For most parents, a teenager with a lingering cough is a familiar frustration—a byproduct of seasonal allergies, a stubborn cold, or perhaps the early signs of asthma. But for the family of one 14-year-old boy, a chronic cough that refused to resolve became the first warning sign of an incredibly rare and aggressive malignancy: primary pulmonary Ewing sarcoma.
The case, detailed in a recent report published in the medical journal Cureus, serves as a critical reminder for clinicians and caregivers alike. It highlights the diagnostic challenge of identifying rare tumors that mimic common respiratory ailments and underscores the necessity of persistent investigation when standard treatments fail to yield results.
Ewing sarcoma is a malignant tumor that typically originates in the bones or soft tissues, most often affecting children and young adults. While it is well-known for its ability to spread to the lungs as a secondary site (metastasis), the occurrence of the cancer starting within the lung tissue itself is an extreme rarity. In this case, the patient’s presentation was deceptive, beginning not with the classic bone pain associated with the disease, but with a persistent, non-productive cough.
The Diagnostic Maze: From Common Cold to Rare Cancer
The path to diagnosis was not immediate, reflecting the deceptive nature of the disease. The patient initially presented with a chronic cough that did not respond to typical respiratory therapies. In the early stages of evaluation, a chest X-ray—the standard first line of defense for respiratory issues—appeared unremarkable. This is a common hurdle in pulmonary oncology. small or strategically located masses can often be obscured by the ribs or the heart on a two-dimensional image.
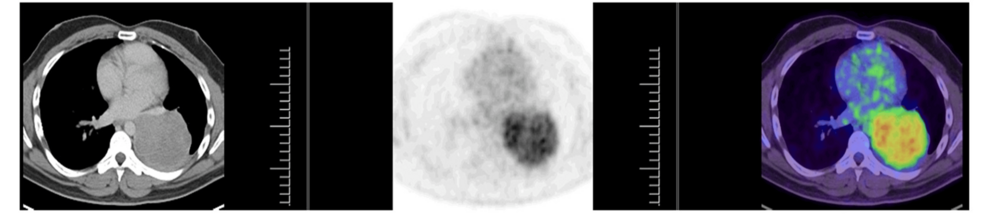
When the symptoms persisted, physicians escalated the imaging to a Computed Tomography (CT) scan. The high-resolution images revealed a starkly different picture: a significant mass in the right lung. This discovery shifted the clinical focus from an inflammatory or infectious cause to a neoplastic one, necessitating a biopsy to determine the exact nature of the growth.
The definitive diagnosis required immunohistochemistry, a process where pathologists use antibodies to identify specific proteins in the cells. The tumor cells tested positive for CD99, a cell-surface glycoprotein that is a hallmark marker for Ewing sarcoma. By confirming the absence of primary tumors in the bones or other soft tissues, the medical team was able to classify this as a primary pulmonary occurrence rather than a metastatic spread.
Primary vs. Metastatic Ewing Sarcoma
To understand the rarity of this case, it is essential to distinguish between where the cancer begins and where it travels. Most Ewing sarcoma patients are diagnosed after a lump is found in a long bone or the pelvis. For these patients, pulmonary nodules are often a sign that the cancer has already spread, which significantly alters the prognosis.
| Feature | Primary Pulmonary Ewing Sarcoma | Metastatic Ewing Sarcoma (Lung) |
|---|---|---|
| Origin | Starts in the lung parenchyma | Starts in bone or soft tissue |
| Frequency | Extremely Rare | Common progression of the disease |
| Initial Symptom | Respiratory (cough, chest pain) | Localized pain/swelling at primary site |
| Imaging | Often a single, large pulmonary mass | Often multiple bilateral nodules |
The Path to Treatment and Recovery
Once the diagnosis was confirmed, the medical team implemented a multimodal treatment strategy. Because Ewing sarcoma is highly sensitive to chemotherapy but requires the physical removal of the tumor to prevent recurrence, the approach was two-pronged.
The patient underwent a rigorous chemotherapy regimen designed to shrink the tumor and eliminate any microscopic cancer cells circulating in the bloodstream. Following the chemotherapy, surgical resection was performed to remove the primary mass from the right lung. This combination—aggressive systemic therapy followed by surgical intervention—is currently the gold standard for managing localized Ewing sarcoma.
The patient’s recovery highlights the importance of early, albeit difficult, detection. While the treatment for Ewing sarcoma is intensive, the prognosis improves significantly when the tumor is localized and can be completely resected surgically.
Clinical Implications: When to Look Deeper
For the broader medical community, this case emphasizes the “red flags” of pediatric respiratory health. While a cough is rarely a sign of sarcoma, the Cureus report suggests that clinicians should maintain a high index of suspicion when a pediatric patient presents with a chronic cough that is refractory to standard treatment and lacks a clear infectious or allergic etiology.
The case reinforces several key clinical takeaways:
- Limitations of X-rays: A clear chest X-ray does not definitively rule out a pulmonary mass in symptomatic patients.
- The Role of CT: Early transition to CT imaging can be life-saving when symptoms persist despite negative initial screens.
- Biopsy Gold Standards: The use of CD99 and other markers is essential in differentiating “small round blue cell tumors,” a group of cancers that look similar under a microscope but require different treatment paths.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The medical community continues to monitor the long-term outcomes of primary pulmonary Ewing sarcoma patients to determine if their prognosis differs significantly from those with traditional bone-based sarcoma. Future updates on pediatric oncology protocols and rare tumor registries will provide more data on the efficacy of current chemotherapy combinations for these specific pulmonary cases.
Do you have experience with rare diagnoses or questions about pediatric respiratory health? Share your thoughts in the comments or share this article to raise awareness.