A rare complication involving pacemakers, known as Reel syndrome, can lead to recurrent syncope – fainting spells – as a result of the device’s lead becoming dislodged and coiling around the pacemaker itself. While uncommon, recognizing this syndrome is crucial for timely intervention and preventing potentially life-threatening cardiac events. This condition, first described in 1968, highlights the importance of careful monitoring of pacemaker function and prompt investigation of any unusual symptoms.
The term “Reel syndrome” refers specifically to the reeling-in of pacemaker leads without damage to the leads themselves. It’s considered a variant of Twiddler’s syndrome, where patients intentionally manipulate the pacemaker or leads, but Reel syndrome occurs spontaneously. A recent case report published in the Indian Pacing Electrophysiol J details the experience of an 86-year-old woman who presented with complete AV block and a coiling ventricular lead, two years after initial pacemaker implantation. The case underscores the potential for delayed presentation of this syndrome and the need for vigilance even in patients with previously stable devices.
Understanding Pacemaker Reel Syndrome
Pacemakers are small, battery-powered devices implanted in the chest to help regulate the heartbeat. They deliver electrical impulses to the heart when the natural pacing system fails. Leads, thin insulated wires, connect the pacemaker to the heart chambers. Reel syndrome occurs when these leads migrate and coil around the pacemaker generator, disrupting its function. This can lead to a variety of symptoms, most notably syncope, but also potentially causing palpitations, dizziness, or even sudden cardiac arrest.
The exact cause of Reel syndrome isn’t fully understood. Several factors may contribute, including inadequate lead fixation, patient anatomy, and lead design. The case report from Morocco highlights the importance of considering Reel syndrome in patients presenting with unexplained pacemaker malfunction, even years after initial implantation. The authors suggest that a high index of suspicion is necessary for accurate diagnosis.
Diagnosing and Treating Reel Syndrome
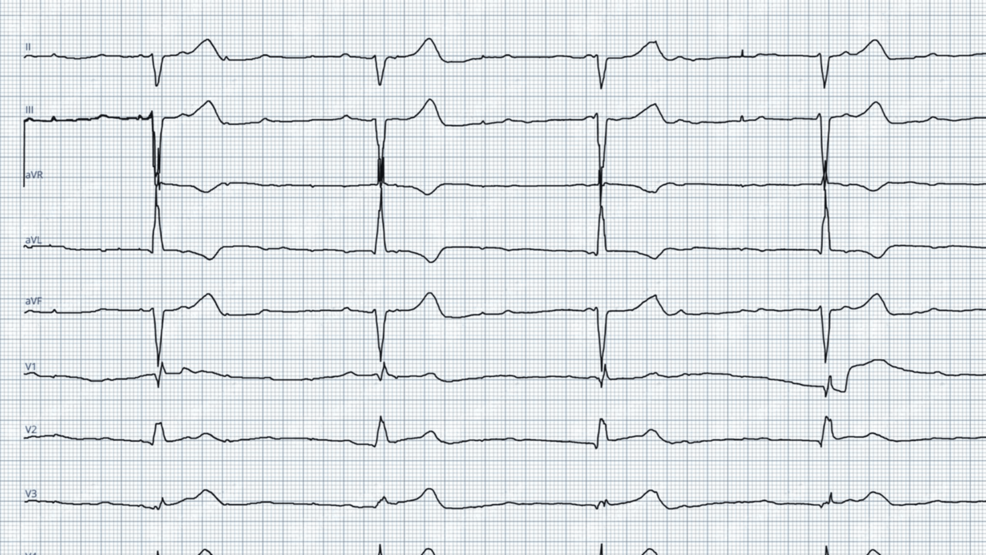
Diagnosing Reel syndrome typically involves a combination of clinical evaluation and imaging studies. A chest X-ray is often the first step, as it can reveal the coiled lead around the pacemaker. Electrocardiograms (ECGs) can present abnormalities in heart rhythm, and device interrogation can assess pacemaker function and identify lead dislodgement.
Treatment usually involves repositioning or replacing the affected lead(s). In some cases, the pacemaker generator may also need to be replaced. The approach depends on the severity of the lead displacement and the overall health of the patient. A case report published in the BMJ Case Reports in 2014 described an 82-year-old woman who experienced syncope due to atrial fibrillation and a malfunctioning pacemaker, ultimately requiring lead replacement. The report emphasizes the importance of prompt diagnosis and intervention to prevent further complications.
Recurrent Syncope as a Key Symptom
Recurrent syncope, or fainting spells, is a common presenting symptom of Reel syndrome. Syncope occurs when there is a temporary reduction in blood flow to the brain, leading to a loss of consciousness. In the context of pacemaker malfunction, syncope can be a sign that the device is not effectively regulating the heart rhythm.
It’s key to note that syncope can have many causes, so it’s not always indicative of Reel syndrome. However, in patients with pacemakers, recurrent syncope should prompt a thorough evaluation of device function. A recent article highlighted in Cureus details a case where recurrent syncope ultimately led to the diagnosis of Reel syndrome.
Looking Ahead: Continued Monitoring and Research
As the population with implanted pacemakers continues to grow, awareness of Reel syndrome is becoming increasingly important. Continued research is needed to better understand the underlying causes of this condition and to develop strategies for prevention. Regular follow-up appointments with a cardiologist, including device interrogation, are essential for monitoring pacemaker function and detecting any potential problems early on. Patients with pacemakers should also be educated about the symptoms of Reel syndrome and instructed to seek medical attention if they experience any concerning changes in their condition.
The next step in understanding and managing Reel syndrome will likely involve larger-scale studies to identify risk factors and optimize lead design. Clinicians should remain vigilant for this rare but potentially serious complication in all pacemaker patients.
Have you or a loved one experienced issues with a pacemaker? Share your thoughts and questions in the comments below. Please also share this article to raise awareness about Reel syndrome.