A cluster of hantavirus infections aboard the MV Hondius cruise ship has left three people dead and several others fighting for their lives, triggering a specialized public health response across Europe and North America. Among the infected is a French national currently hospitalized in serious condition after being repatriated from the vessel, which was traveling from Ushuaïa, Argentina, to Cape Verde.
While the situation has sparked anxiety—with some drawing parallels to the early days of the Covid-19 pandemic—health authorities are emphasizing that the biological behavior of this virus is fundamentally different. For those seeking to understand the Andes hantavirus symptoms and transmission, the current outbreak highlights a rare and dangerous exception to how these viruses typically operate in nature.
The outbreak has been identified as the Andes strain, a specific variant of the hantavirus family. While most hantaviruses are transmitted exclusively from rodents to humans, the Andes strain is the only known version capable of human-to-human transmission. This capability, combined with a high case fatality rate, has led to the isolation of passengers and crew as the ship makes its way toward Rotterdam.
The Clinical Profile of the Andes Strain
To understand the risk, it is first necessary to distinguish the Andes virus from other rodent-borne pathogens. Typically, hantaviruses are contracted by inhaling aerosolized droppings or urine from infected rodents. However, the Andes strain can spread through close, prolonged contact between people, likely via respiratory droplets or direct contact.
The progression of the disease is often deceptive. The incubation period—the time between exposure and the first sign of illness—averages two weeks but can extend up to six weeks. This long window creates a challenge for contact tracing, as individuals may travel long distances before realizing they are ill.
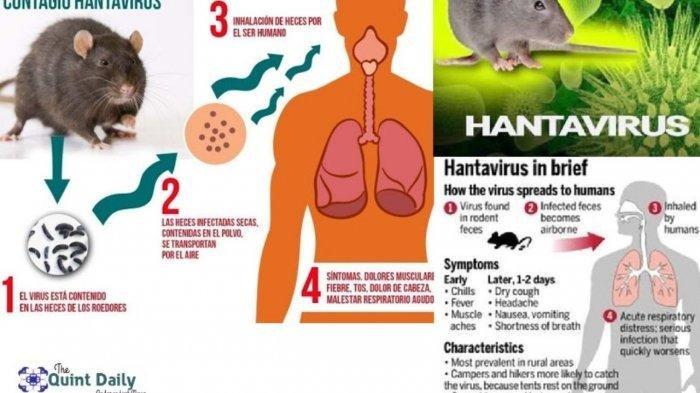
From a clinical perspective, the illness typically evolves in stages. It begins with non-specific, flu-like symptoms: fatigue, fever, and muscle aches. In some cases, patients may experience digestive issues. However, this initial phase can rapidly transition into Hantavirus Pulmonary Syndrome (HPS), characterized by severe respiratory distress and cardiac failure. According to data from the Centers for Disease Control and Prevention (CDC), the lethality of this pulmonary form is high, with some estimates reaching 60%, though the average for the Andes strain is approximately 32%.
In the specific case of the MV Hondius cluster, the current lethality rate stands at just over 30%, with three deaths recorded among ten identified cases.
Current Containment and Global Risk
The international response has been swift, focusing on breaking the chains of transmission through strict isolation. In France, one confirmed case has been reported, while 22 contact cases remain in hospital isolation. In the United States, the CDC is currently monitoring 41 individuals, including passengers and their close contacts who may have been exposed during flights.
Despite the severity of the individual cases, the broader risk to the general public remains low. The European Centre for Disease Prevention and Control (ECDC) has reaffirmed that the risk to the general European population is very low, noting that there is no evidence the virus has mutated to become more contagious than the known Andes strain.
| Metric | Andes Hantavirus Detail |
|---|---|
| Incubation Period | 2 to 6 weeks |
| Primary Transmission | Rodents; Human-to-human (Andes strain) |
| Average Lethality | 32% (can reach 60% in pulmonary form) |
| Primary Diagnosis | PCR and Serological tests |
Treatment and Diagnostic Challenges
One of the most concerning aspects of hantavirus is the lack of a specific antiviral cure or preventative vaccine. Treatment is entirely symptomatic, meaning doctors focus on supporting the patient’s vital organs—often through mechanical ventilation and cardiovascular support—while the body fights the virus.
Early detection is the only way to improve outcomes. Health professionals utilize two primary diagnostic tools: PCR tests, which detect the presence of the virus’s genetic material, and serological tests, which identify antibodies produced by the immune system in response to the infection.
Because the virus is not as easily transmissible as respiratory viruses like SARS-CoV-2, experts like infectiologist Xavier Lescure have noted that transmission likely requires “close and prolonged” contact. This makes the environment of a cruise ship a particular risk factor, though it also means the virus is less likely to trigger a widespread community epidemic.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult a healthcare professional for diagnosis or treatment of any health condition.
The next critical checkpoint will occur on Monday, May 18, when the MV Hondius is scheduled to arrive in Rotterdam. Health authorities will continue to monitor repatriated passengers and crew members over the coming weeks to ensure no new cases emerge following the long incubation period.
We invite you to share this report and leave your questions in the comments section below to help us further our coverage of this public health event.

