For decades, emotional intelligence (EI) was relegated to the realm of “soft skills”—a nebulous blend of empathy and tact often viewed as an innate personality trait rather than a measurable competency. However, a shifting paradigm in clinical research is repositioning these abilities as a sophisticated biological process. The neuroscience of emotional intelligence reveals that the ability to perceive, understand, and manage emotions is not merely a psychological advantage but the result of complex, integrated neural circuits.
At its core, emotional intelligence relies on a dynamic dialogue between the brain’s primitive emotional centers and its advanced executive regions. This biological synergy allows individuals to navigate social complexities, regulate stress, and maintain psychological stability. By mapping the specific pathways involved, researchers are moving beyond behavioral descriptions to identify the actual “hardware” that allows some people to remain calm under pressure while others are overwhelmed by a single critical comment.
This integrative understanding suggests that EI is not a fixed trait assigned at birth. Because the brain remains plastic throughout adulthood, the neural pathways associated with emotional regulation can be strengthened through intentional practice and targeted intervention. This shift from “trait” to “skill” has profound implications for mental health treatment, leadership development, and educational frameworks.
The Biological Hardware of Emotion
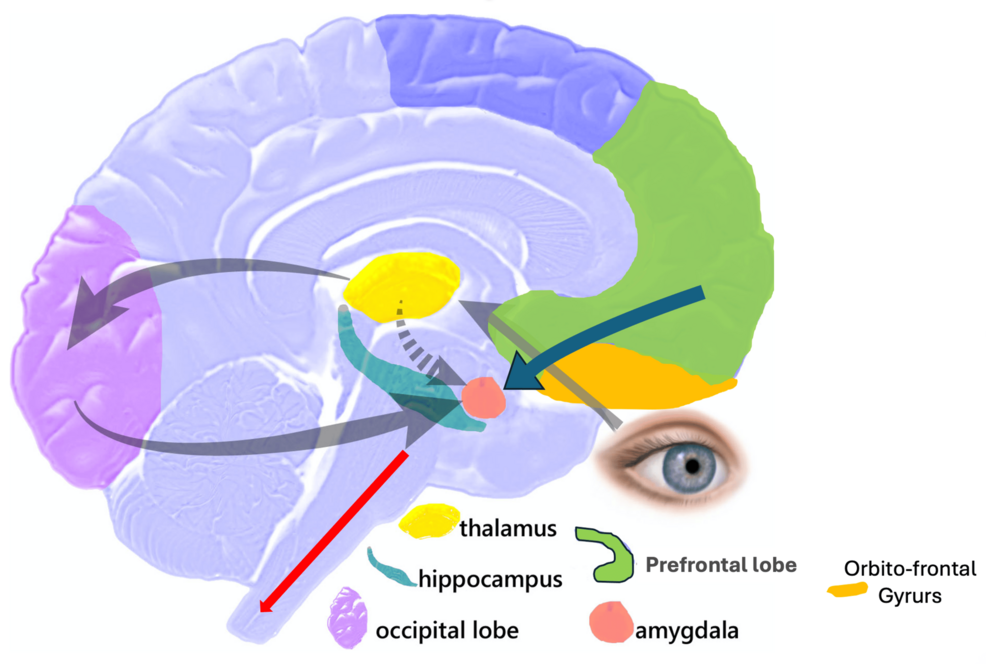
The capacity for emotional intelligence is hosted across a distributed network of brain regions, primarily involving the limbic system and the prefrontal cortex. The amygdala acts as the brain’s sentinel, scanning the environment for threats and triggering immediate emotional responses. While the amygdala is essential for survival, an overactive response—often termed “amygdala hijack”—can bypass rational thought, leading to impulsive reactions.
Counterbalancing this is the prefrontal cortex (PFC), particularly the ventromedial prefrontal cortex, which serves as the brain’s regulatory hub. The PFC evaluates the amygdala’s signals, providing the cognitive appraisal necessary to determine if a reaction is appropriate for the context. When the connection between these two regions is strong, an individual can experience a surge of anger or fear but consciously choose a measured response, a hallmark of high emotional intelligence.

Beyond the PFC and amygdala, the insula plays a critical role in interoception—the ability to sense the internal state of the body. This region allows a person to “feel” an emotion physically, such as the tightening of the chest during anxiety, before the conscious mind labels it. This physical awareness is the first step in emotional granularity, the ability to distinguish between similar emotions, such as frustration versus disappointment, which is essential for effective regulation.
| Brain Region | Primary Function | EI Application |
|---|---|---|
| Amygdala | Threat detection and emotional processing | Initial emotional response and urgency |
| Prefrontal Cortex | Executive function and impulse control | Emotional regulation and decision-making |
| Insula | Interoceptive awareness | Recognizing physical markers of emotion |
| Anterior Cingulate Cortex | Conflict monitoring and empathy | Social adjustment and perspective-taking |
The Mechanics of Emotional Regulation
The process of managing emotions occurs through two primary mechanisms: bottom-up and top-down processing. Bottom-up processing begins with the sensory input and the limbic system; It’s the raw, immediate feeling of an emotion. Top-down processing is the cognitive override where the PFC modulates that emotional response based on logic, experience, and social norms.
Effective emotional regulation is not about suppressing emotions—which often leads to increased physiological stress—but about “reappraisal.” This is the cognitive process of changing the trajectory of an emotion by altering its meaning. For example, instead of viewing a challenging work assignment as a threat to one’s competence, a person with high EI may reappraise it as an opportunity for growth. This cognitive shift actually alters the neural firing patterns, reducing the amygdala’s activation and lowering the heart rate.
The National Center for Biotechnology Information notes that these regulatory processes are deeply tied to the brain’s ability to maintain homeostasis. When the top-down regulation fails, the result is often emotional dysregulation, which is a core feature of various mood disorders and anxiety conditions.
Neuroplasticity and the Capacity for Growth
One of the most encouraging findings in modern neuroscience is the evidence of neuroplasticity—the brain’s ability to reorganize itself by forming new neural connections. This means that the circuits responsible for empathy and regulation can be “trained” much like a muscle. Social-emotional learning (SEL) programs in schools and mindfulness-based stress reduction (MBSR) in clinical settings are designed to leverage this plasticity.
Practices such as mindfulness increase the gray matter density in the prefrontal cortex while decreasing the size and reactivity of the amygdala. By repeatedly engaging in the act of observing an emotion without immediately reacting to it, individuals strengthen the inhibitory pathways from the PFC to the limbic system. This creates a wider “gap” between stimulus and response, allowing for more intentional and empathetic behavior.
This biological adaptability explains why individuals who grew up in high-stress environments with low emotional support can still develop high levels of EI in adulthood. Through therapeutic intervention and conscious effort, the brain can override early maladaptive patterns and build new, healthier pathways for social interaction and self-management.
Societal Impact and Clinical Application
The implications of understanding the biological basis of EI extend far beyond the laboratory. In healthcare, clinicians are recognizing that emotional regulation is a key determinant of patient outcomes. Patients with higher EI tend to have better adherence to treatment plans and lower rates of chronic stress-related illnesses, as they are better equipped to manage the psychological burden of disease.
In the professional sphere, the focus on “executive function” is shifting toward “emotional agility.” The ability to navigate conflict, lead diverse teams, and handle failure is now understood as a cognitive skill set that can be developed. Organizations are increasingly integrating neuroscience-backed training to improve workplace culture and reduce burnout by teaching employees how to manage their neural responses to stress.
the Harvard Health Publishing resources emphasize that the intersection of emotional and physical health is profound; chronic emotional dysregulation can lead to prolonged cortisol exposure, which impairs immune function and cognitive clarity over time.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult a licensed healthcare provider for diagnosis or treatment of mental health conditions.
As research progresses, the next major checkpoint in this field will be the integration of real-time neuroimaging with behavioral data to create personalized “emotional blueprints.” This could allow clinicians to identify exactly where a patient’s regulatory circuit is failing and apply targeted interventions—such as neurofeedback or specific cognitive exercises—to bridge that gap. The transition from understanding the brain to actively optimizing it marks the next frontier in human psychological development.
Do you believe emotional intelligence can be taught, or is it an inherent trait? Share your thoughts in the comments or share this article with your network.