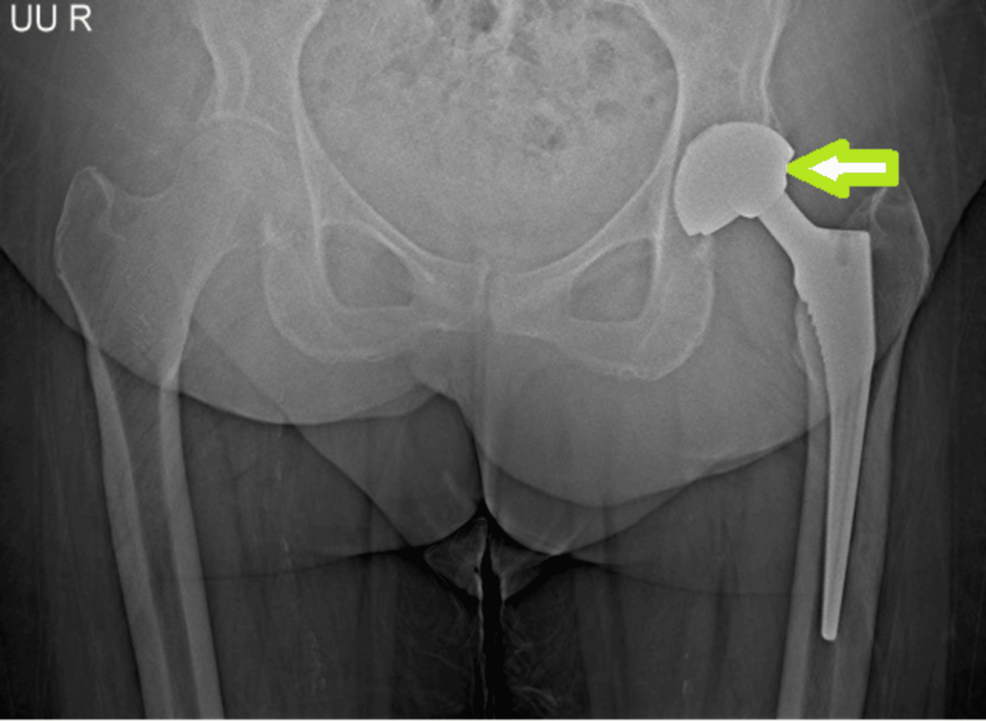
For many patients, a total hip arthroplasty is a gateway to a pain-free life, restoring mobility and independence. To further safeguard this outcome, surgeons often utilize “dual-mobility” implants—a sophisticated design specifically engineered to prevent the joint from popping out of place. However, a rare and deceptive complication known as intraprosthetic dislocation following dual-mobility total hip arthroplasty can occur, where the joint fails internally while appearing stable from the outside.
Unlike a traditional hip dislocation, where the prosthetic head completely exits the socket and causes an obvious deformity of the leg, an intraprosthetic dislocation is a “hidden” failure. In these cases, the smaller internal head of the prosthesis dislocates from its inner liner but remains trapped within the larger outer shell. This creates a clinical paradox: the patient experiences significant pain and loss of function, yet the hip joint remains centered in the socket upon physical examination.
As a board-certified physician, I have seen how these diagnostic nuances can delay treatment. When the external markers of a dislocation are absent, clinicians may overlook the internal collapse of the implant. Recognizing the signs of this specific failure is critical to preventing further wear on the prosthetic components and ensuring the patient returns to full mobility.
The Mechanics of Dual-Mobility Implants
To understand how an internal dislocation occurs, one must first understand the architecture of a dual-mobility bearing. In a standard hip replacement, there is one articulating surface—a ball and a socket. In a dual-mobility system, there are two. A small femoral head is locked into a small polyethylene liner, which is then placed inside a larger metal or ceramic outer shell.
This “joint within a joint” design increases the range of motion and provides a secondary layer of stability. We see typically reserved for high-risk patients, such as those with neurological disorders, previous joint instability, or those undergoing complex revision surgeries. The goal is to provide a wider “jump distance,” making it significantly harder for the joint to dislocate entirely.
However, this complexity introduces a latest failure mode. If the smaller head escapes the inner liner, it can still rotate within the larger outer shell. This allows the patient to continue moving the leg, albeit with pain and restricted range, which often masks the severity of the internal injury.
Identifying the “Hidden” Dislocation
The challenge of diagnosing intraprosthetic dislocation following dual-mobility total hip arthroplasty lies in the discrepancy between the patient’s symptoms and the physical presentation. Patients typically report a sudden onset of groin or hip pain, often following a minor trauma or even a routine movement. They may experience a “clunking” sensation or a sudden inability to rotate the leg fully.

During a physical exam, the leg usually appears to be in a normal position. There is no characteristic shortening or internal rotation typically seen in a full dislocation. Because the outer shell remains seated in the acetabulum (the pelvic socket), the hip does not “look” dislocated.
Diagnosis relies almost exclusively on high-resolution imaging. Standard X-rays are the first line of defense, but they require a keen eye to spot the slight shift in the position of the inner liner relative to the femoral head. In complex cases, a CT scan is often necessary to visualize the precise orientation of the components and determine if the head has completely exited the liner or is merely subluxated (partially dislocated).
| Feature | Standard Dislocation | Intraprosthetic Dislocation (IPD) |
|---|---|---|
| Visual Appearance | Obvious leg deformity/shortening | Normal leg alignment |
| Joint Position | Head is outside the socket | Head is inside the outer shell, outside inner liner |
| Clinical Presentation | Acute, severe instability | Pain, restricted motion, “clunking” |
| Diagnostic Method | Physical exam and X-ray | Careful X-ray analysis and CT imaging |
Treatment and Surgical Revision
Once an intraprosthetic dislocation is confirmed, the primary goal is to restore the integrity of the bearing surface. While a standard dislocation can often be “reduced” (popped back in) through manual manipulation under sedation, an internal dislocation usually requires surgical intervention. This is because the inner liner is often damaged or worn, meaning a simple reduction would likely lead to immediate re-dislocation.
The surgical approach typically involves a revision of the bearing components. The surgeon must remove the dislocated inner liner and the femoral head, inspecting the outer shell for any scratches or wear. If the outer shell is intact, a new liner and head are implanted. If the outer shell has been compromised by the displaced head, it may also need to be replaced to ensure long-term stability.
The success of the revision depends heavily on the timing of the diagnosis. If a patient continues to walk on an internally dislocated hip, the metal head can grind against the outer metal shell, leading to “metallosis”—the release of metal debris into the surrounding soft tissue. This can cause inflammation, tissue death, and a higher risk of implant loosening, which complicates the revision surgery.
Risk Factors and Long-Term Outlook
While dual-mobility implants are generally highly successful, certain factors increase the risk of internal failure. These include extreme ranges of motion, improper component positioning during the initial surgery, or significant wear of the polyethylene liner over time. Patients with high activity levels or those with underlying muscle weakness may also be more susceptible to the forces that trigger an internal pop-out.

For most patients, a timely revision leads to a full recovery of function. The American Academy of Orthopaedic Surgeons emphasizes the importance of postoperative follow-up and imaging to catch these complications early. When detected promptly, the prognosis for returning to a high quality of life is excellent.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients experiencing hip pain or instability should consult a licensed orthopedic surgeon for a proper diagnosis and treatment plan.
Medical researchers continue to analyze the long-term wear rates of various dual-mobility materials to reduce the incidence of these failures. The next major checkpoint for the orthopedic community will be the release of updated longitudinal registry data, which will help surgeons refine the patient selection process for these specific implants to further minimize the risk of internal dislocation.
Do you or a loved one have experience with hip replacement recovery? We invite you to share your thoughts or questions in the comments below.