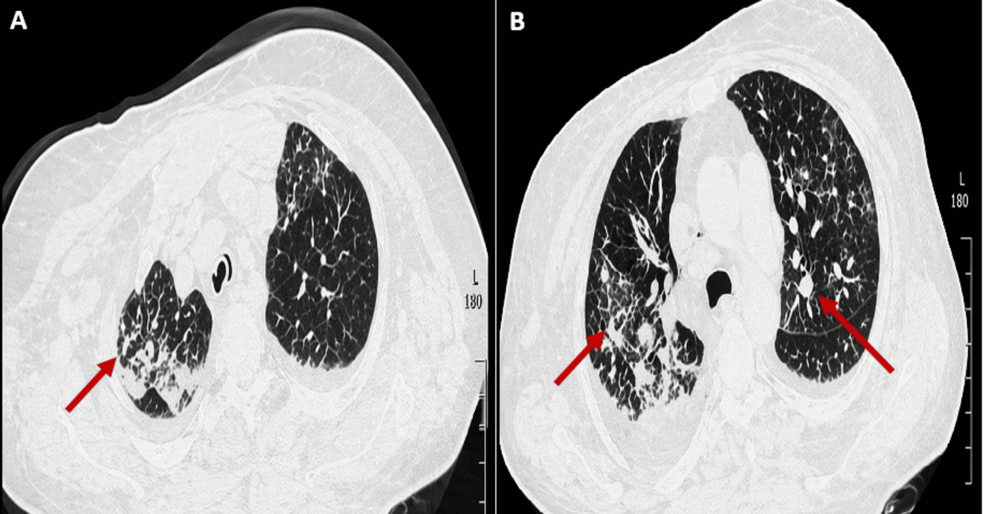
A 62-year-old man’s battle with a chronic lung condition took a perilous turn when a routine respiratory struggle evolved into a life-threatening neurological crisis. The patient, who suffered from severe bronchiectasis, presented with a sudden onset of fever and altered mental status, leading to the discovery of multiple brain abscesses associated with severe bronchiectasis and a systemic respiratory infection.
The case underscores a rare but critical medical pathway known as hematogenous spread, where bacteria from a localized infection in the lungs enter the bloodstream and migrate to distant organs. In this instance, the patient’s compromised pulmonary system served as a reservoir for pathogens that eventually breached the blood-brain barrier, creating pockets of pus within the brain tissue.
For clinicians and caregivers, the case serves as a stark reminder that in patients with chronic obstructive or inflammatory lung diseases, neurological changes should not be dismissed as simple confusion or age-related decline, but rather investigated as potential systemic complications.
From Respiratory Distress to Neurological Decline
The patient arrived at the medical facility exhibiting a classic triad of symptoms: fever, headache, and a significant shift in cognitive function. While his history of severe bronchiectasis—a condition where the bronchial tubes are permanently widened and damaged—made him prone to recurrent lung infections, the rapid onset of mental confusion suggested the infection had moved beyond the chest.
Diagnostic imaging played a pivotal role in identifying the crisis. A contrast-enhanced MRI of the brain revealed several “ring-enhancing lesions,” which are characteristic hallmarks of brain abscesses. These lesions indicate areas of inflammation and infection where the body has attempted to wall off the bacteria, creating a capsule around the infected core.
The connection between the lungs and the brain is a known, albeit infrequent, complication of severe pulmonary disease. When the lungs are severely damaged, as seen in bronchiectasis, the risk of chronic colonization by bacteria increases. If these bacteria penetrate the systemic circulation, they can seed themselves in the brain, leading to abscess formation.
The Path to Recovery: Surgery and Sustained Therapy
Managing multiple brain abscesses requires a dual-pronged approach: reducing the pressure on the brain and eliminating the underlying pathogen. Because the patient presented with multiple lesions and declining consciousness, medical teams opted for surgical intervention.
The patient underwent a craniotomy, a surgical procedure where a section of the skull is removed to allow surgeons to drain the abscesses. This immediate decompression is vital to prevent permanent brain damage or death caused by increased intracranial pressure. Following the surgery, the patient was placed on a rigorous course of long-term intravenous antibiotics tailored to the specific bacteria recovered from the abscesses.
The recovery process for such a complex infection is rarely swift. The patient required prolonged antimicrobial therapy to ensure that any remaining dormant bacteria were eradicated, preventing a relapse of the infection.
| Stage | Key Clinical Findings | Primary Intervention |
|---|---|---|
| Presentation | Fever, cough, altered mental status | Stabilization & Imaging |
| Diagnosis | Ring-enhancing lesions on MRI | Neurological Consultation |
| Acute Phase | Increased intracranial pressure | Surgical Drainage (Craniotomy) |
| Recovery | Gradual cognitive improvement | Long-term Antibiotic Course |
Understanding the Pulmonary-Brain Connection
The mechanism of hematogenous spread is a critical concept in infectious disease. In patients with severe respiratory infections, the inflammatory response can make blood vessels more permeable, allowing bacteria to leak into the bloodstream. Once in the blood, these pathogens can travel to the brain, where they may settle in areas of low blood flow or areas already damaged by previous micro-infarcts.
This specific progression—from bronchiectasis to brain abscess—is particularly dangerous because the initial symptoms of a lung flare-up can mask the early signs of neurological involvement. By the time a patient exhibits altered mental status, the infection in the brain is often already advanced.
Medical experts emphasize that the management of brain abscesses requires a multidisciplinary team, including pulmonologists, neurologists, and infectious disease specialists, to treat both the source of the infection and the secondary site of damage.
Key Risk Factors and Warning Signs
- Chronic Lung Disease: Conditions like bronchiectasis or cystic fibrosis that create a permanent environment for bacterial growth.
- Recurrent Pneumonia: Frequent respiratory infections that increase the likelihood of bacterial translocation into the blood.
- Neurological Shifts: Sudden confusion, personality changes, or focal neurological deficits in a patient with a known infection.
- Systemic Inflammation: Persistent high fever that does not respond to standard respiratory antibiotics.
Clinical Implications for Long-Term Care
This case highlights the necessity of aggressive monitoring for patients with severe pulmonary damage. The “seeding” of the brain from the lungs is a rare event, but its mortality rate is high if not caught early. The successful outcome in this patient was attributed to the rapid use of MRI imaging and the timely decision to proceed with surgical drainage.
For those living with chronic respiratory conditions, the takeaway is the importance of vigilance. Any sudden change in mental clarity or the onset of severe headaches during a respiratory flare-up should be treated as a medical emergency.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The medical community continues to monitor the long-term outcomes of patients who survive hematogenous brain seeding, with future focus on refining antibiotic protocols to prevent recurrence. The next phase of care for patients in similar conditions typically involves long-term pulmonary rehabilitation and regular neurological screenings to ensure full cognitive recovery.
Do you or a loved one manage a chronic respiratory condition? Share your experience or questions in the comments below.