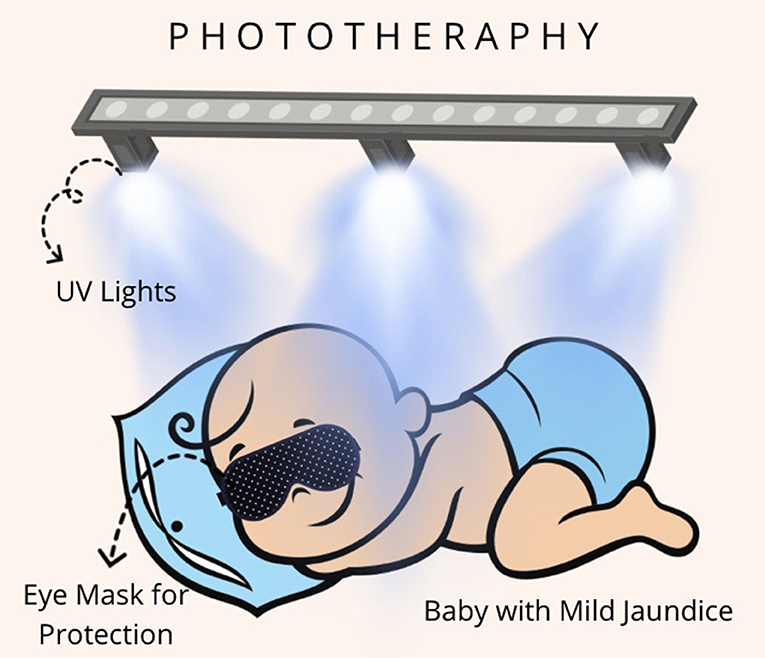
For generations, a common piece of anecdotal advice given to new parents has been to place a jaundiced newborn in a sunny windowsill to help “clear” the yellow tint from their skin. It seems like a gentle, natural solution—harnessing the power of the sun to treat a common neonatal condition. Although, recent clinical evidence suggests that using sunlight to treat newborn jaundice through window glass is not only ineffective but potentially misleading for parents seeking a cure.
The core of the issue lies in the physics of light and the chemistry of the newborn body. While sunlight does contain the wavelengths necessary to break down bilirubin—the yellow pigment responsible for jaundice—standard window glass acts as a sophisticated filter. By the time the light reaches a baby resting on a windowsill, the most therapeutic components have been stripped away, leaving the treatment useless while creating a false sense of security for caregivers.
As a physician, I have seen how these “home remedies” can delay necessary medical intervention. Neonatal jaundice, or neonatal hyperbilirubinemia, occurs when a baby’s liver is not yet efficient enough to remove bilirubin from the bloodstream. When levels climb too high, it is no longer a cosmetic concern but a medical one that requires precise, measured light therapy.
The science of the “glass barrier”
To understand why windows fail as a treatment tool, one must look at the light spectrum. Bilirubin is most effectively broken down by light in the blue-green spectrum, specifically wavelengths between 460 and 490 nanometers. This process, known as photoisomerization, changes the structure of the bilirubin molecule so it can be excreted more easily through the baby’s bile and urine.
While the sun emits a full spectrum of light, most modern window glass is designed to block ultraviolet B (UVB) rays and significantly attenuate other high-energy wavelengths to protect interiors from fading and humans from burns. The “sunbathing” that occurs behind a pane of glass lacks the intensity and the specific spectral power required to lower bilirubin levels in a clinically significant way.
This creates a dangerous gap in care. A parent may believe they are treating their child’s jaundice at home, while the bilirubin levels continue to rise undetected. Because the baby is not receiving the necessary dose of blue light, the condition remains untreated despite the appearance of “sunlight exposure.”
The risks of direct sunlight exposure
If window sunlight is ineffective, some might assume that moving the baby outside into direct sunlight is the logical alternative. However, medical professionals strongly advise against this practice due to the extreme vulnerability of newborn skin.
A newborn’s skin is significantly thinner and more permeable than that of an adult. Direct exposure to the sun poses several immediate risks:
- Thermal Regulation: Newborns cannot regulate their body temperature efficiently. Direct sun exposure can lead to rapid overheating or hyperthermia.
- Skin Burns: Because they lack mature melanin protection, infants are highly susceptible to severe sunburns, even during short periods of exposure.
- Dehydration: The heat from direct sun can increase insensible water loss, which may actually worsen jaundice by concentrating bilirubin in the blood.
In a clinical setting, phototherapy is delivered using specially calibrated LED or fluorescent lamps that emit only the necessary blue light spectrum without the heat or harmful UV radiation found in natural sunlight.
Comparing Light Therapy Methods
| Method | Effective Wavelengths | Safety Profile | Clinical Efficacy |
|---|---|---|---|
| Window Sunlight | Filtered/Insufficient | Low risk, but ineffective | Negligible |
| Direct Sunlight | Full Spectrum | High risk (burns/heat) | Variable/Uncontrolled |
| Clinical Phototherapy | Targeted Blue Light | High (Controlled) | Gold Standard |
When jaundice becomes a medical emergency
Most cases of newborn jaundice are mild and resolve on their own as the liver matures. However, when bilirubin levels reach critical thresholds, the pigment can cross the blood-brain barrier. This can lead to a permanent neurological condition known as kernicterus, which can cause cerebral palsy, hearing loss, and intellectual disabilities.
Because the progression of jaundice can be rapid, relying on unverified home treatments like windowsill exposure can be perilous. Parents should monitor for “warning signs” that indicate a need for immediate pediatric evaluation:
- The yellow color spreads to the abdomen, arms, or legs.
- The baby becomes excessively sleepy or difficult to wake.
- The baby is not feeding well or has a high-pitched cry.
Pediatricians use a tool called a transcutaneous bilirubinometer—a small device pressed against the baby’s skin—to obtain an instant reading of bilirubin levels. If the levels exceed the threshold established by the American Academy of Pediatrics, the infant is started on professional phototherapy immediately.
Moving toward evidence-based neonatal care
The transition from traditional “folk” remedies to evidence-based medicine is essential for infant safety. While the instinct to use the sun is rooted in a kernel of truth—that light does treat jaundice—the application of that truth must be precise. The difference between a windowpane and a medical-grade blue light is the difference between a placebo and a cure.

For parents today, the best course of action is to maintain frequent feedings, which help the baby pass bilirubin through stool, and to adhere strictly to the screening schedule recommended by their healthcare provider. If a physician suggests phototherapy, it should be performed using approved medical equipment, whether in the hospital or via a certified home-phototherapy rental system.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Medical guidelines for neonatal jaundice are periodically updated based on new clinical trials regarding bilirubin thresholds and the efficacy of various light-emitting diodes. Parents and caregivers should check with their pediatric clinic for the most current screening protocols for the current birth year.
Do you have experience with newborn jaundice or questions about neonatal care? Share your thoughts in the comments below or share this guide with new parents.