For millions of people, the arrival of GLP-1 receptor agonists like semaglutide and tirzepatide has felt like a medical miracle. These medications, which mimic hormones that regulate appetite and insulin, have rewritten the playbook for obesity treatment, allowing patients to achieve weight loss previously seen only through invasive surgery. However, a daunting reality accompanies these gains: the “rebound.” For many, the weight begins to creep back the moment the medication is discontinued, driven by a biological surge in hunger and a slowing metabolism.
This physiological tug-of-war has left clinicians searching for a way to “lock in” the progress made during GLP-1 therapy. New research highlighted by Medscape Medical News suggests a promising middle ground. By utilizing Endoscopic Sleeve Gastroplasty (ESG)—a minimally invasive procedure that reduces stomach volume without surgical incisions—patients may be able to maintain their weight loss far more effectively than through lifestyle modifications alone after stopping GLP-1 medications.
As a physician and medical writer, I have watched the narrative around obesity shift from a focus on “willpower” to a recognition of complex endocrine signaling. The challenge has always been sustainability. The integration of ESG as a secondary intervention represents a strategic shift: using pharmacology to initiate weight loss and a mechanical intervention to sustain it.
Bridging the Gap Between Medication and Maintenance
The central conflict in obesity management is the body’s homeostatic drive to return to its highest previous weight. When GLP-1 medications are stopped, the appetite suppression vanishes, and the body often aggressively signals for caloric intake to recover lost mass. While diet and exercise are the gold standards for health, they often struggle to compete with these powerful hormonal drives.

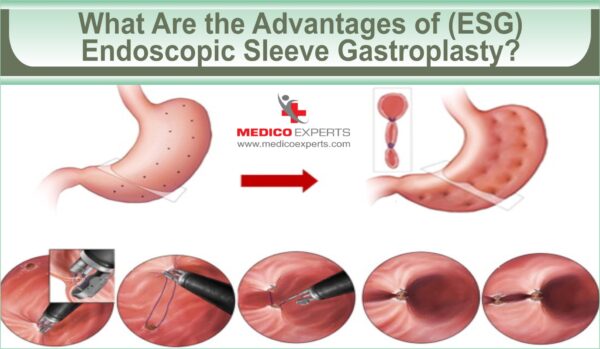
ESG offers a structural solution to this hormonal problem. Unlike a traditional sleeve gastrectomy, which involves surgically removing a large portion of the stomach, ESG is performed endoscopically. A physician inserts a flexible tube through the mouth and uses a specialized suturing device to fold the stomach into a narrow tube. This reduces the volume of the stomach, limiting the amount of food a person can consume and altering the rate of gastric emptying.
Researchers found that when this procedure is performed after a patient has already achieved significant weight loss via GLP-1s, the results are substantially more durable. At the one-year mark following the cessation of medication, those who underwent ESG showed significantly greater total weight loss compared to a control group relying solely on lifestyle changes. This suggests that the physical restriction of the stomach acts as a critical fail-safe against the return of appetite.
Comparing Weight Loss Strategies Post-GLP-1
To understand why this hybrid approach is gaining traction, it is helpful to compare the mechanisms and outcomes of the common paths patients take after stopping medication.
| Strategy | Mechanism of Action | Invasiveness | 1-Year Sustainability |
|---|---|---|---|
| Lifestyle Modification | Behavioral changes, caloric restriction | Non-invasive | Variable. high risk of regain |
| Endoscopic Sleeve (ESG) | Mechanical volume reduction (sutures) | Minimally invasive | Significantly higher weight maintenance |
| Surgical Gastrectomy | Permanent organ resection | High (Invasive) | Very high; higher risk profile |
The Clinical Implications of a Hybrid Model
The shift toward combining GLP-1s with ESG is not without its nuances. From a clinical perspective, the “sequencing” of these treatments is key. Using GLP-1s first allows patients to lose a significant amount of visceral fat, which can make the endoscopic procedure safer and easier to perform. It also allows the patient to adapt to a lower-calorie intake before the mechanical restriction of ESG is introduced.
For the patient, the appeal lies in the risk-benefit ratio. Because ESG requires no incisions, there is no scarring and the recovery time is drastically shorter than traditional bariatric surgery. This lowers the barrier to entry for patients who are terrified of the operating room but are equally terrified of regaining 50 or 100 pounds.
However, several constraints remain. ESG is not a “magic bullet” and requires a commitment to nutritional guidance to avoid deficiencies. The cost of the procedure and insurance coverage vary widely, often leaving a gap between those who can afford this “maintenance” phase and those who cannot.
Who Benefits Most from this Approach?
- The “Non-Responder” to Lifestyle: Patients who have a history of failing traditional diet and exercise programs despite strong motivation.
- The Medication-Intolerant: Those who achieved great results on GLP-1s but cannot tolerate the long-term side effects (such as severe nausea or gastric motility issues).
- The High-Risk Surgical Candidate: Individuals who would be too high-risk for a full laparoscopic gastrectomy but still require more than behavioral support.
What Remains Unknown
While the one-year data is encouraging, the medical community is still seeking long-term longitudinal data. We do not yet know if the weight maintenance provided by ESG lasts five or ten years, or if the stomach eventually stretches, necessitating further intervention. More research is needed to determine the optimal “switching point”—exactly when a patient should transition from medication to the procedure to maximize the metabolic benefit.

There is also the question of “metabolic memory.” Some researchers are investigating whether the combination of GLP-1s and ESG actually resets the body’s weight set-point more effectively than either treatment alone, potentially altering the hormonal environment of the gut in a permanent way.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should consult with a board-certified bariatric physician or gastroenterologist to determine the safest and most effective weight management plan for their specific health needs.
The next major checkpoint for this field will be the release of expanded multi-center trial data, expected in late 2025, which will look at the five-year outcomes of patients using sequential GLP-1 and ESG therapy. These findings will likely influence whether insurance providers begin to categorize ESG as a standard “maintenance” tool for obesity.
Do you think a combination of medication and minimally invasive procedures is the future of weight loss? Share your thoughts in the comments or share this article with someone navigating these options.