In the quiet of a pediatric exam room, a conversation that once felt routine has grow an emotional tightrope. For many parents, the act of scheduling childhood immunizations is no longer a simple checklist of preventative care, but a high-stakes navigation of conflicting data, viral headlines, and an overwhelming sense of responsibility.
This shift represents a broader vaccine trust among parents crisis that is redefining the relationship between families and their physicians. While the overarching goal remains the same—the health and safety of the child—the path to reaching that goal is increasingly obstructed by a digital landscape where raw studies trend on social media long before clinical peer review can provide necessary context.
As a physician, I see this tension daily. Clinicians are trained to interpret evidence, weigh statistical risks, and translate scientific uncertainty into actionable advice. Parents, yet, are often forced to navigate that same uncertainty without the professional infrastructure of medical training, relying instead on algorithmic feeds that prioritize engagement over accuracy.
The Nuance of Vaccine Confidence
One of the most critical misunderstandings in the current public health discourse is the idea that vaccine hesitancy is a binary state. Trust is not a single, monolithic construct. rather, it is vaccine-specific and highly context-dependent.
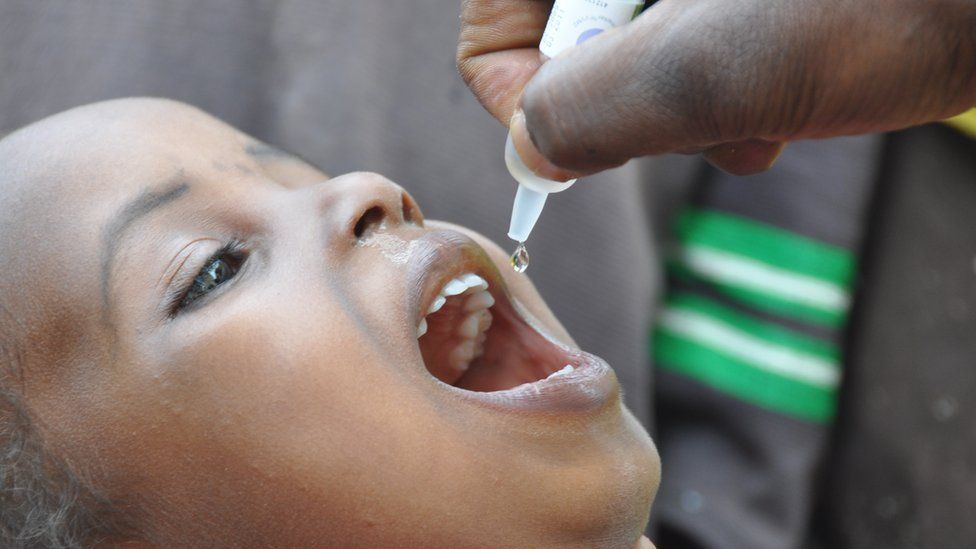
Data suggests that confidence remains robust for longstanding, “legacy” immunizations. According to research from the Kaiser Family Foundation (KFF), a significant majority of parents continue to view routine childhood vaccines—such as those for Polio and Measles, Mumps, and Rubella (MMR)—as essential for community health and safe for their children.
However, this confidence fractures when applied to newer or more frequently updated vaccines. Trust in the influenza and COVID-19 vaccines remains more divided. For many families, the rapid development and evolving recommendations surrounding the COVID-19 pandemic created a perception of instability, leading some to question the necessity of these specific shots for children even while they maintain faith in the traditional schedule.
Comparing Trust Levels Across Vaccine Types
| Vaccine Category | General Trust Level | Primary Driver of Hesitancy |
|---|---|---|
| Legacy (MMR, Polio) | High | Rare; typically linked to specific misinformation |
| Seasonal (Influenza) | Moderate | Perceived low efficacy or annual burden |
| Recent (COVID-19) | Divided | Rapid rollout and evolving guidance |
The Gap Between Evidence and Interpretation
The friction in the exam room often stems from a disparity in how information is consumed. In a medical setting, a new study is vetted for methodology, sample size, and conflict of interest. In the digital sphere, a single outlier result or a misinterpreted abstract can be amplified millions of times, creating a “truth effect” through sheer repetition.
This creates a profound vulnerability for parents in medicine and the general public alike. When recommendations evolve—as they naturally do in science—it can be misinterpreted as a sign of failure or dishonesty rather than a sign of progress. The emotional burden of responsibility weighs heavily on parents; the fear of making the “wrong” choice often outweighs the statistical fear of the disease itself.
This environment transforms the physician’s role from a provider of information to a curator of truth. The challenge is to move away from an adversarial framework—where “hesitant” parents are pitted against “pro-vaccine” clinicians—and toward a collaborative model based on shared goals.
Navigating Evolving Public Health Guidelines
The landscape is further complicated when official guidance appears to shift. The Centers for Disease Control and Prevention (CDC) and the American Academy of Pediatrics (AAP) work closely to establish immunization schedules, but nuances in how these recommendations are communicated or scheduled can lead to confusion.
When scheduling differences occur or when the timing of a booster is adjusted, it can inadvertently fuel skepticism. To a clinician, a schedule adjustment is a refinement based on new data; to a parent scrolling through a forum, it may look like a contradiction.
To bridge this gap, healthcare providers are increasingly focusing on “motivational interviewing”—a technique that prioritizes listening to a parent’s specific fears without judgment before introducing evidence. By acknowledging the emotional weight of the decision, physicians can rebuild the trust necessary to ensure children receive the protection they necessitate.
The Path Toward Community Immunity
The goal of these conversations is not simply to achieve a signature on a consent form, but to restore the social contract of community immunity. When vaccine trust erodes, the risk is not limited to the individual child but extends to the most vulnerable members of the population who cannot be vaccinated for medical reasons.

Restoring this trust requires a multi-pronged approach: clearer communication from public health agencies, a commitment to transparency regarding side effects and risks, and a shift in the clinical approach toward empathy and patience.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or vaccination schedule.
The next critical checkpoint for vaccine trust will be the release of updated seasonal guidance and the ongoing review of pediatric booster efficacy for the coming year. As these updates are integrated into clinical practice, the focus will remain on how to communicate these changes without triggering further skepticism.
We want to hear from you. How have your conversations about vaccinations changed in recent years? Share your experiences in the comments below.

