For many, high cholesterol is a quiet concern discussed during an annual physical, managed with a daily pill or a shift in diet. But for some, an extreme surge in blood fats can trigger a violent and life-threatening systemic collapse. What we have is the reality of acute necrotizing pancreatitis due to hypertriglyceridemia, a severe form of pancreatic inflammation where the organ begins to digest itself due to dangerously high levels of triglycerides.
The condition transforms a metabolic imbalance into a surgical emergency. Unlike standard pancreatitis, which may be caused by gallstones or alcohol, this specific variant is driven by “lipemic” blood—blood so saturated with fats that it can become milky in appearance. When triglyceride levels climb, typically above 1,000 mg/dL, the risk of acute pancreatitis increases sharply, potentially leading to necrosis, or the death of pancreatic tissue.
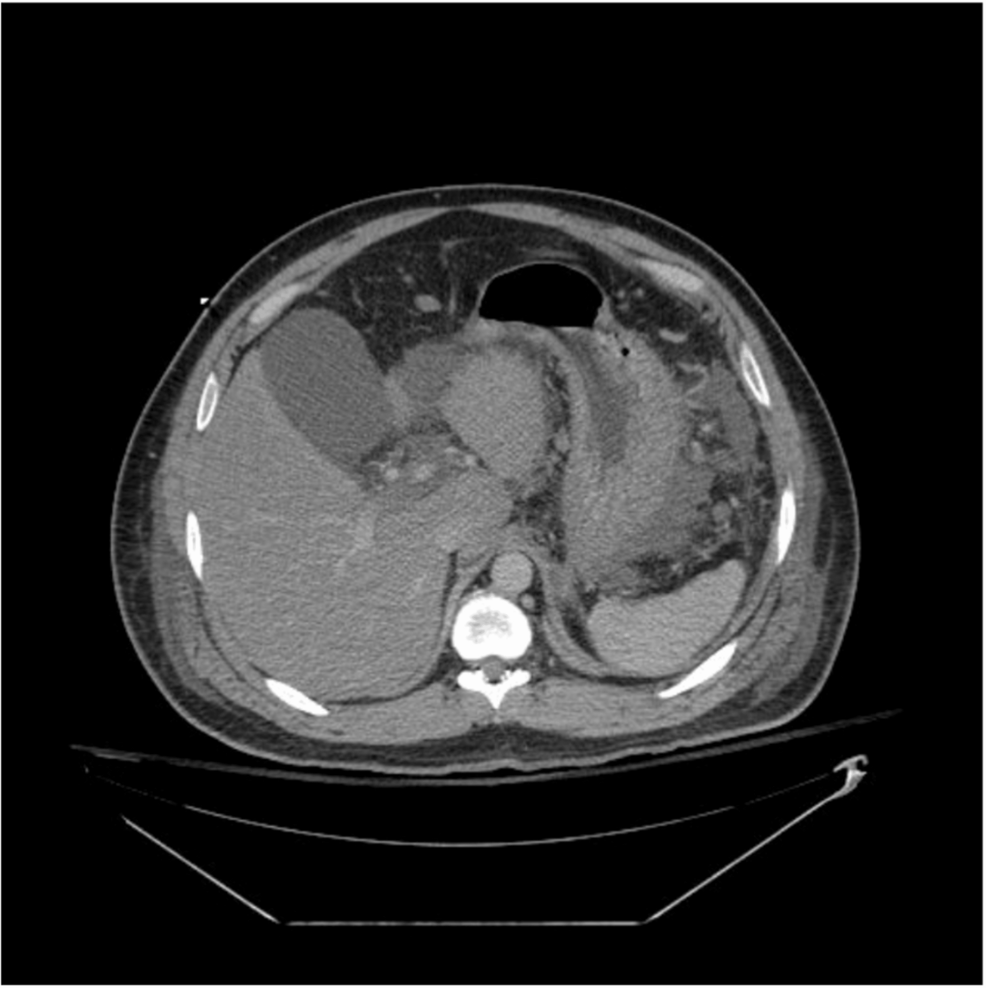
A recent clinical case highlights the volatility of this condition. A patient presented with the classic hallmarks of the disease: excruciating epigastric pain radiating to the back, accompanied by nausea and vomiting. While the symptoms mirrored common gallbladder issues, blood work revealed a critical metabolic crisis. The diagnosis of necrotizing pancreatitis meant that the inflammation had progressed beyond simple swelling, causing portions of the pancreas to die, which significantly increases the risk of secondary infections and organ failure.
The Biological Trigger: How Fat Becomes Toxic
To understand why hypertriglyceridemia leads to organ death, one must look at how the body processes lipids. Triglycerides are normally transported in the blood via lipoproteins. However, when these levels reach critical heights, the enzyme lipase—which the pancreas produces to help digest fats—begins to break down these triglycerides within the pancreatic capillaries.

This process releases an overwhelming amount of free fatty acids. These acids are toxic to the lining of the blood vessels and the pancreatic cells themselves. The resulting chemical burn causes capillary damage, restricts blood flow (ischemia) and triggers a massive inflammatory response. As the tissue dies, it creates a fertile ground for bacteria, which can lead to infected necrosis—a complication with a high mortality rate.
Medical professionals categorize the severity of the condition based on the extent of the necrosis. In the reported case, the patient’s condition required aggressive intervention to stop the inflammatory cascade and mechanically clear the blood of the offending fats.
Critical Lipid Thresholds and Risk Levels
While most adults maintain triglyceride levels well below 150 mg/dL, those with genetic predispositions or uncontrolled metabolic diseases can drift into dangerous territory. The following table outlines the general clinical thresholds for triglyceride levels and their associated risks.
| Category | Triglyceride Level (mg/dL) | Primary Clinical Risk |
|---|---|---|
| Normal | Less than 150 | Low risk |
| Borderline High | 150 – 199 | Increased cardiovascular risk |
| High | 200 – 499 | Elevated metabolic risk |
| Very High/Critical | Above 500 (Critical >1,000) | Acute Pancreatitis/Necrosis |
The Race to Stabilize: Treatment Strategies
Treating acute necrotizing pancreatitis due to hypertriglyceridemia is a race against time. The primary goal is to lower the serum triglyceride levels as quickly as possible to prevent further necrosis. Depending on the patient’s stability, physicians typically employ one of three primary strategies.
- Insulin Infusions: In patients with diabetes or those who are hemodynamically stable, intravenous insulin is used. Insulin activates lipoprotein lipase, an enzyme that clears triglycerides from the blood.
- Plasmapheresis: For the most critical cases, doctors use “blood filtering” or therapeutic plasma exchange. This process physically removes the excess lipids from the bloodstream, providing the fastest possible reduction in triglyceride levels.
- Conservative Management: This includes strict “nothing by mouth” (NPO) status to let the pancreas rest, aggressive intravenous hydration, and pain management.
In the case of necrotizing pancreatitis, the challenge is doubled. Doctors must not only lower the lipids but also monitor for “infected necrosis.” If the dead tissue becomes infected, surgical intervention or percutaneous drainage may be required to remove the necrotic debris, as antibiotics often cannot penetrate dead tissue effectively.
Identifying the Root Cause: Who Is at Risk?
Hypertriglyceridemia is rarely a standalone event; it is usually the result of an underlying trigger or a genetic blueprint. Understanding these risks is essential for preventing a recurrence, which can be just as deadly as the first episode.
Genetic factors, such as familial chylomicronemia syndrome, can cause lifelong elevations in lipids regardless of diet. However, secondary causes are more common. Uncontrolled type 2 diabetes is a leading culprit, as insulin deficiency prevents the body from clearing fats from the blood. Other contributors include chronic alcohol abuse, severe hypothyroidism, and certain medications, such as some antipsychotics or retinoids.
For the patient in the case report, the focus shifted from emergency stabilization to long-term metabolic control. This involves a stringent low-fat diet, the use of fibrates (medications specifically designed to lower triglycerides), and rigorous monitoring of blood glucose levels.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next step for patients recovering from this condition is typically a multidisciplinary follow-up involving gastroenterologists and endocrinologists to establish a permanent lipid-management plan. Ongoing surveillance of triglyceride levels is the only way to ensure that a patient does not slide back into the critical zone that triggers pancreatic failure.
Do you have questions about metabolic health or lipid management? Share this article and join the conversation in the comments below.