For decades, managing systemic lupus erythematosus (SLE) has felt less like a precise science and more like a high-stakes balancing act. Physicians have long navigated a narrow corridor between controlling a volatile immune system and avoiding the devastating side effects of the very drugs used to tame it. For patients, this often means a lifelong reliance on corticosteroids—medications that can save a life during a flare but erode bone density and disrupt metabolic health over time.
The frustration within the rheumatology community stems from a stark reality: the therapeutic landscape for SLE has remained remarkably stagnant. While other autoimmune conditions have seen a surge of targeted biologics, SLE patients have had very few new options since the 1950s. Until recently, the “gold standard” remained a blunt instrument of broad immunosuppression, leaving many patients to suffer from persistent organ damage despite aggressive treatment.
However, a new candidate is entering the conversation. Enpatoran, a small-molecule inhibitor targeting the sphingosine-1-phosphate (S1P) receptor, represents a potential shift in how we approach this heterogeneous disease. Rather than simply suppressing the immune system or neutralizing a single cytokine, enpatoran aims to physically sequester the problematic cells that drive lupus inflammation, potentially offering a “steroid-sparing” alternative that could redefine the standard of care.
The Long Stagnation of Lupus Care
SLE is notoriously difficult to treat because it is not a single disease, but a spectrum. One patient may present with severe lupus nephritis (kidney inflammation), while another struggles with neuropsychiatric lupus or profound hematologic issues. This clinical heterogeneity means that a drug that works for one person may do nothing for another.
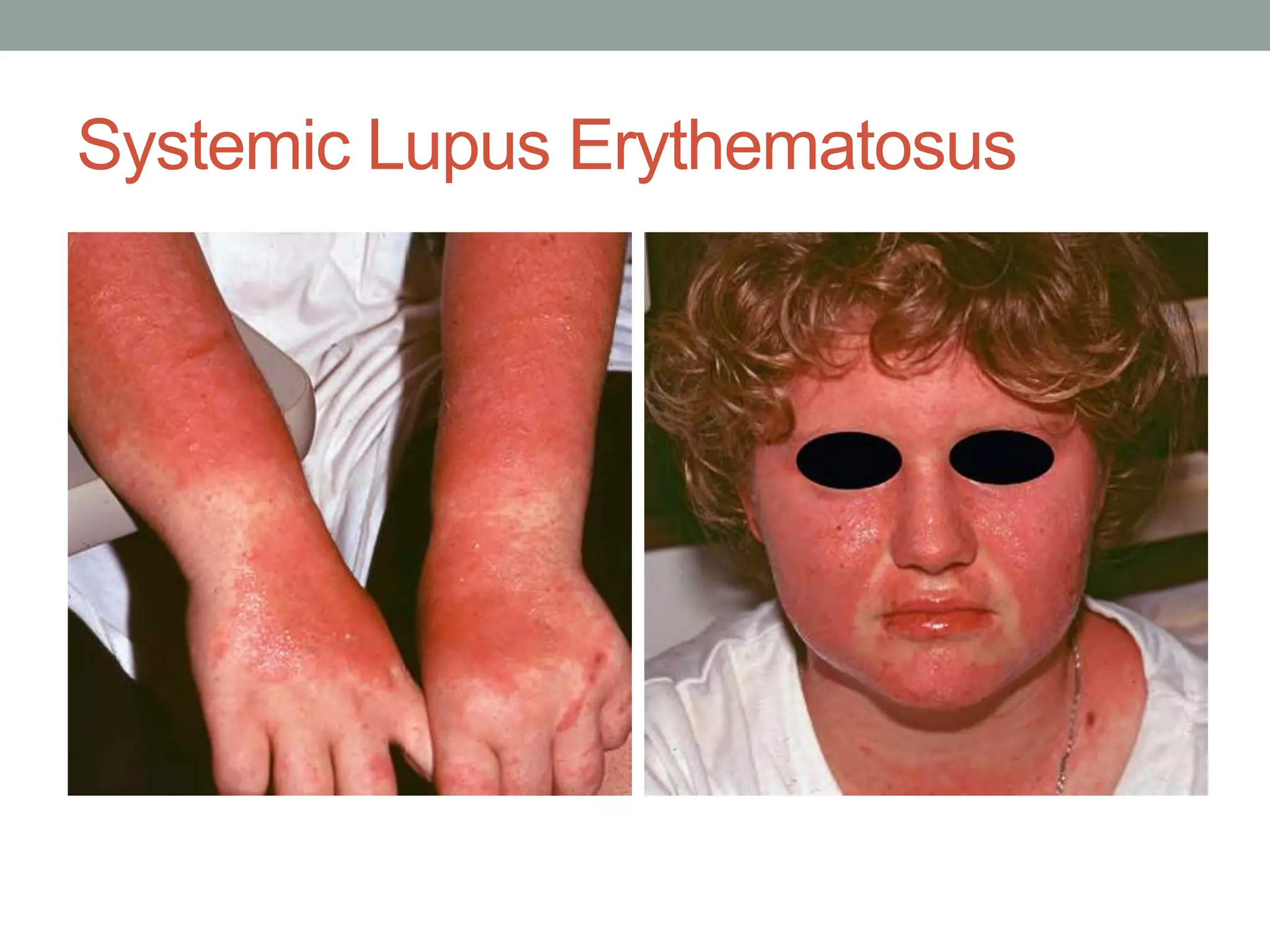
For over half a century, the primary tools were hydroxychloroquine and corticosteroids. While effective, steroids are “double-edged swords.” Long-term use is linked to cataracts, hypertension, and an increased risk of opportunistic infections. The goal of modern rheumatology is not just remission, but steroid-sparing remission—achieving stability while tapering the patient off prednisone.
In recent years, two major breakthroughs arrived: belimumab, which targets B-cell activating factor (BAFF), and anifrolumab, which blocks the type-1 interferon receptor. While these biologics have provided a lifeline for many, they are not panaceas. They are often insufficient as monotherapies, carry high costs, and have limited availability in many parts of the world. The need for an oral, targeted, and accessible therapy remains acute.
Enter Enpatoran: A New Mechanism of Action
Enpatoran operates on a fundamentally different principle than previous biologics. Instead of targeting a specific protein or receptor on the surface of an immune cell to “turn it off,” enpatoran targets the movement of the cells themselves.
The drug is an S1P1 receptor modulator. In a healthy immune system, lymphocytes (white blood cells) reside in the lymph nodes and only exit into the bloodstream when they receive a specific signal via the S1P receptor. In SLE, autoreactive lymphocytes—the “rogue” cells that attack the body’s own tissues—leak into the circulation and infiltrate organs like the kidneys and skin, causing inflammation and permanent scarring.
Enpatoran essentially creates a “traffic jam” within the lymph nodes. By modulating the S1P1 receptor, it prevents these autoreactive lymphocytes from exiting the lymph nodes and entering the blood. By sequestering the “army” of inflammatory cells before they can reach the target organs, enpatoran aims to reduce the systemic inflammatory load without the broad-spectrum toxicity associated with traditional chemotherapy-based immunosuppressants.
| Therapy | Primary Target | Route | Primary Goal |
|---|---|---|---|
| Belimumab | BAFF / BLyS | IV / Subcutaneous | B-cell survival inhibition |
| Anifrolumab | Type-1 IFN Receptor | IV | Interferon signaling blockade |
| Enpatoran | S1P1 Receptor | Oral | Lymphocyte sequestration |
| Corticosteroids | Glucocorticoid Receptor | Oral / IV | Broad anti-inflammatory |
Moving Beyond Steroid Dependency
The true value of enpatoran lies in its potential to reduce the “steroid burden.” Because it targets a different pathway than current biologics, there is a theoretical possibility that it could be used in combination with other therapies to achieve deeper remission.
For the patient, the shift from an intravenous infusion (required for anifrolumab or belimumab) to a daily oral pill is more than a matter of convenience; it is a matter of quality of life. Oral therapies lower the barrier to access, particularly for patients in rural areas or those with limited insurance coverage. If enpatoran can prove that it maintains efficacy while allowing clinicians to aggressively taper steroids, it would address the single greatest unmet need in SLE management.
However, S1P modulators are not without risks. In other autoimmune contexts, such as multiple sclerosis, S1P inhibitors have been associated with bradycardia (slow heart rate) and macular edema. The challenge for enpatoran will be demonstrating a safety profile that is favorable enough to justify its use in a population that may already have compromised organ function.
The Path to Clinical Integration
As enpatoran moves through the clinical trial pipeline, the medical community is looking for specific markers of success. The primary question is no longer just “Does it work?” but “For whom does it work best?” Given the heterogeneity of SLE, researchers are analyzing biomarkers to determine if certain subsets of patients—perhaps those with high lymphocyte counts or specific organ involvement—respond more favorably to S1P modulation.
The transition from broad immunosuppression to precision medicine is slow, but the introduction of a small-molecule oral agent like enpatoran suggests the “therapeutic ceiling” for lupus is finally beginning to lift. If the data holds, the “toolbox” for SLE will expand from a few blunt instruments to a set of precision tools tailored to the individual patient’s pathology.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should consult with a board-certified rheumatologist regarding treatment options for systemic lupus erythematosus.
The next major milestone for enpatoran will be the release of comprehensive Phase 2/3 clinical data, which will determine its viability for regulatory filing and subsequent FDA review. These results will clarify whether S1P modulation is a sustainable long-term strategy for SLE patients.
Do you or a loved one live with SLE? We want to hear your thoughts on the evolution of lupus treatments. Share your experience in the comments or share this article with your healthcare community.

