As spring blossoms across the United States, millions of residents are finding that the beauty of the season comes with a significant physical toll. A surge in seasonal allergies is currently affecting a vast portion of the population, manifesting in the classic, disruptive symptoms of itchy eyes, persistent sneezing, and runny noses.
The scale of the impact is substantial, with health experts indicating that approximately 1 in 3 adults and 1 in 4 children are struggling with these allergic reactions. For many, these are not merely inconveniences but chronic conditions that can interfere with sleep, school performance, and overall daily productivity during the peak pollen months.
Managing these symptoms requires a combination of environmental awareness and medical intervention. Dr. Keedra McNeill, a pediatrician with Kaiser Permanente, emphasizes that families must take proactive steps to mitigate the impact of airborne allergens on children, whose immune systems may react more acutely to spring triggers.
Understanding the Biological Trigger
Seasonal allergies, often referred to as allergic rhinitis, occur when the immune system overreacts to harmless airborne substances, primarily pollen from trees, grasses, and weeds. When an allergen enters the nasal passage or eyes, the body releases histamine, a chemical that triggers the inflammation and mucus production associated with the “spring cold” feeling.
The timing of these surges often correlates with specific blooming cycles. Early spring is typically dominated by tree pollen, followed by grasses in late spring and early summer, and finally weeds like ragweed in the late summer and autumn. According to the American Academy of Allergy, Asthma & Immunology, the severity of a season can be influenced by weather patterns, where warm, windy days often lead to higher pollen counts in the air.
For those affected, the experience varies by demographic. While adults often manage symptoms with long-term medication, children may present with different signs, such as irritability or increased fatigue, which can sometimes be mistaken for a common cold or the flu.
Practical Strategies for Symptom Management
To reduce the burden of seasonal allergies, medical professionals recommend a multi-layered approach that focuses on both avoidance and treatment. Reducing the amount of pollen that enters the home and the body is the first line of defense.
Effective environmental controls include:
- Monitoring Pollen Counts: Checking local forecasts to avoid outdoor activities during peak pollen hours, which typically occur in the early morning and late afternoon.
- Creating “Safe Zones”: Keeping windows closed during high-pollen days and utilizing air conditioning with HEPA filters to scrub allergens from indoor air.
- Hygiene Rituals: Showering and changing clothes immediately after spending time outdoors to remove pollen trapped in hair and fabric.
- Nasal Irrigation: Using saline sprays or neti pots to physically rinse allergens from the nasal passages.
When environmental controls are insufficient, pharmacological options become necessary. Over-the-counter antihistamines, nasal corticosteroids, and decongestants are common choices. However, physicians caution against the prolonged use of certain nasal decongestant sprays, which can lead to a “rebound” effect, increasing congestion over time.
Comparing Common Allergy Treatments
| Treatment Type | Primary Function | Common Examples |
|---|---|---|
| Antihistamines | Blocks histamine receptors to stop itching/sneezing | Loratadine, Cetirizine |
| Corticosteroids | Reduces inflammation in the nasal passages | Fluticasone, Budesonide |
| Decongestants | Shrinks swollen nasal membranes to ease breathing | Pseudoephedrine, Oxymetazoline |
The Intersection of Allergies and Asthma
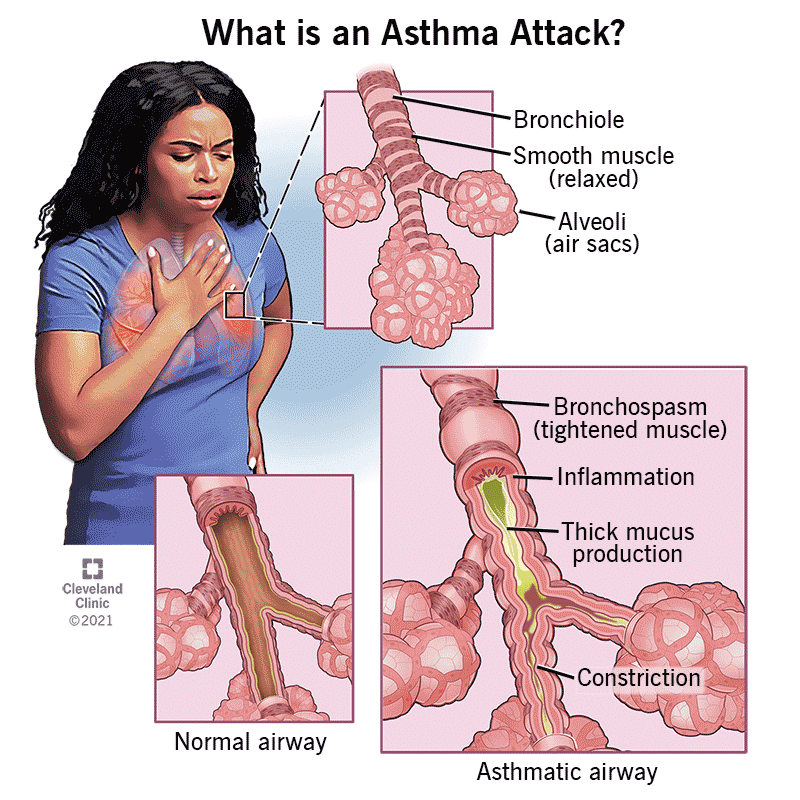
For a significant subset of the population, seasonal allergies are not limited to the upper respiratory tract. There is a strong correlation between allergic rhinitis and asthma, a condition often termed “allergic asthma.” In these cases, pollen can trigger bronchial inflammation, leading to wheezing, shortness of breath, and chest tightness.
The Centers for Disease Control and Prevention (CDC) notes that uncontrolled allergies can exacerbate asthma symptoms, making it critical for patients to maintain a coordinated treatment plan. This often involves using a “preventer” inhaler in conjunction with allergy medications to keep the airways open and responsive.
Pediatricians, including Dr. McNeill, highlight the importance of identifying these triggers early in childhood. When children are diagnosed early, they can be taught how to manage their environment, reducing the likelihood of severe respiratory distress during peak bloom periods.
When to Seek Professional Care
While many people manage their symptoms with drugstore remedies, certain indicators suggest that a visit to an allergist or primary care provider is necessary. If over-the-counter medications fail to provide relief, or if symptoms begin to affect the quality of sleep and daily functioning, professional intervention is warranted.

A board-certified allergist can provide skin-prick tests or blood tests to identify the specific triggers causing the reaction. This precision allows for a more tailored approach, such as prescription-strength medications or immunotherapy (allergy shots), which aims to desensitize the immune system to specific allergens over time.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As the spring season progresses, pollen levels will continue to fluctuate based on regional weather patterns and plant cycles. Public health officials and meteorological services will continue to provide updated pollen counts through the end of the bloom cycle, providing essential data for those managing their respiratory health.
Do you have a strategy that helps you get through allergy season? Share your experiences and tips in the comments below.

