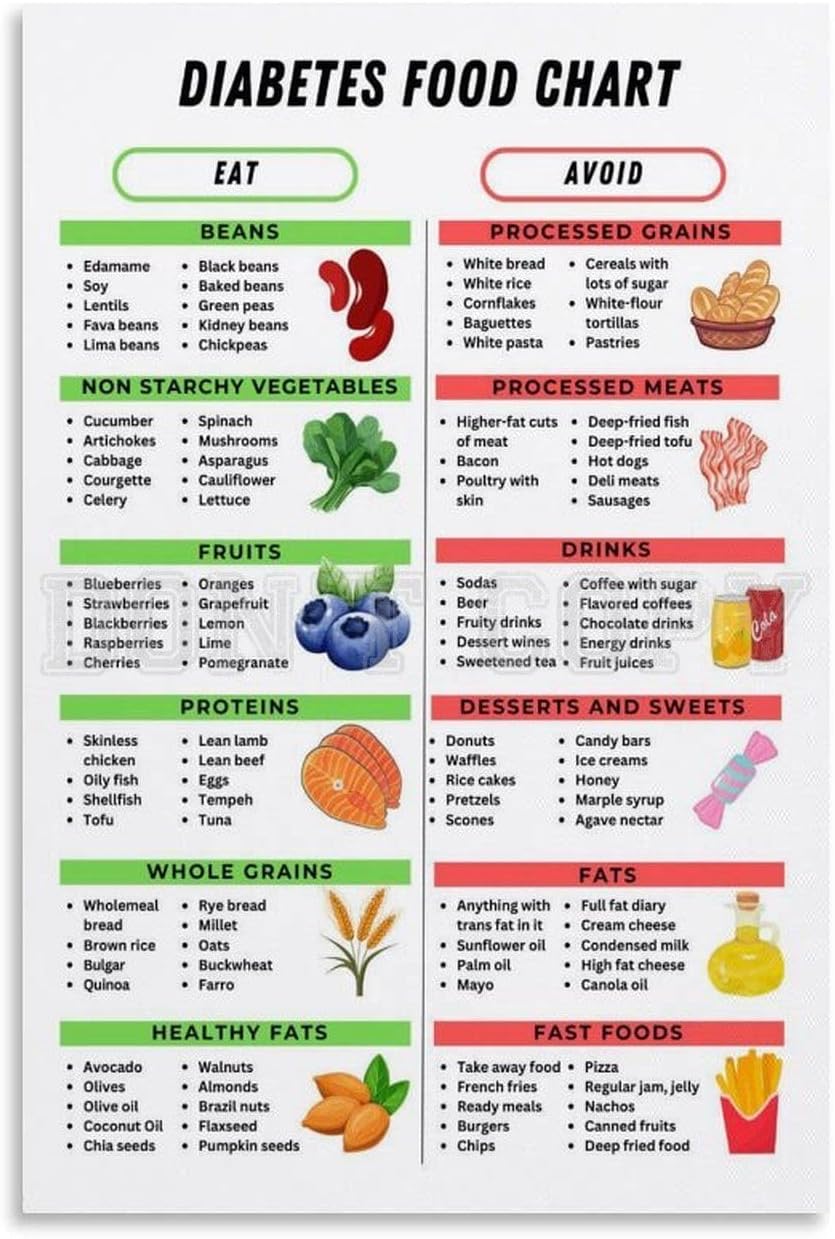
For many, the journey toward a type 2 diabetes diagnosis doesn’t begin with a sudden lifestyle collapse, but with a series of seemingly innocent dietary choices. A morning glass of orange juice, a bowl of polished white rice, or a mid-afternoon sweetened latte are staples of the modern diet, often masquerading as energy boosters or healthy starts. However, clinical evidence suggests these habits may be creating a “shortcut” to metabolic dysfunction.
Dr. Kang Hyung-chang, an internal medicine specialist and creator of the educational channel “Doctor Studying Cancer” (암 공부하는 의사 강형창), has recently sounded the alarm on specific foods that accelerate the onset of diabetes. His warnings center not just on the presence of sugar, but on the speed at which that sugar enters the bloodstream—a phenomenon known as the “glucose spike.”
As a board-certified physician, I have seen this pattern repeatedly in clinical practice. The danger lies in the invisibility of the process. Insulin resistance develops silently over years, often remaining undetected until blood glucose levels reach a critical threshold. By the time a patient receives a diagnosis, the pancreatic beta cells—responsible for producing insulin—may already be significantly fatigued.
The Danger of Liquid Calories and the ‘Glucose Spike’
One of the most critical warnings issued by Dr. Kang involves liquid sugars, particularly high-fructose corn syrup and concentrated fruit juices. While whole fruits contain fiber that slows the absorption of sugar, juicing removes this essential barrier. The result is a concentrated dose of fructose and glucose that hits the liver and bloodstream almost instantaneously.
When glucose levels spike rapidly, the pancreas is forced to secrete massive amounts of insulin to bring those levels down. Over time, the body’s cells become less responsive to this insulin. This “insulin resistance” is the physiological hallmark of pre-diabetes. Dr. Kang emphasizes that liquid sugars are particularly insidious because they do not trigger the same satiety signals in the brain as solid food, leading to overconsumption without a feeling of fullness.
The impact is not limited to weight gain. Rapid fluctuations in blood sugar can lead to systemic inflammation and oxidative stress, which further damage the vascular system and exacerbate the risk of cardiovascular disease—a common complication for those living with diabetes.
Identifying the ‘Worst Foods’ for Metabolic Health
While many people associate diabetes solely with candy and cake, Dr. Kang points to “hidden” culprits that are often integrated into traditional or perceived-healthy diets. Refined carbohydrates—those stripped of their bran and germ—behave similarly to pure sugar once digested.

White rice, white bread and flour-based noodles are prime examples. These refined grains have a high glycemic index (GI), meaning they are broken down quickly into glucose. In a typical high-carb meal, the bloodstream is flooded with sugar, triggering the cycle of insulin spikes and subsequent crashes, which often leaves the individual feeling hungry again shortly after eating.
| Food Category | Absorption Speed | Insulin Response | Metabolic Impact |
|---|---|---|---|
| Liquid Sugars (Juice/Soda) | Rapid | Extreme Spike | High risk of insulin resistance |
| Refined Carbs (White Rice/Bread) | Fast | Significant Spike | Promotes fat storage and hunger |
| Whole Grains/Fiber-rich Veggies | Slow | Gradual Rise | Stabilizes blood sugar levels |
| Proteins and Healthy Fats | Very Slow | Minimal/Stable | Supports satiety and muscle mass |
The Strategy of ‘Eating Order’ to Mitigate Risk
Beyond simply avoiding “worst foods,” Dr. Kang and other metabolic health experts suggest that how we eat is as important as what we eat. The sequence of food consumption can significantly alter the postprandial (after-meal) glucose response.
The recommended sequence is: Fiber $\rightarrow$ Protein/Fat $\rightarrow$ Carbohydrates.
- Fiber First: Starting a meal with a salad or steamed vegetables creates a “mesh” in the small intestine. This fiber layer slows down the absorption of glucose from the carbohydrates that follow.
- Protein and Fats Second: Consuming proteins (fish, meat, tofu) and healthy fats next further slows gastric emptying, ensuring that sugar enters the bloodstream at a manageable pace.
- Carbohydrates Last: By the time the white rice or bread is consumed, the presence of fiber and protein prevents the sharp glucose spike that would occur if these foods were eaten on an empty stomach.
This simple shift in habit can reduce the burden on the pancreas and help maintain a more stable energy level throughout the day, effectively turning a “shortcut to diabetes” into a pathway toward metabolic stability.
The Broader Impact: Why Metabolic Health Matters
Diabetes is rarely an isolated condition. It is often the centerpiece of metabolic syndrome, a cluster of conditions including hypertension, high triglycerides, and abdominal obesity. When the body loses its ability to regulate glucose, it affects every organ system. Chronic hyperglycemia damages the small blood vessels in the kidneys (nephropathy), the nerves (neuropathy), and the retina (retinopathy).

For those at risk, the focus should not be on restrictive dieting—which often leads to unsustainable cycles of bingeing—but on stabilizing the glycemic curve. This involves replacing liquid sugars with water or unsweetened tea, swapping refined grains for whole grains like brown rice or quinoa, and prioritizing a vegetable-forward plate.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As healthcare shifts toward personalized nutrition, the next major checkpoint for diabetes prevention will likely be the widespread adoption of Continuous Glucose Monitors (CGMs) for non-diabetics. These devices allow individuals to see in real-time how specific foods—like the “worst foods” mentioned by Dr. Kang—affect their unique biology, moving the conversation from general guidelines to precise, data-driven dietary management.
Do you have a strategy for managing your blood sugar, or a “healthy” food you discovered was actually a sugar trap? Share your experience in the comments below.